Indications & Basics - Why We Need Wires
-
Core Problem: Failure of the heart's intrinsic conduction system, leading to symptomatic bradycardia or risk of sudden cardiac death (SCD) from tachyarrhythmias. Pacemakers provide a safety net; ICDs provide a shock.
-
Pacing for Bradycardia:
- Symptomatic sinus node dysfunction ("sick sinus syndrome").
- High-grade AV block: Mobitz II, Third-degree (complete) AV block.
- Symptomatic bradycardia post-MI or drugs.
-
ICD for Tachycardia:
- Primary Prevention: Cardiomyopathy with LVEF ≤ 35%.
- Secondary Prevention: History of survived SCD due to VT/VF.
⭐ For primary prevention, an ICD is indicated in HF patients with LVEF ≤ 35% on optimal medical therapy for >3 months, at least 40 days post-MI.
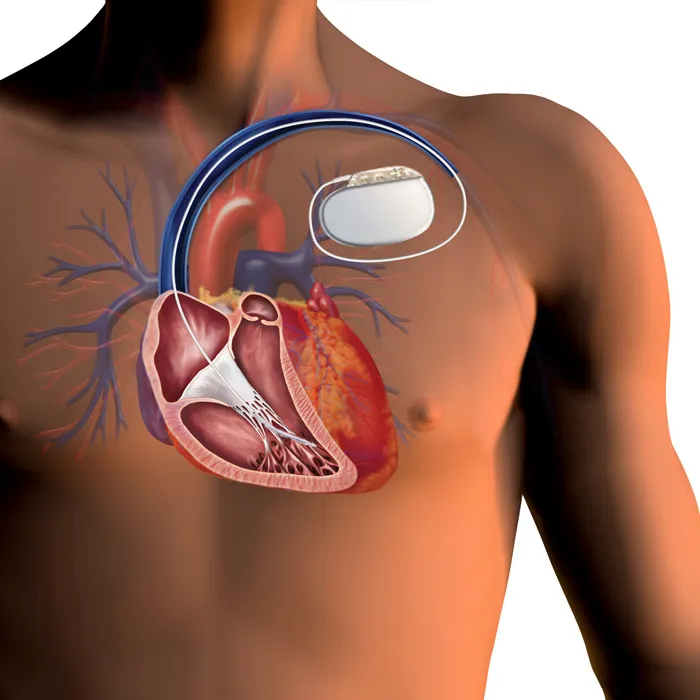
Device Types & Pacing Codes - Alphabet Soup of Pacing
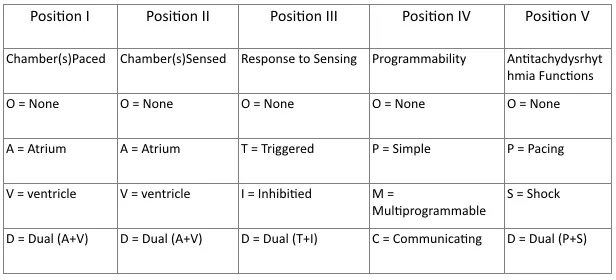
- Device Types
| Device | Core Function | Key Indication(s) |
|---|---|---|
| Pacemaker (PPM) | Bradycardia treatment | Symptomatic bradycardia, high-degree AV block |
| ICD | Terminates tachyarrhythmias | Primary/secondary prevention of sudden cardiac death |
| CRT | Resynchronizes ventricles | Heart failure (EF ≤35%), LBBB with wide QRS |
- 📌 **P**aced, **S**ensed, **R**esponse: Position I, II, III.
⭐ Magnet Application: Placing a magnet over an ICD disables its antitachycardia functions (shocking/ATP), but does not affect its pacemaker function. In a pacemaker, a magnet induces an asynchronous pacing mode (e.g., VOO/DOO).
ECG Findings - Reading the Pacer Spikes
- Pacer Spike: A sharp, vertical line on the ECG indicating pacemaker discharge.
- Spike Location & Morphology:
- Atrial Pacing: Spike before the P wave.
- Ventricular Pacing: Spike before a wide QRS complex (often LBBB-like).
- Dual-Chamber (AV Sequential): Spikes appear before both the P wave and QRS complex.
- Capture: Each pacer spike is followed by the expected electrical event (P wave or QRS). Failure to capture means the stimulus was insufficient.
- Sensing: The pacemaker correctly inhibits firing when it detects an intrinsic beat.
⭐ Placing a magnet over a pacemaker usually forces it into a fixed-rate, asynchronous pacing mode, overriding its sensing function. This helps assess battery status and capture function without interference from the patient's intrinsic rhythm.
Complications & Management - When Good Wires Go Bad
- Lead Complications:
- Dislodgement/Fracture: Most common early issue. Leads to failure to sense or capture. Seen on CXR.
- Perforation: Can cause chest pain, hiccups (phrenic nerve stimulation), or pericardial effusion.
- Pocket Issues:
- Infection/Erosion: Erythema, pain, drainage. Requires entire system explant & antibiotics.
- Twiddler’s Syndrome: Patient manipulation of generator causes lead dislodgement.
- ICD-Specific:
- Inappropriate Shocks: Often due to SVT (like AFib) misidentified as VT. Manage underlying arrhythmia; reprogram device.
⭐ Device Infection Management: Superficial infection may be treated with antibiotics, but any evidence of deeper pocket or device infection necessitates removal of the entire pacemaker/ICD system (generator and leads).
- Pacemakers are for symptomatic bradycardia (e.g., 3rd-degree AV block, sick sinus syndrome).
- ICDs are for primary prevention (HFrEF with EF <35%) and secondary prevention (post-VT/VF arrest).
- A magnet over a pacemaker causes asynchronous pacing (AOO/VOO/DOO).
- A magnet over an ICD disables shock therapy but does not affect pacing.
- Failure to capture shows pacer spikes not followed by a QRS or P-wave.
- Failure to sense occurs when the pacemaker doesn't detect intrinsic cardiac activity.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

