IBS Overview - The Gut Feeling
- Chronic, relapsing functional GI disorder characterized by abdominal pain and altered bowel habits without demonstrable organic pathology.
- Pathophysiology: Multifactorial, involving visceral hypersensitivity, altered gut motility, gut-brain axis dysregulation, and post-infectious changes.
- Diagnosis: Relies on clinical symptoms using Rome IV criteria:
- Recurrent abdominal pain on average at least 1 day/week in the last 3 months.
- Associated with ≥2 of the following: related to defecation, change in stool frequency, or change in stool form (appearance).
⭐ IBS is one of the most common GI disorders, predominantly affecting women and individuals < 50 years old. It is a diagnosis of exclusion.
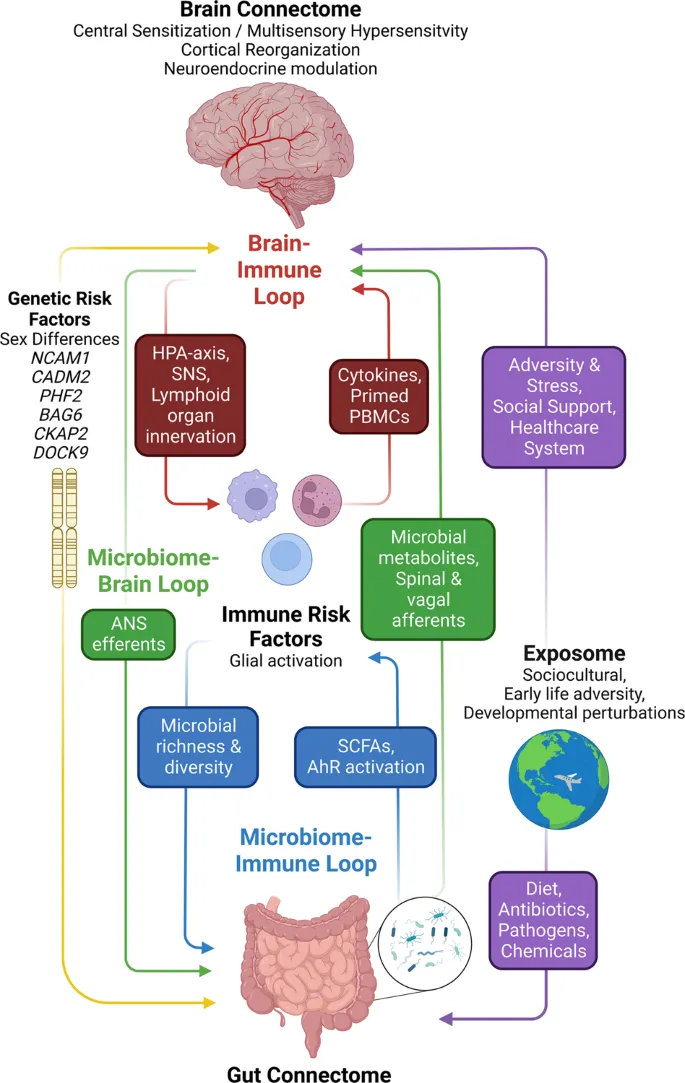
Pathophysiology - Gut-Brain Axis Glitch
- Core Defect: Bidirectional signaling failure between the central nervous system (CNS) and the enteric nervous system (ENS).
- Key Consequences:
- Visceral Hypersensitivity: Amplified pain signals from normal gut events (e.g., gas, peristalsis). The primary reason for abdominal pain.
- Altered Motility: Irregular gut contractions leading to diarrhea, constipation, or a mix.
- Immune Activation: Low-grade inflammation and mast cell activation.
- Microbiome Dysbiosis: Alterations in gut flora composition.
- Neurotransmitter Dysregulation: Primarily involving Serotonin (5-HT).
