LSDs - Cellular Trash Cans
- Core Defect: Inherited mutations causing deficient or absent lysosomal enzymes, the cell's recycling centers.
- Mechanism: Failure to degrade complex macromolecules (e.g., sphingolipids, mucopolysaccharides).
- Pathology: Leads to toxic accumulation of undigested substrates within lysosomes, causing cellular swelling and progressive organ damage (hepatosplenomegaly, neurodegeneration).
⭐ Most LSDs are autosomal recessive. Key exceptions are Fabry disease (X-linked recessive) and Hunter syndrome (X-linked recessive).
Sphingolipidoses - Fatty Buildup
- Inherited deficiencies of enzymes for sphingolipid metabolism.
- Most are autosomal recessive, except for Fabry disease (X-linked recessive).
| Disease | Deficient Enzyme | Accumulated Substrate | Key Features |
|---|---|---|---|
| Tay-Sachs | Hexosaminidase A | $GM2$ ganglioside | Cherry-red spot; NO hepatosplenomegaly; onion skin lysosomes. |
| Fabry | α-galactosidase A | Ceramide trihexoside | Peripheral neuropathy; angiokeratomas; renal failure. |
| Metachromatic Leukodystrophy | Arylsulfatase A | Cerebroside sulfate | Central & peripheral demyelination; ataxia; dementia. |
| Krabbe | Galactocerebrosidase | Galactocerebroside | Peripheral neuropathy; optic atrophy; globoid cells. |
| Gaucher | Glucocerebrosidase | Glucocerebroside | Hepatosplenomegaly; pancytopenia; bone crises; crumpled tissue paper cells. |
| Niemann-Pick | Sphingomyelinase | Sphingomyelin | Hepatosplenomegaly; cherry-red spot; foam cells. |
⭐ Gaucher disease is the most common lysosomal storage disease, characterized by "crumpled tissue paper" macrophages on bone marrow biopsy.
📌 Mnemonic: No man picks his nose with his sphinger (Niemann-Pick, Sphingomyelinase).
Mucopolysaccharidoses - Sugar Mess
-
Group of inherited metabolic disorders caused by the absence or malfunctioning of lysosomal enzymes needed to break down glycosaminoglycans (GAGs).
-
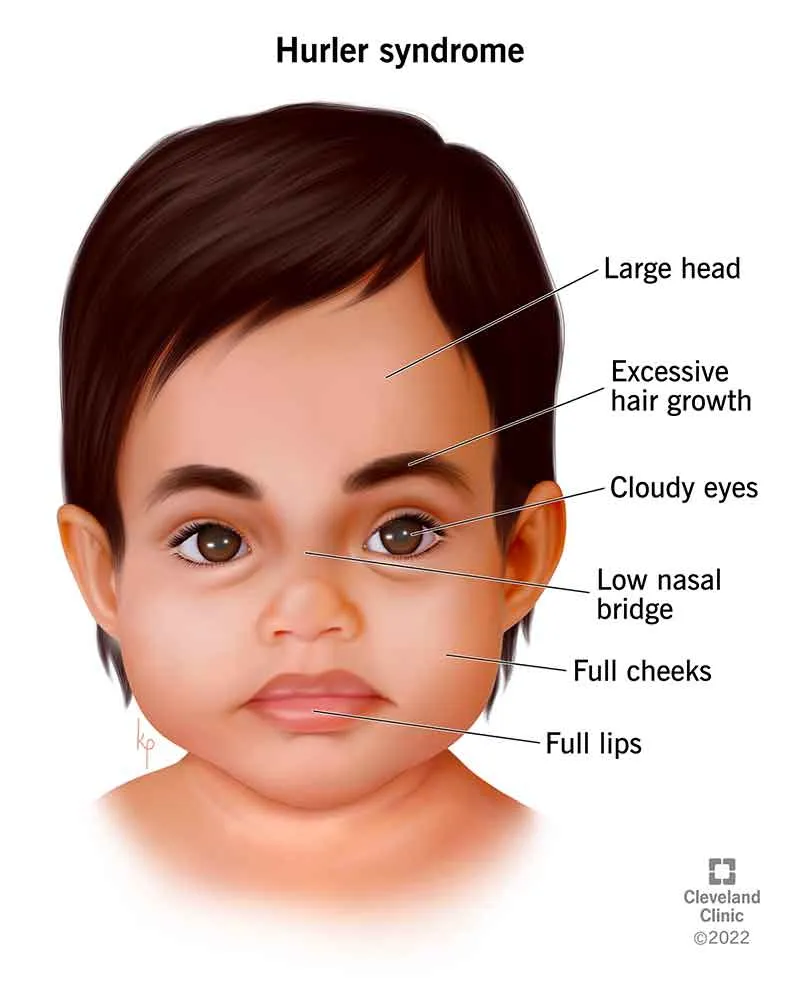
Hurler Syndrome (MPS I)
- Deficiency: α-L-iduronidase.
- Accumulation: Heparan & dermatan sulfate.
- Features: Corneal clouding, gargoylism, dysostosis multiplex, developmental delay.
- Inheritance: Autosomal Recessive.
-
Hunter Syndrome (MPS II)
- Deficiency: Iduronate-2-sulfatase.
- Accumulation: Heparan & dermatan sulfate.
- Features: No corneal clouding, aggressive behavior, mild to severe physical & intellectual disability.
⭐ Hunter syndrome is X-linked recessive, a key distinguishing feature from most other autosomal recessive lysosomal storage diseases.
📌 Mnemonic: Hunters see clearly (no corneal clouding) and aim for the X (X-linked).
Diagnosis & Management - Lab Sleuthing
- Primary Test: Direct measurement of specific enzyme activity in leukocytes or cultured fibroblasts is the gold standard.
- Confirmatory: Genetic testing for specific gene mutations confirms the diagnosis and is vital for carrier detection and prenatal counseling.
- Management Principles:
- Enzyme Replacement Therapy (ERT): Mainstay for many LSDs (e.g., Gaucher, Fabry).
- Substrate Reduction Therapy (SRT): Inhibits synthesis of the accumulating substrate.
- Hematopoietic Stem Cell Transplant (HSCT): For certain mucopolysaccharidoses (e.g., Hurler syndrome).
⭐ Enzyme Replacement Therapy (ERT) infusions do not cross the blood-brain barrier, limiting efficacy for neurological symptoms.
High‑Yield Points - ⚡ Biggest Takeaways
- Most are autosomal recessive, except for the X-linked Fabry and Hunter diseases.
- Tay-Sachs and Niemann-Pick both present with a "cherry-red" macula, but hepatosplenomegaly is absent in Tay-Sachs.
- Gaucher disease is the most common, featuring massive hepatosplenomegaly and "crinkled paper" macrophages.
- Fabry disease is characterized by peripheral neuropathy, angiokeratomas, and eventual renal failure.
- Hunter syndrome (X-linked) is distinguished from Hurler by the absence of corneal clouding and presence of aggressive behavior.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

