Pathophysiology & Etiology - The Rusty Tank Runs Dry
Iron is a critical component of heme synthesis ($Fe^{2+}$ + Protoporphyrin → Heme). Insufficient iron impairs hemoglobin production, leading to microcytic, hypochromic anemia.
📌 Mnemonic LEAD for causes:
- Loss of blood (most common)
- Chronic GI bleeding (e.g., PUD, colon cancer) in men & postmenopausal women.
- Menorrhagia in premenopausal women.
- Exaggerated demand
- Pregnancy, lactation, adolescent growth spurts.
- Absorption poor
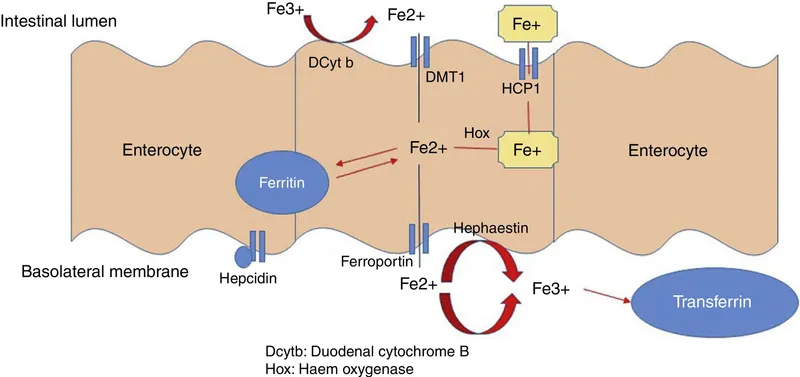
- Duodenum is the primary site of absorption.
- Celiac disease, gastrectomy, achlorhydria (e.g., PPI use).
- Diet inadequate
- Malnutrition, vegetarian/vegan diets.
⭐ Exam Favorite: Plummer-Vinson syndrome is a classic triad of dysphagia (esophageal webs), iron-deficiency anemia, and atrophic glossitis.
Clinical & Diagnosis - Pale, Tired, Spooned Nails
-
Symptoms: Fatigue, weakness, pallor (especially conjunctival), headache, dyspnea on exertion.
-
Specific Signs (Classic Triad):
- Koilonychia: Spoon-shaped nails.
- Glossitis: Atrophic, smooth, sore tongue.
- Angular Cheilitis: Fissures at mouth corners.
-
Pica: Craving for non-nutritive substances like ice (pagophagia), clay, or starch.
-
**Initial Labs (CBC):
- Microcytic, hypochromic anemia (↓ Hb, ↓ MCV < 80 fL, ↓ MCHC).
- ↑ RDW (Red Cell Distribution Width) is the earliest marker.
-
Confirmatory Iron Studies:
- ↓ Serum Ferritin (< 30 ng/mL is most specific).
- ↓ Serum Iron.
- ↑ TIBC (Total Iron-Binding Capacity).
- ↓ Transferrin Saturation (< 15%).
⭐ Plummer-Vinson Syndrome: Presents as a triad of dysphagia (due to esophageal webs), iron-deficiency anemia, and glossitis. It carries an increased risk for esophageal squamous cell carcinoma.
Management - Restocking the Iron Store
- Oral Iron (First-Line)
- Ferrous Sulfate: Standard dose is 325 mg (65 mg elemental iron) PO TID.
- Administer on an empty stomach or with Vitamin C (ascorbic acid) to ↑ absorption.
- Avoid with antacids, calcium, PPIs, or tetracyclines.
- Side effects: Constipation, black stools, nausea, epigastric distress.
- Parenteral Iron (IV/IM)
- Indications: Malabsorption (e.g., celiac, IBD), intolerance to oral Fe, or severe anemia requiring rapid correction.
- Formulations: Iron sucrose, ferric gluconate, iron dextran.
- ⚠️ Iron dextran carries a higher risk of anaphylaxis; a test dose is required.
⭐ Treatment Goal: Continue oral iron for 3-6 months after hemoglobin levels normalize to fully replenish body iron stores (target ferritin >50 ng/mL).
High‑Yield Points - ⚡ Biggest Takeaways
- Most common anemia, typically from chronic blood loss (GI bleed, menses) or dietary insufficiency.
- Classic signs include pica (ice craving), koilonychia (spoon nails), and atrophic glossitis.
- Key lab findings: ↓ ferritin is the most specific marker, ↑ TIBC, ↓ serum iron, and ↑ RDW.
- Blood smear reveals microcytic, hypochromic red cells.
- Consider Plummer-Vinson syndrome: triad of IDA, dysphagia, and esophageal webs.
- In older males/postmenopausal women, exclude GI malignancy as the underlying cause.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