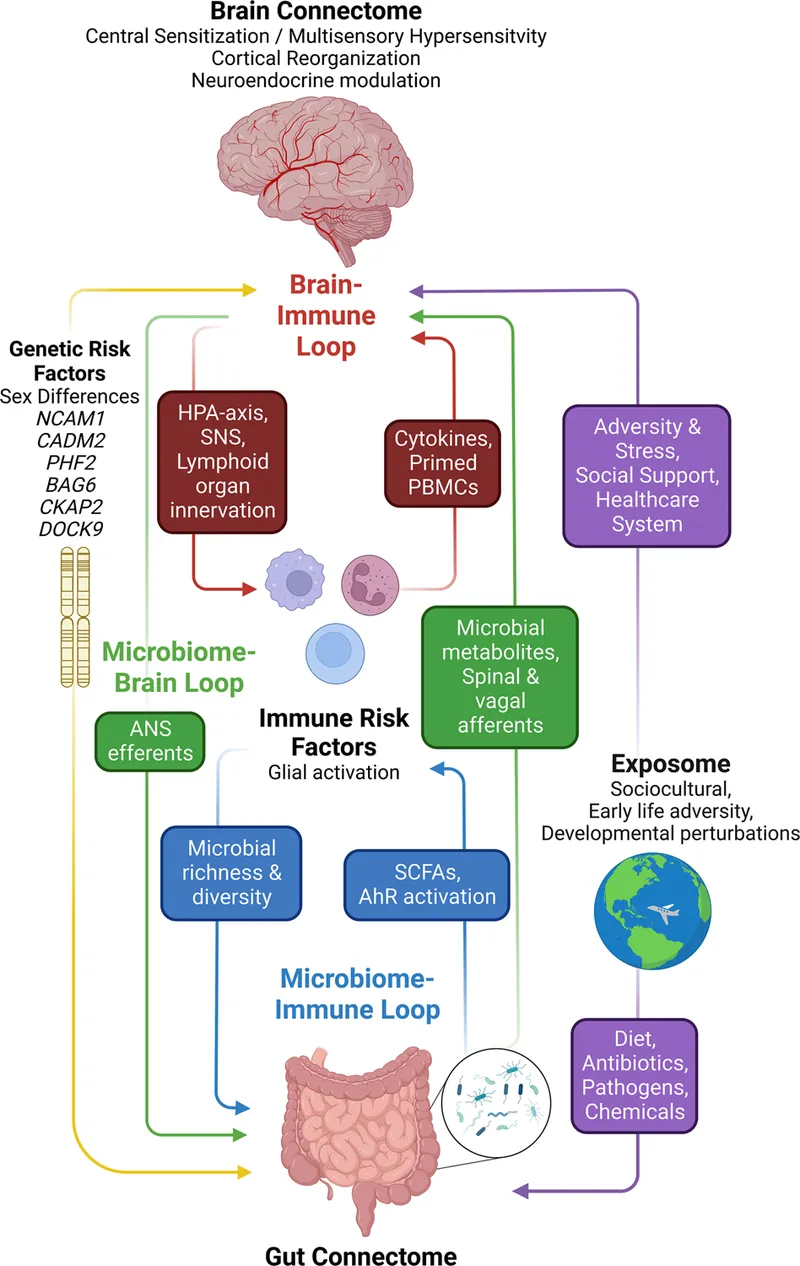
⭐ Post-infectious IBS (PI-IBS) can occur after acute gastroenteritis (e.g., Campylobacter), suggesting an autoimmune link where antibodies to microbial toxins cross-react with gut proteins like vinculin.
Diagnosis - The Rome Rules
Diagnosis of IBS is based on the Rome IV criteria, focusing on recurrent abdominal pain.
- Frequency: On average, at least 1 day/week in the last 3 months.
- Association: Pain must be associated with ≥2 of the following:
- Related to defecation
- Change in stool frequency
- Change in stool form (appearance)
- Chronicity: Criteria fulfilled for the last 3 months with symptom onset at least 6 months prior to diagnosis.
⭐ Absence of "alarm features" (e.g., rectal bleeding, nocturnal diarrhea, weight loss, anemia) is key to diagnosis. Their presence suggests organic disease requiring further investigation.
Management - Taming the Tumult
- Foundation: Patient education, stress reduction, and increased physical activity.
- Dietary: A trial of a low FODMAP diet is a cornerstone therapy. Avoid known trigger foods and excessive caffeine.
- Symptom-Guided Pharmacotherapy:
- IBS-C: Soluble fiber (psyllium), osmotic laxatives (PEG). For refractory cases, consider secretagogues like Lubiprostone.
- IBS-D: Loperamide for acute control. Rifaximin, a gut-specific antibiotic, can improve bloating and diarrhea.
- Pain/Bloating: Antispasmodics (e.g., dicyclomine) provide short-term relief.
⭐ For refractory IBS with severe pain, use central neuromodulators. Low-dose TCAs (amitriptyline) are ideal for IBS-D due to their constipating side effects.
- IBS is a functional disorder defined by chronic, relapsing abdominal pain related to defecation and altered bowel habits.
- Diagnosis relies on the Rome IV criteria after excluding organic causes; look for the absence of red flag symptoms like weight loss or bleeding.
- Key pathophysiology involves visceral hypersensitivity and altered gut-brain axis communication.
- Management is tailored to the predominant symptom: fiber for constipation (IBS-C) and loperamide for diarrhea (IBS-D).
- Psychosocial stressors frequently exacerbate symptoms.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

