Diagnosis & Staging - The Scorecard
- Gold Standard: Liver Biopsy for fibrosis staging.
- Non-Invasive:
- Elastography (FibroScan) measures liver stiffness.
- Serum biomarkers (APRI, FIB-4).
- Prognostic Scores:
- Child-Pugh: Assesses 1-2 year survival. 📌 PAABE: PT/INR, Ascites, Albumin, Bilirubin, Encephalopathy.
- MELD-Na: Predicts 3-month mortality; prioritizes for transplant. Uses $f(\text{Bilirubin, INR, Creatinine, Na})$.
⭐ A MELD score >15 is a common threshold for liver transplant referral.
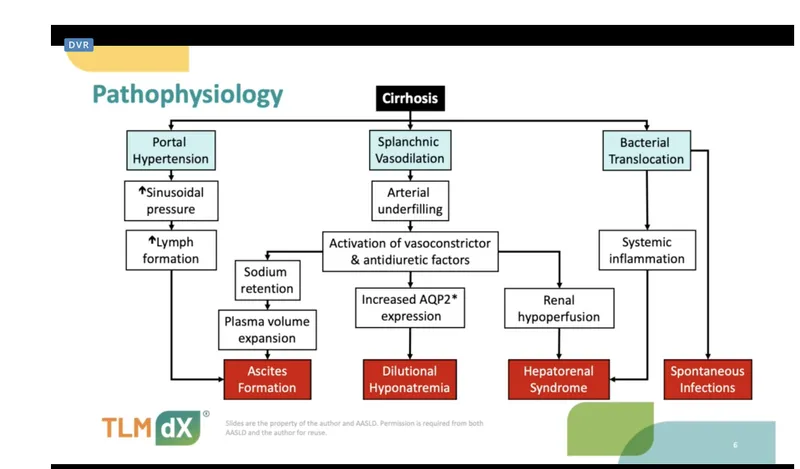
Decompensation Management - Leaky Pipes & Brain Fog
Ascites ("Leaky Pipes")
- Initial: Sodium restriction (<2 g/day) & diuretics.
- 📌 Mnemonic: Spironolactone to Furosemide ratio 100mg:40mg.
- Refractory Ascites:
- Large-Volume Paracentesis (LVP): Albumin infusion (6-8 g/L removed >5L).
- Transjugular Intrahepatic Portosystemic Shunt (TIPS).
- Spontaneous Bacterial Peritonitis (SBP):
- Treat with Ceftriaxone. Prophylaxis with Fluoroquinolones/TMP-SMX.
⭐ Spontaneous Bacterial Peritonitis (SBP) is diagnosed with an ascitic fluid absolute neutrophil count of >250 cells/mm³. Empiric treatment with a third-gen cephalosporin (e.g., Cefotaxime/Ceftriaxone) should be initiated immediately.
Hepatic Encephalopathy ("Brain Fog")
- Acute: Identify & treat precipitants (e.g., infection, GI bleed).
- Chronic:
- Lactulose: Titrate to 2-3 soft stools/day.
- Rifaximin: Add-on therapy if refractory.
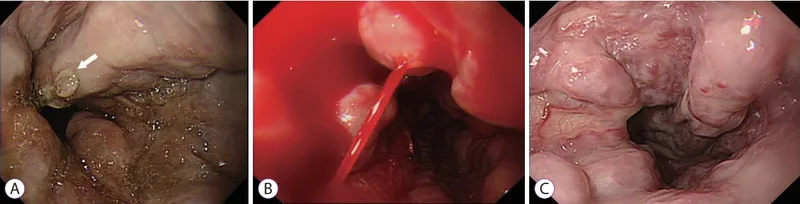
Varices & Bleeding - Code Red Protocol
- Immediate Steps: Secure airway (ABC); 2 large-bore IVs.
- Hemodynamic Support:
- Transfuse PRBCs if Hb <7 g/dL.
- IV fluids (crystalloids) for resuscitation.
- Pharmacotherapy:
- Octreotide (somatostatin analog) bolus then infusion to ↓ splanchnic blood flow.
- Prophylactic Antibiotics (e.g., Ceftriaxone) for 7 days.
- Urgent Endoscopy (EGD): Within 12 hours.
- Diagnosis & therapy (endoscopic variceal ligation/banding).
- Refractory Bleeding:
- Balloon Tamponade (Sengstaken-Blakemore tube) as a bridge.
- Transjugular Intrahepatic Portosystemic Shunt (TIPS) if endoscopy fails.
⭐ Prophylactic antibiotics (e.g., ceftriaxone) are critical, as they are proven to reduce mortality in acute variceal bleeds by preventing infections like SBP.
Long-Term Care - Surveillance & Solutions
- HCC Surveillance:
- Ultrasound (US) +/- Alpha-fetoprotein (AFP) every 6 months.
- Variceal Surveillance:
- EGD (esophagogastroduodenoscopy) at diagnosis.
- Repeat EGD every 1-2 years if varices are present, or 2-3 years if absent.
- Vaccinations:
- Hepatitis A & B series if not immune.
- Pneumococcal (PCV13, PPSV23), annual influenza.
- General Management:
- Abstain from alcohol.
- Avoid NSAIDs and other hepatotoxic drugs.
- Nutritional support to prevent malnutrition.
- Definitive Therapy:
- Liver transplantation is the only curative option.
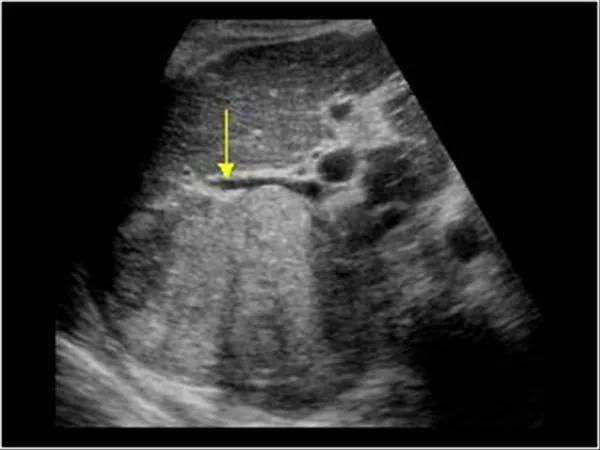
⭐ High-Yield Fact: Patients with cirrhosis who develop a new hepatic mass on ultrasound should undergo a triple-phase CT scan or MRI for definitive diagnosis of hepatocellular carcinoma (HCC). Biopsy is often deferred due to bleeding risk.
High‑Yield Points - ⚡ Biggest Takeaways
- Ascites is managed with sodium restriction and diuretics like spironolactone and furosemide.
- For Hepatic Encephalopathy, use lactulose and rifaximin; always correct the precipitating cause.
- Suspect SBP with ascitic fluid PMN > 250/mm³; treat with ceftriaxone.
- Acute variceal bleeding requires octreotide and endoscopic band ligation.
- Use non-selective beta-blockers like propranolol for variceal bleeding prophylaxis.
- Hepatorenal syndrome is treated with albumin, midodrine, and octreotide pending transplant.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

