Meningitis - Braincoat on Fire
- Classic Triad: Fever, nuchal rigidity, altered mental status (AMS).
- Physical Signs: Kernig's (pain on knee extension), Brudzinski's (neck flexion → hip/knee flexion).
- Etiology by Age:
- Neonate (<1 mo): GBS, E. coli, Listeria.
- Child/Adult: S. pneumoniae, N. meningitidis.
- >50 / Immunocompromised: Add Listeria coverage (Ampicillin).
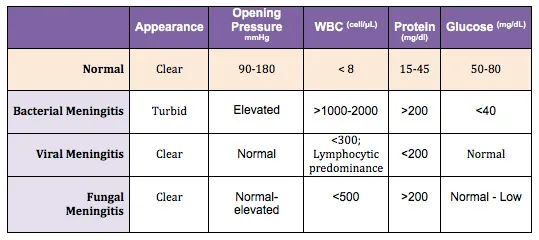
- CSF Findings:
- Bacterial: ↑↑WBC (Neutrophils), ↓Glucose (<40 mg/dL), ↑Protein, ↑Opening Pressure.
- Viral: ↑WBC (Lymphocytes), Normal Glucose, Normal/↑Protein.
- Fungal/TB: ↑WBC (Lymphocytes), ↓Glucose, ↑Protein.
⭐ Give dexamethasone 15-20 min before or with the first dose of empiric antibiotics to reduce neurological sequelae (esp. from S. pneumoniae).
Encephalitis - Gray Matter Mayhem
- Definition: Inflammation of the brain parenchyma, primarily affecting gray matter. Differentiated from meningitis by the presence of abnormal brain function (altered mental status, motor/sensory deficits, seizures).
- Etiology:
- Most common sporadic: Herpes Simplex Virus-1 (HSV-1).
- Epidemics: Arboviruses (e.g., West Nile Virus, St. Louis encephalitis).
- Diagnosis:
- MRI: Essential for localization.
- LP & CSF analysis: PCR for viral DNA is the gold standard.
- Treatment:
- Start IV Acyclovir empirically for any suspected case to cover for devastating HSV encephalitis.
⭐ High-Yield: HSV-1 encephalitis shows a classic predilection for the temporal lobes, leading to focal deficits like aphasia, seizures, or personality changes.
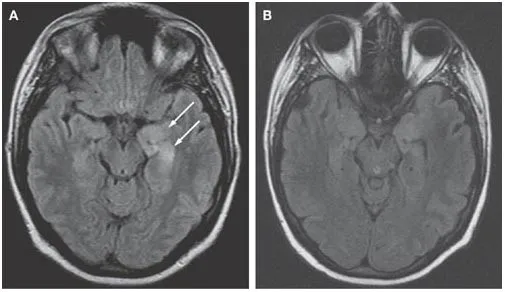
Brain Abscess - Pus in the Processor
- Etiology: Direct spread from sinusitis, otitis media, dental infection; hematogenous from endocarditis or lung infections.
- Pathogens: Streptococcus (esp. S. viridans, S. intermedius), Staphylococcus aureus, anaerobes (Bacteroides).
- Presentation: Headache is the most common symptom. The classic triad (headache, fever, focal deficits) is rare. Seizures are frequent.
- Diagnosis: Ring-enhancing lesion on CT/MRI with contrast. Restricted diffusion on DWI is key.
- Management: Aspiration/drainage + prolonged antibiotics (4-8 weeks) like ceftriaxone + metronidazole.
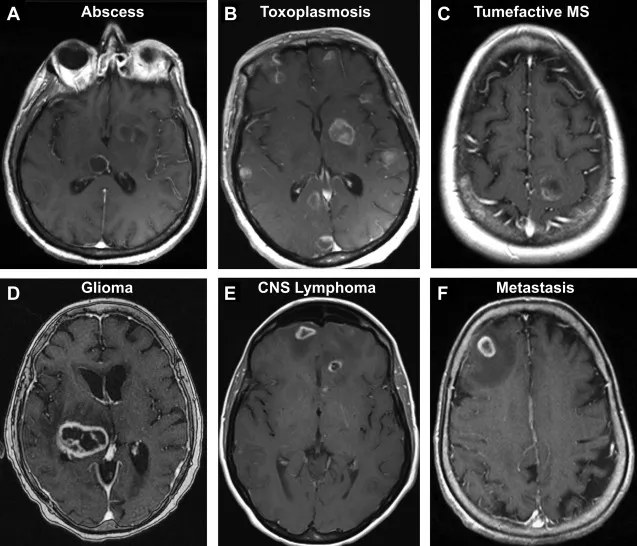
⭐ The central core of a bacterial abscess shows restricted diffusion on DWI MRI, helping to distinguish it from a necrotic tumor which typically does not.
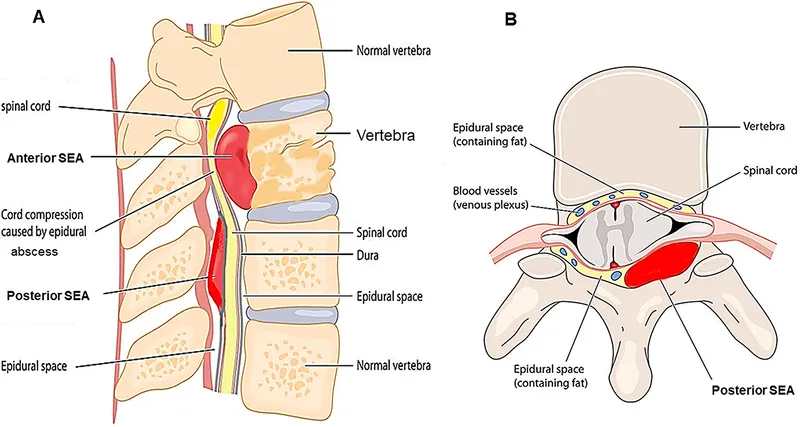
Spinal Epidural Abscess - Spine's Pus Pocket
- Patho: Pus collection in the epidural space, compressing the spinal cord.
- Risks: IV drug use, spinal procedures (e.g., epidural anesthesia), immunosuppression (diabetes), distant infection (e.g., skin).
- Classic Triad: 1. Fever, 2. Focal back pain, 3. Neurologic deficits.
- 📌 F-B-N Triad: Fever, Back pain, Neurologic deficits.
- Dx: MRI with gadolinium is the gold standard test.
- Tx: Urgent surgical decompression (laminectomy) + prolonged IV antibiotics (e.g., Vancomycin + Ceftriaxone).
⭐ Neurologic deficits can progress rapidly from radiculopathy to paralysis within hours to days; urgent diagnosis is critical.
High‑Yield Points - ⚡ Biggest Takeaways
- CSF analysis is key: bacterial meningitis has ↑ protein, ↓ glucose, and neutrophils. Viral meningitis has normal glucose and lymphocytes.
- Start empiric antibiotics (ceftriaxone, vancomycin) immediately after LP. Add ampicillin for extremes of age to cover Listeria.
- HSV-1 is the most common cause of fatal sporadic encephalitis, affecting the temporal lobes. Treat urgently with IV acyclovir.
- Cryptococcus neoformans causes meningitis in immunocompromised patients (CD4 < 100).
- N. meningitidis is linked to a petechial rash and outbreaks in close quarters (dorms, barracks).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

