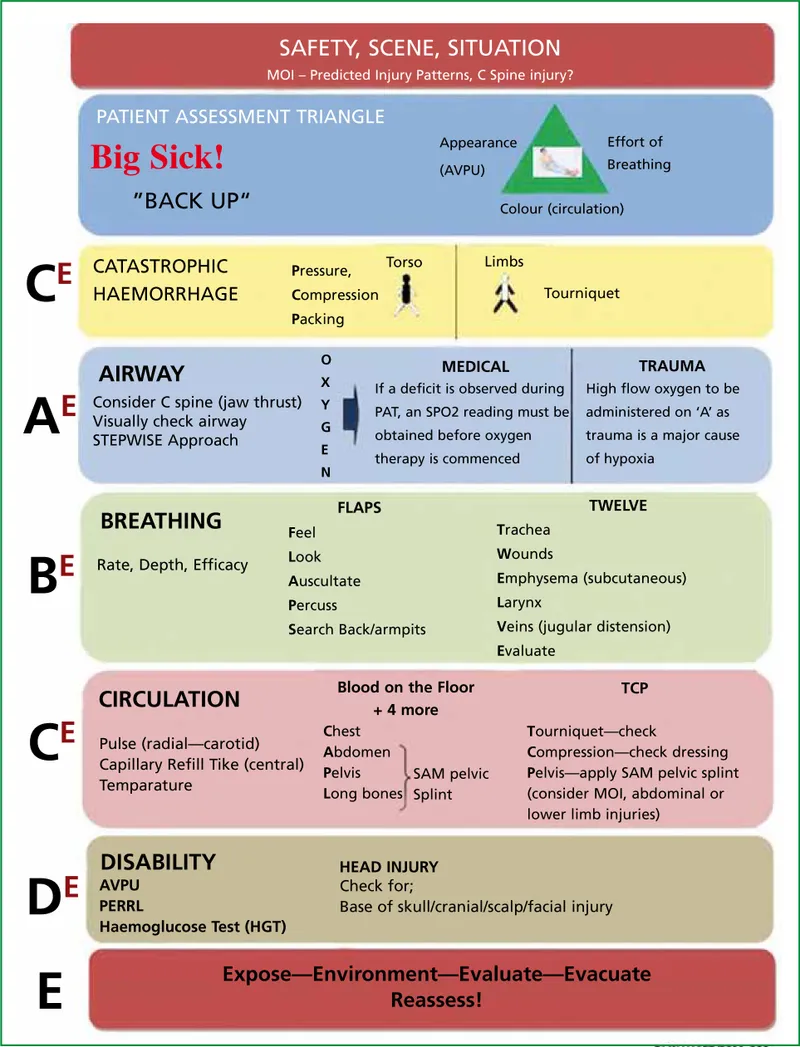
Primary Survey - The ABCDE Lifesaver
- A rapid, systematic approach to assess and treat life-threatening conditions sequentially. Address any identified issue before proceeding to the next letter.
- A - Airway: Check for patency. Use jaw-thrust for suspected C-spine injury.
- B - Breathing: Assess respiratory rate, effort, SpO₂. Provide high-flow O₂ for SpO₂ < 94%.
- C - Circulation: Check pulse, BP, CRT (<2s). Stop major bleeding. Secure 2 large-bore IV cannulas.
- D - Disability: Assess GCS/AVPU, pupillary response, and blood glucose.
- E - Exposure: Fully undress the patient to examine for injuries, then cover to prevent hypothermia.
⭐ A Glasgow Coma Scale (GCS) score of ≤ 8 is a strong indication for definitive airway management (intubation).
Cardiovascular Crises - Code Blue Conditions
Immediate recognition of shockable vs. non-shockable rhythms is critical. Prioritize high-quality CPR and early defibrillation.
- CPR: Rate 100-120/min, depth 5-6 cm. Minimize interruptions.
- Reversible Causes (H's & T's):
- Hypovolemia, Hypoxia, Hydrogen ion (acidosis), Hypo/Hyperkalemia, Hypothermia.
- Tension pneumothorax, Tamponade, Toxins, Thrombosis (pulmonary/coronary).
