Pathophysiology & Genetics - The Lazy Liver Enzyme
- Genetic Defect: Autosomal recessive mutation in the PYGL gene.
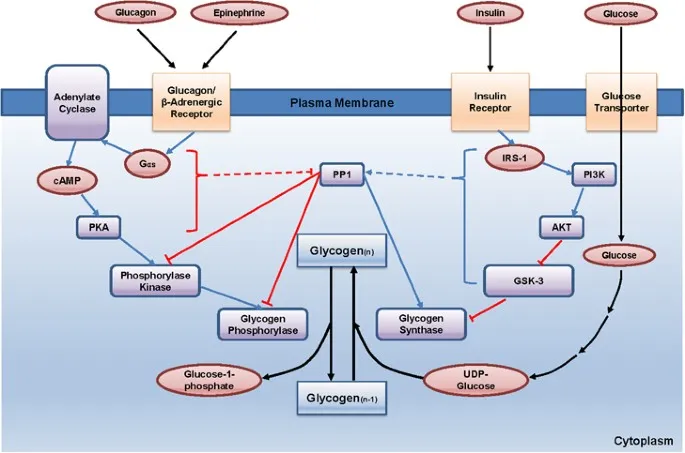
- Enzyme Deficiency: Results in deficient liver glycogen phosphorylase, the rate-limiting enzyme for hepatic glycogenolysis.
- Pathophysiology: The liver's inability to properly break down glycogen leads to:
- ↑ Glycogen accumulation → Hepatomegaly
- ↓ Glucose release during fasting → Mild hypoglycemia
⭐ Exam Pearl: Symptoms often improve with age. The enzyme is deficient or "lazy," not completely absent, leading to a milder phenotype compared to other GSDs. Many patients become asymptomatic by puberty.
📌 Mnemonic: Hers disease = Hepatic Phosphorylase Deficiency & Hepatomegaly.
Clinical Presentation - Big Liver, Mild Trouble
Error generating content for this concept group: Invalid JSON response
Diagnosis - Finding the Faulty Fuel-Tap
- Lab Findings:
- Mild post-absorptive hypoglycemia & ketosis.
- ↑ Hyperlipidemia.
- ↑ Serum transaminases (AST, ALT).
- Key Negative Findings (Differentiators):
- NORMAL blood lactate.
- NORMAL uric acid.
⭐ Unlike GSD I (von Gierke disease), blood lactate levels remain NORMAL in Hers disease because gluconeogenesis is unaffected.
Management & Prognosis - Starch & Steady Wins
- Primary Goal: Maintain normoglycemia & prevent hypoglycemia, especially during fasting.
- Dietary Therapy:
- Frequent, small meals rich in complex carbohydrates.
- High-protein diet to provide substrates for gluconeogenesis.
- ⚠️ Avoid large boluses of simple sugars.
- Key Intervention: Administration of uncooked cornstarch (a slow-release glucose source), especially nocturnally or before anticipated fasts.
- Prognosis:
- Generally very good.
- Hepatomegaly, growth retardation, and hypoglycemia often improve with age and can resolve spontaneously after puberty.
⭐ Hers disease spares the muscle. Unlike McArdle disease (GSD V), patients do not experience exercise intolerance or rhabdomyolysis.
High-Yield Points - ⚡ Biggest Takeaways
- Deficient enzyme: Liver glycogen phosphorylase, leading to impaired glycogenolysis.
- Inheritance: Autosomal recessive.
- Key features: Hepatomegaly, growth retardation, and mild fasting hypoglycemia.
- Labs: Normal blood lactate and uric acid levels, distinguishing it from GSD I.
- Ketosis is present during fasting due to intact fatty acid oxidation.
- Prognosis: Generally mild, with symptoms often improving with age.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

