Test Selection Principles - The First Crucial Step
- Pre-test Probability (PTP): The estimated likelihood of a disease before performing a test, based on patient history, exam, and prevalence. It's the cornerstone of Bayesian reasoning in medicine.
- Test Purpose Dictates Choice:
- Screening: Detects potential disease in asymptomatic individuals (e.g., Pap smear). Applied to populations with low PTP.
- Diagnostic: Confirms or refutes a diagnosis in symptomatic individuals (e.g., biopsy). Used in high PTP settings.
- Monitoring: Tracks disease progression or treatment response (e.g., HbA1c).
⭐ As Pre-test Probability increases, the Positive Predictive Value (PPV) of a test also increases, while the Negative Predictive Value (NPV) decreases.
Diagnostic Test Metrics - Decoding the Numbers
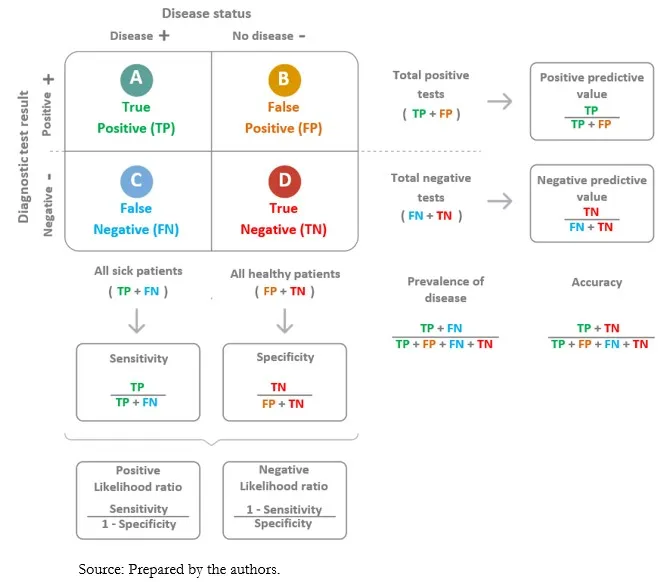
| Disease Present | Disease Absent | |
|---|---|---|
| Test +ve | True Positive (TP) | False Positive (FP) |
| Test -ve | False Negative (FN) | True Negative (TN) |
- $Sensitivity = \frac{TP}{TP + FN}$
- Specificity: Ability to correctly identify those without the disease.
- $Specificity = \frac{TN}{TN + FP}$
- 📌 Mnemonic: SPIN (Specific test, when Positive, rules IN) & SNOUT (Sensitive test, when Negative, rules OUT).
- Positive Predictive Value (PPV): Probability that a patient with a positive test truly has the disease.
- $PPV = \frac{TP}{TP + FP}$
- Negative Predictive Value (NPV): Probability that a patient with a negative test is truly disease-free.
- $NPV = \frac{TN}{TN + FN}$
- Prevalence affects predictive values:
- ↑ Prevalence → ↑ PPV, ↓ NPV
⭐ Sensitivity and Specificity are intrinsic properties of a test and are not affected by the prevalence of the disease in the population.
Likelihood Ratios & ROC - Odds, Ends, and Curves
-
Likelihood Ratios (LRs) quantify how much a test result changes the certainty of a diagnosis.
- Positive LR (LR+): $ \frac{Sensitivity}{1 - Specificity} $. How much to increase the odds of disease given a positive test.
- Negative LR (LR-): $ \frac{1 - Sensitivity}{Specificity} $. How much to decrease the odds of disease given a negative test.
- Clinical application via odds: $Post-test odds = Pre-test odds \times LR$.
- Interpretation: LR+ > 10 or LR- < 0.1 provide strong evidence.
-
Receiver Operating Characteristic (ROC) Curve:
- Plots Sensitivity (True Positive Rate) vs. 1 - Specificity (False Positive Rate).
- Area Under the Curve (AUC) measures overall diagnostic accuracy.
- AUC = 1: Perfect test.
- AUC = 0.5: Useless (chance).
- AUC > 0.8: Good test.

⭐ Likelihood Ratios are more robust than predictive values as they are not significantly affected by disease prevalence.
High‑Yield Points - ⚡ Biggest Takeaways
- Always start with screening tests (high sensitivity) before using confirmatory tests (high specificity).
- Test selection is guided by pre-test probability; high probability may warrant a more specific initial test.
- Likelihood Ratios (LRs) are clinically superior; seek Positive LR >10 and Negative LR <0.1 for strong evidence.
- Never treat the report; always correlate lab findings with the clinical picture.
- Avoid the "shotgun approach"-order tests sequentially and logically.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

