Pathophysiology - Brain Under Siege
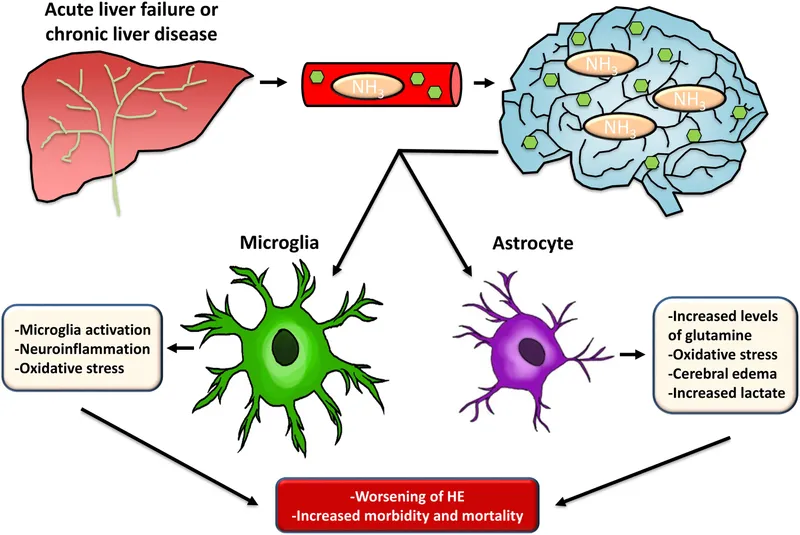
- Ammonia ($NH_3$) readily crosses the blood-brain barrier, overwhelming astrocyte detoxification capacity.
- Key Reactions in Astrocytes:
- $NH_3 + \alpha-ketoglutarate \rightarrow Glutamate$
- $Glutamate + NH_3 \rightarrow Glutamine$
- Consequences:
- ↓ α-ketoglutarate: Depletes TCA cycle intermediates → ↓ ATP production.
- ↑ Glutamine: Acts as an osmolyte, causing astrocyte swelling, cerebral edema, and ↑ intracranial pressure.
- Neurotransmitter imbalance: ↓ Glutamate (excitatory) and altered GABAergic tone.
⭐ In hyperammonemia, the accumulation of glutamine within astrocytes is the key factor causing osmotic stress, leading to cerebral edema and subsequent neurological damage.
Etiologies - The Usual Suspects
| Cause Category | Specifics & High-Yield Points |
|---|---|
| Congenital | Urea Cycle Enzyme Deficiencies: - Ornithine Transcarbamylase (OTC) Deficiency: Most common. Causes ↑ orotic acid in blood & urine. - Citrullinemia (Argininosuccinate Synthase deficiency) - Argininosuccinic Aciduria (Argininosuccinate Lyase deficiency) |
| Acquired | Advanced Liver Disease: Cirrhosis is the most frequent cause in adults. Drugs: Valproate, asparaginase. Increased Nitrogen Load: GI bleed, high-protein diet, infection/sepsis (catabolism). |
⭐ Ornithine Transcarbamylase (OTC) deficiency is the sole X-linked recessive urea cycle disorder. Excess carbamoyl phosphate is shunted to pyrimidine synthesis, causing orotic aciduria.
Clinical Presentation - Ammonia's Aftermath
- Neurotoxicity (Encephalopathy): Ammonia is a potent neurotoxin, primarily affecting the CNS.
- Early: Blurring of vision, slurred speech, drowsiness, confusion.
- Classic Sign: Asterixis (flapping tremor of outstretched hands).
- Late: Lethargy, seizures, coma, death from cerebral herniation.
