Pathophysiology - Faulty Glycogen Branches
- Enzyme Defect: Deficiency of the glycogen branching enzyme (amylo-α-1,4→α-1,6-transglucosidase).
- Genetic Basis: Autosomal recessive mutation in the GBE1 gene.
- Abnormal Glycogen Structure:
- Fewer branches and long outer chains, creating an amylopectin-like structure.
- This abnormal glycogen has ↓ decreased solubility, causing it to precipitate in tissues.
- Cellular Injury:
- Insoluble glycogen deposits (polyglucosan bodies) act as foreign bodies.
- Triggers a host immune response, leading to fibrosis, and ultimately organ failure (e.g., progressive liver cirrhosis).
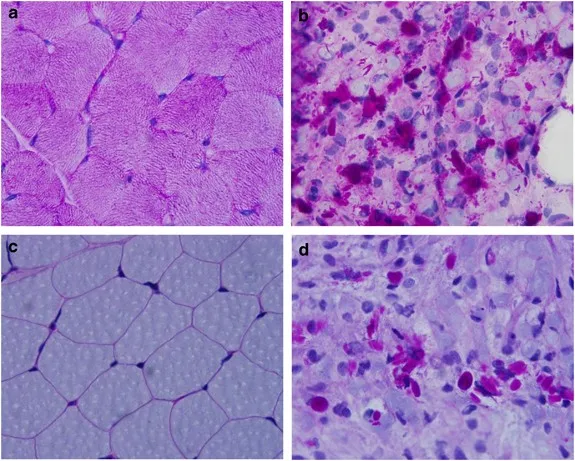
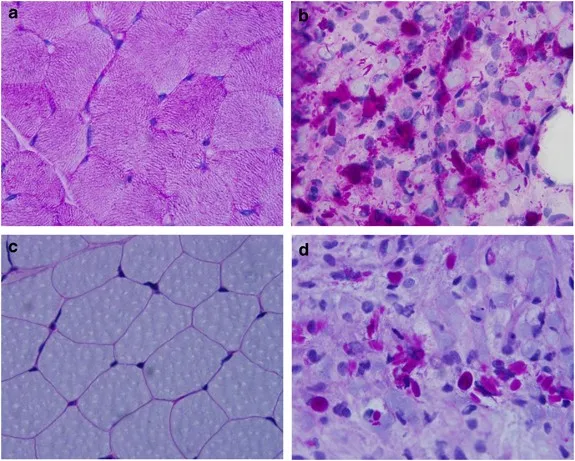
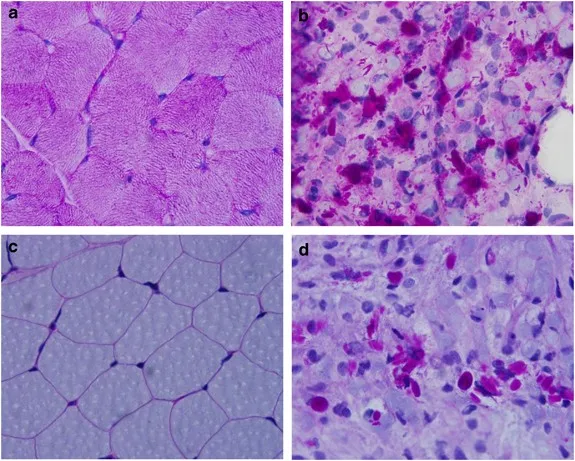
⭐ The abnormal glycogen deposits are PAS-positive and diastase-resistant.
Clinical Presentation - Liver's Rocky Road
- Early Infancy Onset: Typically presents within the first 18 months of life with classic signs of liver dysfunction.
- Failure to Thrive: Poor weight gain and growth retardation are prominent early indicators.
- Progressive Hepatosplenomegaly: The liver and spleen progressively enlarge. The liver feels unusually firm, evolving to a nodular texture characteristic of cirrhosis.
- Variable Muscle & Heart Involvement: Some patients may also exhibit hypotonia, muscle weakness, and cardiomyopathy, complicating the clinical picture.
⭐ The core pathology is aggressive hepatic fibrosis. The abnormal, insoluble glycogen precipitates, provoking an immune response that rapidly destroys the liver, leading to death by age 5 without a transplant.
Diagnosis - Confirming the Culprit
- Enzyme Assay: Definitive test measuring glycogen branching enzyme (GBE) activity in liver, muscle, or skin fibroblasts.
- Liver Biopsy: Histology is key.
- Shows PAS-positive, diastase-resistant inclusions (abnormal glycogen).
- Reveals progressive fibrosis leading to cirrhosis.
- Genetic Testing: Confirms diagnosis by identifying mutations in the GBE1 gene.
- Prenatal Diagnosis: Possible via amniocentesis or chorionic villus sampling (CVS).
⭐ Exam Favorite: The pathognomonic finding on liver biopsy is the presence of cytoplasmic inclusions that are PAS-positive but resistant to diastase digestion, unlike normal glycogen which is digested.
Management - Support & Transplant
- Mainstay: Primarily supportive care, focusing on nutritional management to prevent hypoglycemia and manage progressive liver dysfunction.
- Curative: Liver transplantation is the only definitive treatment for hepatic failure, often required in early childhood.
⭐ Transplant corrects the hepatic disease, but extrahepatic manifestations like cardiomyopathy may persist and progress.
- Deficiency: Branching enzyme (α-1,4 → α-1,6 glucosyltransferase).
- Inheritance: Autosomal recessive.
- Pathology: Accumulation of abnormal, unbranched glycogen (amylopectin-like) in hepatocytes.
- Clinical Hallmark: Presents in infancy with failure to thrive, hepatosplenomegaly, and rapidly progressive liver cirrhosis.
- Mechanism: The abnormal glycogen structure provokes a foreign-body immune reaction, leading to hepatic fibrosis.
- Prognosis: Typically results in death from liver failure by age 5.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

