CRC Basics - Why We Screen
- Goal: Detect & remove precancerous polyps (adenomas) to prevent progression to adenocarcinoma.
- Adenoma-Carcinoma Sequence: Slow, multi-step progression (mutations in APC, KRAS, p53) over ~10-15 years, creating a wide window for intervention.
- Epidemiology: 2nd leading cause of US cancer death. Most cases are sporadic.
- Key Risk Factors: Age >45, 1st-degree relative with CRC, IBD (UC > Crohn's), obesity.
⭐ Most CRCs arise from adenomatous polyps. Right-sided lesions often present with iron deficiency anemia; left-sided lesions cause changes in stool caliber.
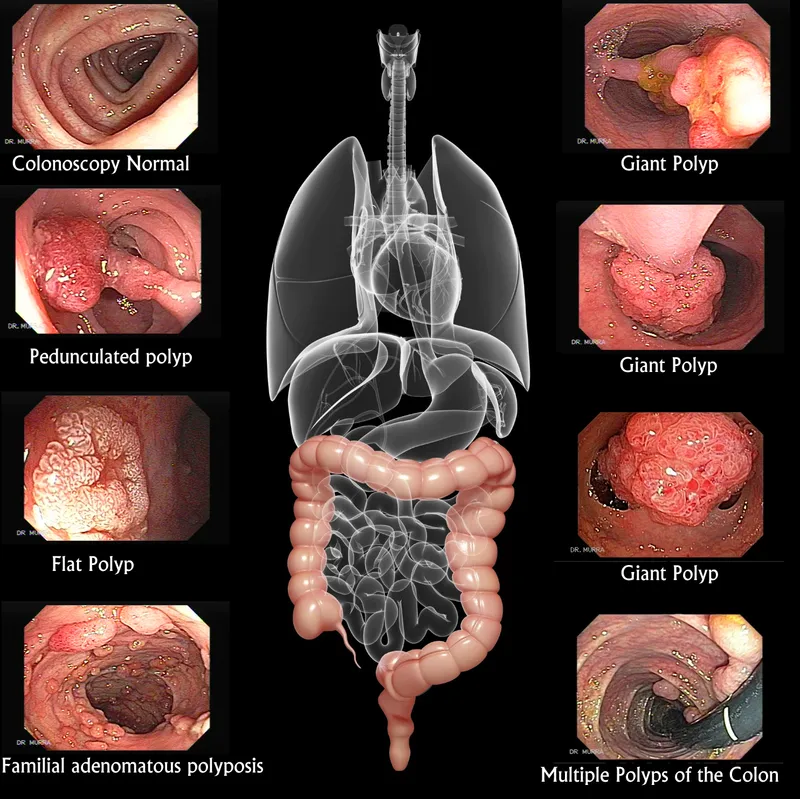
Screening Modalities - The Toolbox
A comparison of available CRC screening tests:
| Test | Frequency | Pros | Cons |
|---|---|---|---|
| Stool-Based | |||
| FIT | Annually | No prep, non-invasive | Lower sensitivity for polyps |
| gFOBT | Annually | Inexpensive | Low sensitivity/specificity, dietary restrictions |
| sDNA-FIT | Every 3 yrs | ↑ sensitivity for cancer vs. FIT | Expensive, ↑ false positives |
| Visual | |||
| Colonoscopy | Every 10 yrs | Gold standard; diagnostic & therapeutic | Invasive, full prep, sedation risk |
| CT Colonography | Every 5 yrs | Less invasive, no sedation | Prep needed, radiation, can't biopsy |
| Flex Sigmoidoscopy | Every 5 yrs | Less prep | Views only distal 1/3 of colon |
⭐ Exam Favorite: Unlike the guaiac-based FOBT (gFOBT), the Fecal Immunochemical Test (FIT) is specific for human globin and does not require dietary or medication restrictions (e.g., avoiding red meat, iron supplements, or vitamin C), leading to better patient adherence and fewer false positives.
Screening Algorithms - The Playbook
Routine screening for average-risk individuals begins at age 45 and continues until age 75. The decision to screen between ages 76-85 is individualized, weighing life expectancy and comorbidities. Screening is generally discontinued after age 85.
- Tier 1 (Prevent & Detect):
- Colonoscopy every 10 years.
- Tier 2 (Detection Only):
- Fecal Immunochemical Test (FIT) annually.
- Stool DNA-FIT (e.g., Cologuard) every 1-3 years.
- CT Colonography every 5 years.
- Flexible Sigmoidoscopy every 5 years.
⭐ Any positive non-colonoscopy screening test (FIT, Sigmoid, Cologuard) must be followed by a diagnostic colonoscopy to be considered a complete screening.
High-Risk Groups - The Exceptions
- Family Hx (CRC/Advanced Adenoma):
- FDR <60y: Scope at 40y or 10y before diagnosis, q5y.
- FDR ≥60y: Scope at 40y, q10y.
- Inflammatory Bowel Disease (UC/Crohn's):
- Scope 8 years post-pancolitis dx, q1-2y with biopsies.
- Genetic Syndromes:
- FAP: Sigmoidoscopy @ 10-12y.
- Lynch (HNPCC): Colonoscopy @ 20-25y, q1-2y.
⭐ In IBD, surveillance requires extensive random biopsies (e.g., 4-quadrant every 10 cm) as dysplasia can be flat and invisible.
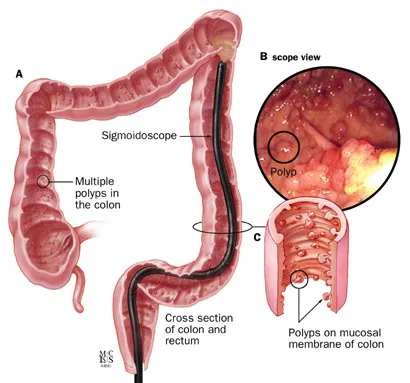
High‑Yield Points - ⚡ Biggest Takeaways
- Average-risk colorectal cancer screening now begins at age 45.
- Colonoscopy every 10 years is the preferred screening strategy; annual FIT is the best non-invasive test.
- For a first-degree relative with CRC diagnosed at <60 years, start screening at age 40 or 10 years before the relative's diagnosis.
- Lynch syndrome and FAP are high-risk conditions requiring much earlier and more frequent surveillance.
- Screening is generally discontinued after age 75.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