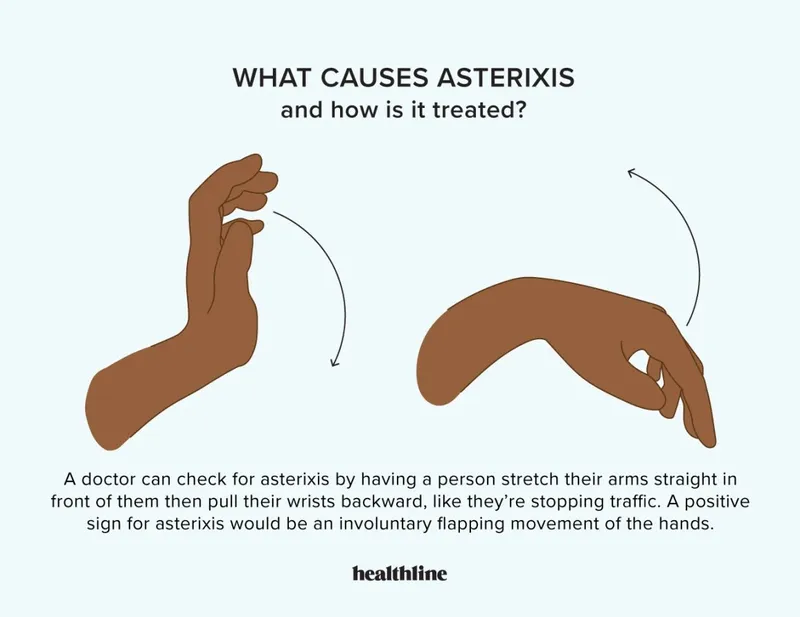
- Mechanism of Toxicity:
⭐ Hyperammonemia depletes α-ketoglutarate in the brain by shunting it towards glutamate/glutamine synthesis. This inhibits the TCA cycle, critically reducing ATP production in astrocytes and impairing neuronal function.
- Systemic Effects: Nausea, vomiting, and hyperventilation leading to respiratory alkalosis.
Diagnosis & Management - The Damage Control
-
Initial Workup:
- Labs: ↑ Plasma ammonia >150 µmol/L (asterixis, coma), LFTs, ABG (respiratory alkalosis).
- Urine Orotic Acid: Differentiates OTC deficiency (↑) from CPS1 deficiency (↓).
-
Management Strategy:
- Pharmacotherapy:
- Gut: Lactulose (traps $NH_3$ as $NH_4^+$), Rifaximin (↓ urease-producing bacteria).
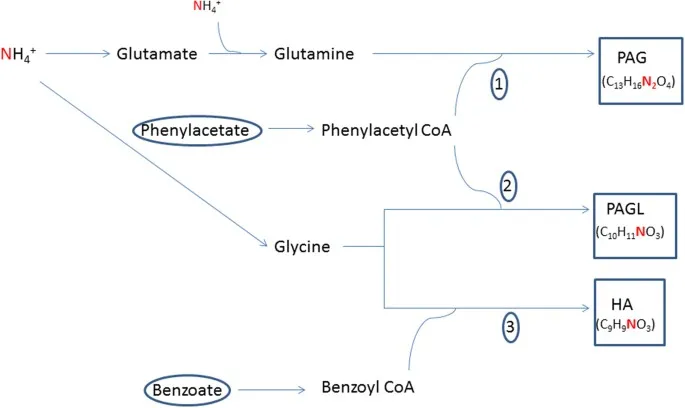
- Systemic (Scavengers): Sodium Benzoate, Sodium Phenylacetate.
⭐ Cerebral Edema: The primary cause of death in acute hyperammonemia is brain herniation from astrocyte swelling due to excess glutamine. Rapid ammonia reduction is critical.
High‑Yield Points - ⚡ Biggest Takeaways
- Hyperammonemia most commonly results from liver failure (acquired) or urea cycle enzyme deficiencies (genetic).
- Ornithine transcarbamylase (OTC) deficiency, an X-linked recessive disorder, is the most common urea cycle defect.
- Excess ammonia (NH₃) depletes α-ketoglutarate, impairing the TCA cycle and causing neurotoxicity.
- Clinical signs include asterixis (flapping tremor), slurred speech, vomiting, and cerebral edema.
- Labs show ↑ blood ammonia and glutamine; orotic aciduria is characteristic of OTC deficiency.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

