Pathophysiology - Clogged Pipes 101
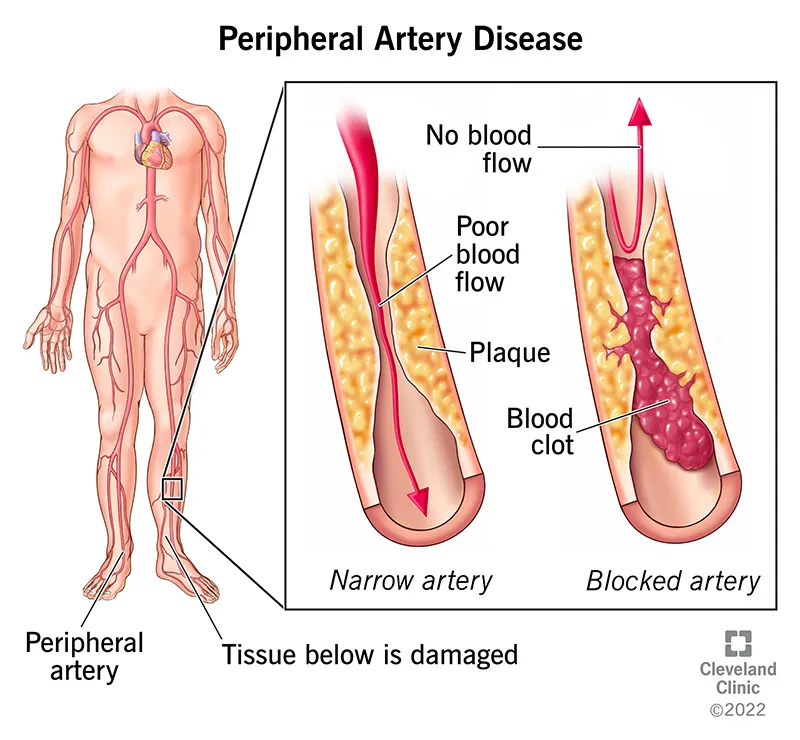
- Atherosclerosis is the primary cause, leading to stenosis or occlusion.
- Major Risk Factors: Smoking (strongest), Diabetes Mellitus, Hyperlipidemia, Hypertension.
- Process: Endothelial injury → lipid deposition (LDLs) → foam cell & plaque formation → narrowed lumen → ↓ blood flow (ischemia).
- Most Common Sites: Superficial femoral artery (SFA) in Hunter's canal, followed by the popliteal artery.
⭐ Leriche Syndrome Triad (Aortoiliac occlusion):
- Bilateral hip, thigh, and buttock claudication
- Impotence
- Symmetric atrophy of the bilateral lower extremities.
Clinical Features - The Leg's Complaint
- Intermittent Claudication: Reproducible muscle pain (calf, thigh, buttock) on exertion, promptly relieved by rest.
- Rest Pain: Severe, nocturnal forefoot pain, relieved by dependency (hanging foot off bed). A key feature of Critical Limb Ischemia (CLI).
- Physical Signs:
- Shiny, atrophic skin with hair loss.
- Dependent rubor and elevation pallor.
- Cool skin; diminished or absent pulses.
- Tissue Loss (Advanced Disease):
- Arterial Ulcers: Deep, "punched-out," painful lesions on distal toes or pressure points.
- Gangrene.
⭐ The location of arterial ulcers (e.g., tips of the toes, pressure points) is a key differentiator from venous ulcers (typically over the medial malleolus).
Diagnosis - Checking the Flow
- Ankle-Brachial Index (ABI): Best initial, non-invasive test.
- Calculated as $ABI = \frac{\text{Highest Ankle SBP}}{\text{Highest Brachial SBP}}$.
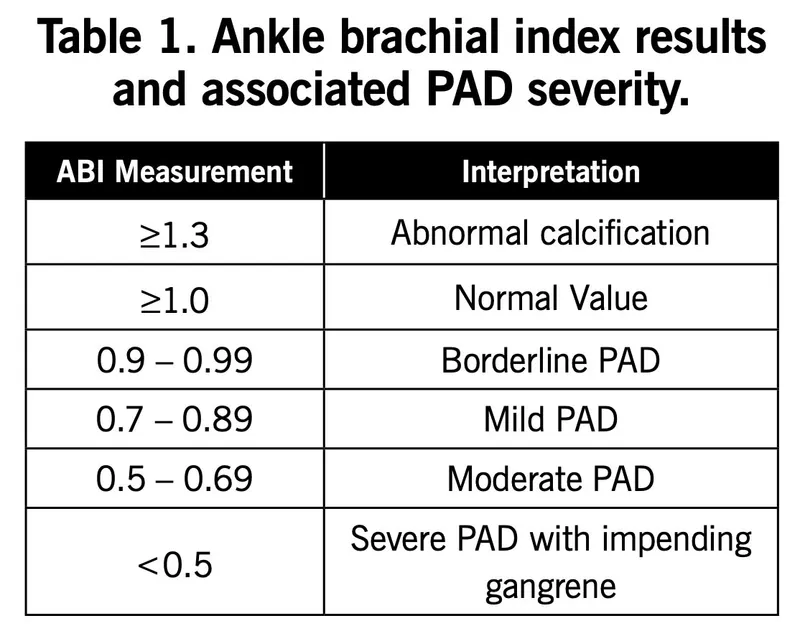
- Interpretation:
- < 0.9: Diagnostic of PAD.
- < 0.4: Severe disease / Critical Limb Ischemia (CLI).
- > 1.4: Calcified, non-compressible vessels (e.g., advanced age, diabetes).
⭐ An Ankle-Brachial Index (ABI) of <0.9 is the simple, non-invasive, first-line test for diagnosing PAD.
- Imaging:
- Doppler US: Localizes lesions.
- CTA/MRA: Gold standard for anatomical detail before revascularization.
Management - Restoring the Rush
⭐ A supervised exercise program is a highly effective, first-line intervention for intermittent claudication that can improve symptoms and walking distance significantly.
-
Conservative Management
- Risk Factor Modification: Smoking cessation is paramount. Also manage HTN, DM, HLD.
- Supervised Exercise Therapy: Walk until near-maximal claudication pain, rest, repeat.
-
Medical Management
- Antiplatelet Therapy: Aspirin or Clopidogrel to reduce MI/stroke risk.
- Statins: All patients with PAD should be on a statin, regardless of LDL level.
- Cilostazol: Phosphodiesterase inhibitor; most effective medical therapy for claudication symptoms.
-
Surgical Intervention
- Revascularization: For limb-threatening ischemia or debilitating, refractory symptoms.
- Percutaneous: Angioplasty ± Stenting
- Surgical: Bypass grafting (e.g., fem-pop)
- Amputation: For non-salvageable limbs (gangrene, intractable pain).
- Revascularization: For limb-threatening ischemia or debilitating, refractory symptoms.
High-Yield Points - ⚡ Biggest Takeaways
- Atherosclerosis of the lower extremities is the primary cause, most commonly affecting the superficial femoral artery.
- Intermittent claudication is the hallmark symptom: reproducible leg pain with exertion that is relieved by rest.
- An Ankle-Brachial Index (ABI) < 0.9 is the main screening and diagnostic test.
- Cilostazol is the most effective medical therapy specifically for claudication symptoms.
- Aspirin and statins are critical for reducing cardiovascular risk, including MI and stroke.
- Critical limb ischemia presents as rest pain, non-healing arterial ulcers, or gangrene.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