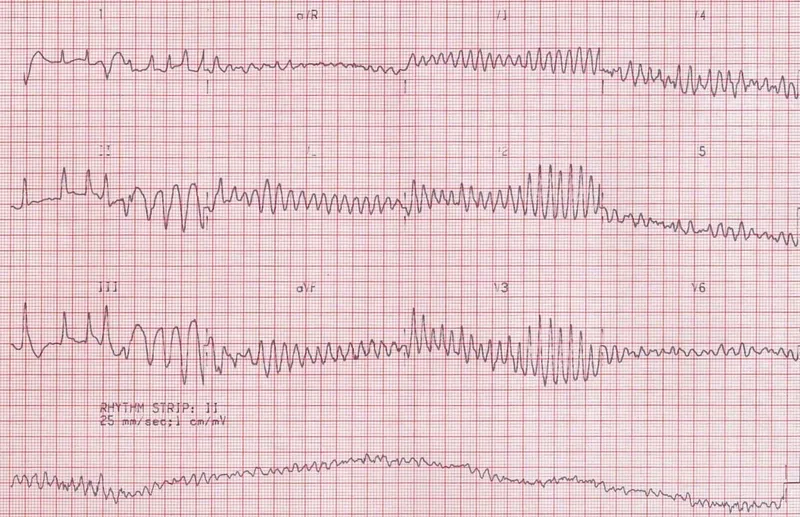
⭐ For pulseless electrical activity (PEA), the focus is high-quality CPR and aggressively searching for/treating the reversible H's & T's, as the electrical system is functional but there is no mechanical capture.
Respiratory Red Alerts - Can't-Breathe Catastrophes
-
Immediate Action Triggers: Stridor, cyanosis, use of accessory muscles, respiratory rate >30 or <8, SpO2 <90% on high-flow O₂, altered mental status.
-
Key Conditions & Classic Signs:
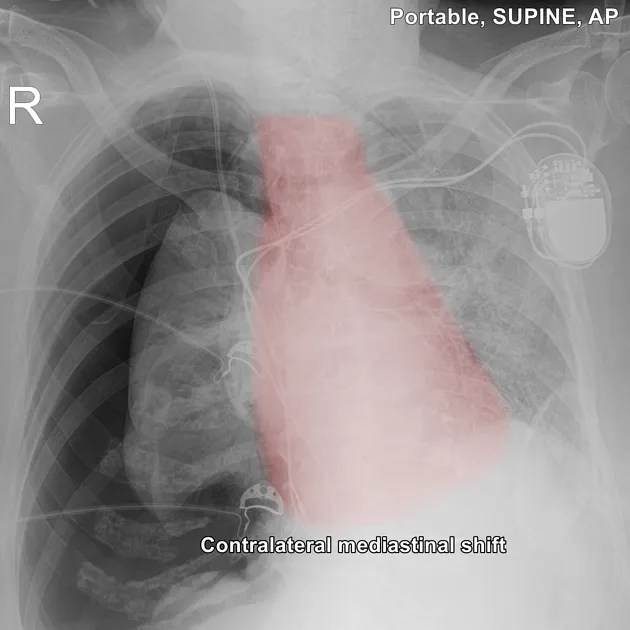
- Tension Pneumothorax: Unilateral absent breath sounds, hyper-resonance, tracheal deviation (late sign). Immediate needle decompression.
- Massive Hemoptysis: >600 mL/24h or >100 mL/h. Position patient bleeding-side down.
- Flail Chest: Paradoxical chest movement from trauma (≥3 adjacent ribs fractured in ≥2 places).
- Airway Obstruction: Stridor, dysphonia, drooling (epiglottitis), angioedema.
⭐ A "silent chest" in a severe asthma exacerbation signals impending respiratory failure due to minimal airflow; it is a pre-arrest finding.
Neurological Emergencies - Brain Attack Alerts
- Time is Brain: Immediate recognition is crucial to salvage the ischemic penumbra.
- 📌 Mnemonic BE-FAST: Balance loss, Eyes (vision loss), Face droop, Arm weakness, Speech difficulty, Time to activate emergency response.
- Initial Actions: Secure ABCs, check blood glucose (critical mimic), establish IV access.
- Key Goal: Door-to-needle time for thrombolysis < 60 minutes.

⭐ Hypoglycemia (< 60 mg/dL) is the most important stroke mimic to rule out immediately, as it is easily reversible and can present with identical focal neurological deficits.
High‑Yield Points - ⚡ Biggest Takeaways
- Always assess Airway, Breathing, Circulation (ABC) first; any compromise is the highest priority.
- Recognize airway obstruction: listen for stridor or gurgling. Intubate if GCS ≤ 8.
- Identify breathing failure: watch for respiratory rate >30 or <8, or SpO2 <90%.
- Spot circulatory shock: check for SBP <90 mmHg, tachycardia, and altered mental status.
- Altered Mental Status (AMS) is a critical sign of cerebral hypoxia or hypoperfusion.
- The first step for any unstable patient is to move to ICU/ER and administer oxygen.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

