CRS Pathophysiology - The Vicious Cycle
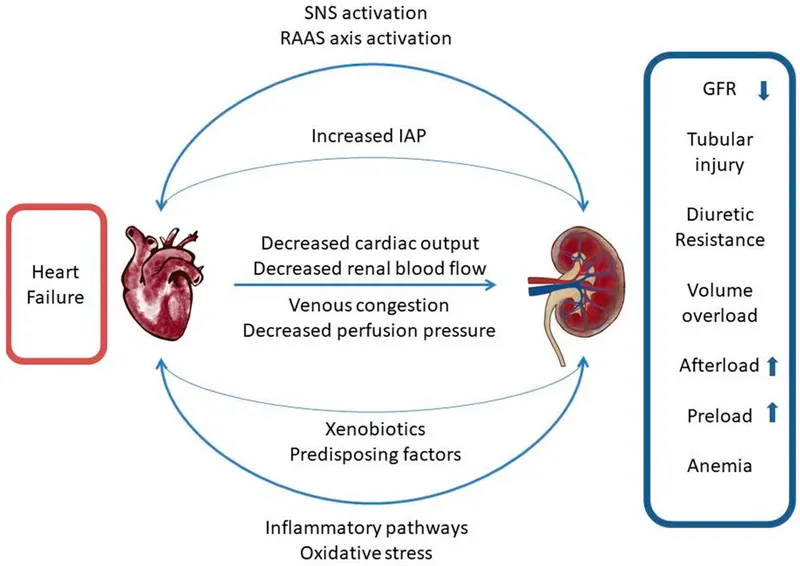
Cardio-Renal Syndrome (CRS) describes a bidirectional injury pathway where heart and kidney dysfunction amplify one another, creating a self-perpetuating cycle. The core mechanism involves hemodynamic and neurohormonal feedback loops.
- Hemodynamic Insults:
- ↓ Cardiac Output: Leads to renal hypoperfusion.
- ↑ Venous Congestion: Raises renal interstitial pressure, impairing glomerular filtration.
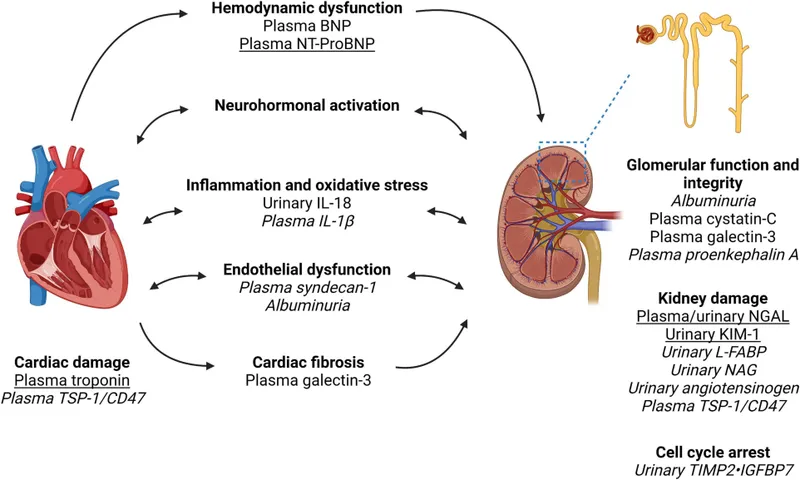
⭐ Exam Favorite: In acute decompensated heart failure, elevated central venous pressure (venous congestion) is a more potent predictor of worsening renal function than reduced cardiac index (forward failure).
CRS Classification - A Tale of Five Types
- Type 1 (Acute Cardiorenal): Acute Heart Failure (AHF) → Acute Kidney Injury (AKI).
- Example: Cardiogenic shock causing renal hypoperfusion.
- Type 2 (Chronic Cardiorenal): Chronic Heart Failure (CHF) → Chronic Kidney Disease (CKD).
- Mechanism: Long-term hypoperfusion, venous congestion, neurohormonal activation.
- Type 3 (Acute Renocardiac): AKI → Acute Cardiac Dysfunction.
- Example: AKI causing volume overload, hyperkalemia, or uremic pericarditis.
- Type 4 (Chronic Renocardiac): CKD → Chronic Cardiac Dysfunction.
- Mechanism: Leads to LVH, fibrosis, and accelerated atherosclerosis.
- Type 5 (Secondary): Systemic disorder → simultaneous heart & kidney dysfunction.
- Examples: Sepsis, diabetes, amyloidosis.
⭐ Type 2 is the most common form of CRS. The presence of renal dysfunction in chronic heart failure patients is a powerful independent predictor of mortality.
Diagnosis & Workup - Unmasking the Culprit
- Clinical Exam: Focus on volume overload: jugular venous distention (JVD), pitting edema, and pulmonary rales. Check for uremic signs like asterixis.
- Key Labs:
- ↑BUN/Cr (ratio >20:1), ↑BNP (>400 pg/mL).
- Hyperkalemia and metabolic acidosis are common.
- Urinalysis: May show bland sediment, granular casts (acute tubular necrosis), or proteinuria.
- Imaging:
- Echocardiogram: Evaluates cardiac structure and function.
- Renal Ultrasound: Excludes obstructive causes.
⭐ A bland urinalysis with few cells or casts is common in early CRS, pointing towards a hemodynamic rather than an intrinsic renal injury.
CRS Management - Damage Control
-
Core Challenge: Overcoming diuretic resistance in the setting of acute decompensated heart failure (ADHF) to achieve effective decongestion without worsening renal function.
-
Key Interventions:
- Pharmacologic: Start with IV loop diuretics. Add a thiazide for synergy. Use inotropes/vasodilators for hemodynamic instability.
- Mechanical: Ultrafiltration for refractory cases.
⭐ Exam Favorite: Continuous infusion of loop diuretics may be more effective and less ototoxic than intermittent boluses in patients with severe diuretic resistance.
High‑Yield Points - ⚡ Biggest Takeaways
- Cardio-Renal Syndrome (CRS) involves a vicious cycle of bidirectional injury between the heart and kidneys.
- Type 1 is acute heart failure causing acute kidney injury (AKI), often from ↓ cardiac output and ↑ venous congestion.
- Type 2 is chronic heart failure leading to progressive chronic kidney disease (CKD).
- Key lab findings include ↑ BUN and creatinine with worsening cardiac function.
- Management involves cautious diuresis and optimizing hemodynamics.
- Diuretic resistance is a hallmark of advanced CRS.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

