Core Ethical Principles - The Moral Compass
- Beneficence: The duty to act in the patient's best interest. Aims to promote well-being, prevent illness, and alleviate suffering.
- Non-maleficence: Primum non nocere - "First, do no harm." Obligation to avoid causing unnecessary pain or disability. The cornerstone of medical ethics.
- Autonomy: Respecting the patient's right to make informed decisions about their own body and healthcare, including the right to refuse treatment.
- Justice: Ensuring fair and equitable distribution of healthcare resources and treatment. Treat similar cases with similar care, avoiding bias.
📌 Mnemonic: Remember the 4 Pillars with B-A-N-J (Beneficence, Autonomy, Non-maleficence, Justice).
⭐ Principle of Double Effect: An act with both a good and a bad outcome (e.g., morphine for palliation which may hasten respiratory depression) is ethically permissible if the intended effect is good and the bad effect is foreseen but unintended.

Triage & Justice - High-Stakes Prioritizing
-
Core Principle: Justice (fair allocation of scarce resources). In emergencies, this shifts from individual-focused care to community-focused, utilitarian goals.
-
Ethical Pillars in Triage:
- Beneficence: Do maximum good for the largest number of people.
- Non-maleficence: Avoid harm; don't expend limited resources on futile cases.
- Distributive Justice: Fairly distribute resources (beds, ventilators, staff time).
- Procedural Justice: Use a consistent, transparent, and unbiased process for decision-making.
-
Triage Categories & Action:
⭐ Exam Favourite: The primary ethical justification for triage during mass casualty events is utilitarianism - aiming to produce the greatest good for the greatest number, which means prioritizing patients who are likely to survive with immediate intervention over those with a very poor prognosis.
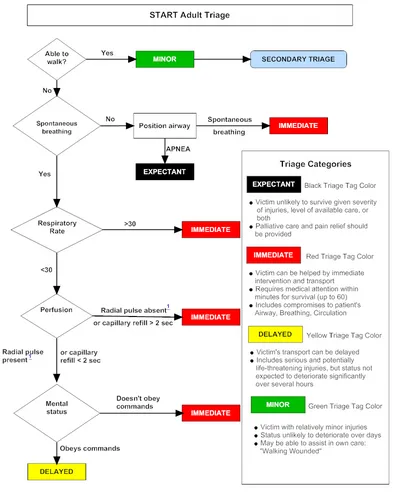
- Avoidance of Improper Criteria: Decisions must NOT be based on social status, wealth, connections, or perceived social worth. Age or disability should only be considered if they directly impact prognosis.
Consent & Confidentiality - Patient Rights Playbook
-
Informed Consent: A voluntary decision made by a competent patient based on adequate information. Core pillars are voluntariness, information, and capacity.
- Types:
- Implied: Inferred from actions (e.g., extending arm for injection). Crucial in emergencies under the Doctrine of Necessity.
- Express: Stated orally or in writing for specific interventions.
- 📌 BRAIN Mnemonic for Consent Elements:
- Benefits of treatment.
- Risks involved.
- Alternatives available.
- Implications of refusing.
- Nature of the procedure.
- Types:
-
Confidentiality: A doctor's legal and ethical duty to not disclose information obtained from a patient without their consent.
- Exceptions: Permissible to breach when there is a risk of serious harm to others, required by law (court order, notifiable diseases), or with patient consent.
⭐ Tarasoff Principle: A landmark legal case establishing a "duty to protect." If a patient makes a credible threat of violence against a specific person, confidentiality may be breached to warn the potential victim.
High-Yield Points - ⚡ Biggest Takeaways
- Patient autonomy is paramount; always obtain informed consent before any intervention.
- Balance the principles of beneficence (acting for patient good) and non-maleficence (avoiding harm).
- Apply distributive justice for fair allocation of scarce resources, like ICU beds or ventilators.
- Uphold patient confidentiality and dignity at all times.
- Adherence to ICMR ethical guidelines is mandatory in the Indian context.
- Carefully consider the futility of treatment in terminally ill patients to avoid unnecessary suffering.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

