Initial Clues - Spotting the Suspect
-
Clinical Presentation: Varies by type, but classic signs raise suspicion.
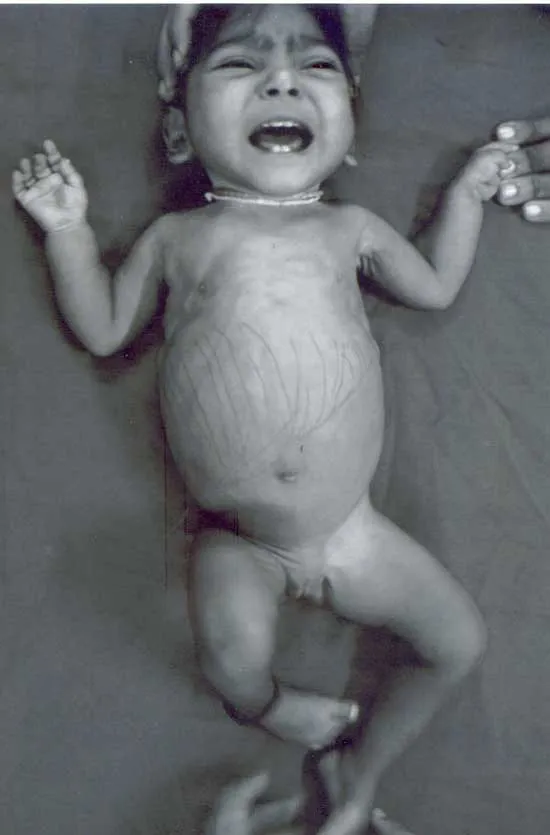
- Hepatic forms: Present in infancy/early childhood.
- Hepatomegaly (protuberant abdomen).
- Fasting hypoglycemia (seizures, lethargy).
- Poor growth, doll-like facies (Von Gierke).
- Myopathic forms: Present in adolescence/adulthood.
- Exercise intolerance, muscle cramps, weakness.
- Second-wind phenomenon (McArdle).
- Progressive weakness (Pompe).
- Hepatic forms: Present in infancy/early childhood.
-
Initial Lab Panel:
- Blood glucose (fasting): ↓
- Lactate, uric acid, triglycerides, cholesterol: ↑ (especially in GSD I)
- Liver transaminases (ALT/AST): ↑
- Creatine kinase (CK): ↑ (in myopathic forms)
⭐ High-Yield Clue: A key initial test is the glucagon stimulation test. In GSD I, there is no rise in blood glucose after glucagon administration, but a marked rise in lactate.
Lab Investigations - The Bloodwork Story
- Fasting State Analysis: The cornerstone of initial workup.
- Hypoglycemia: Severe, hallmark of GSD I (Von Gierke).
- Lactic Acidosis: ↑↑ Lactate, especially in GSD Ia.
- Hyperuricemia: ↑ Uric acid, leading to gout.
- Hyperlipidemia: ↑ Triglycerides and cholesterol.
- Enzyme Markers: Pinpoint organ involvement.
- Liver Transaminases (AST/ALT): ↑ in hepatic types (I, III, IV).
- Creatine Kinase (CK-MM): ↑ in myopathic types (II, V, VII).
- Provocative Testing:
- Glucagon Challenge: Assesses hepatic glycogenolysis.
⭐ In GSD Type I, a glucagon challenge fails to raise blood glucose but significantly increases lactate levels.
📌 Mnemonic (Von Gierke): Think Very Poor Liver. ↑ VLDL (lipids), ↑ Purines (uric acid), ↑ Lactate.
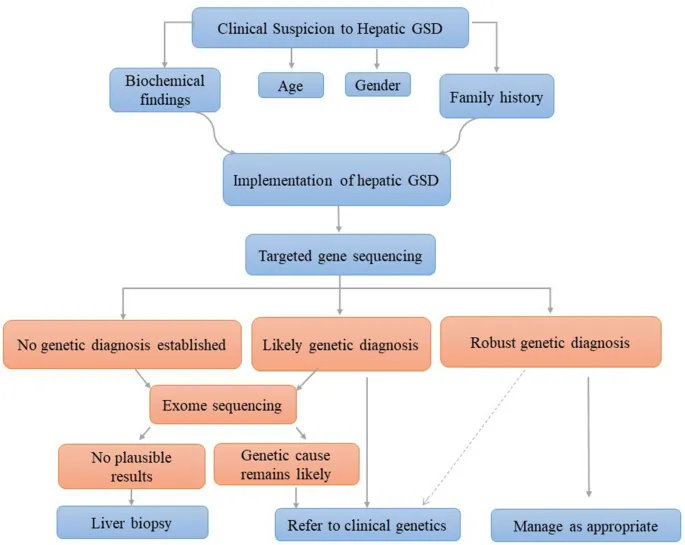
Confirmatory Tests - Naming the Culprit
-
Gold Standard: Enzyme Assay & Genetic Testing
- Definitive diagnosis via measurement of specific enzyme activity.
- Samples: Leukocytes, cultured skin fibroblasts, or tissue biopsy (muscle/liver).
- Molecular genetic testing identifies specific gene mutations (e.g., G6PC, PYGM).
-
Tissue Biopsy
- Liver Biopsy: Demonstrates ↑ glycogen content and potential fibrosis or fatty change.
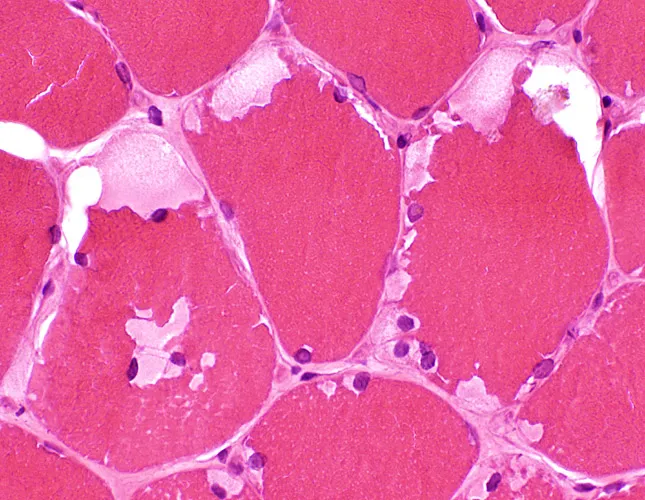
- Muscle Biopsy: Crucial for myopathic forms (e.g., McArdle, Pompe).
- Histology: Periodic acid-Schiff (PAS) stain reveals excess glycogen.
⭐ Pompe disease (Type II) is unique as both a GSD and a lysosomal storage disease. Muscle biopsy distinctively shows glycogen accumulation within lysosomes.
Tissue & Imaging - A Deeper Look
- Tissue Biopsy: The definitive diagnostic standard for many GSDs.
- Liver Biopsy: Primarily for hepatic forms (e.g., Von Gierke, Cori). Assesses glycogen content and specific enzyme activity.
- Muscle Biopsy: For myopathic forms (e.g., Pompe, McArdle). Shows excess glycogen in muscle fibers.
- Histopathology:
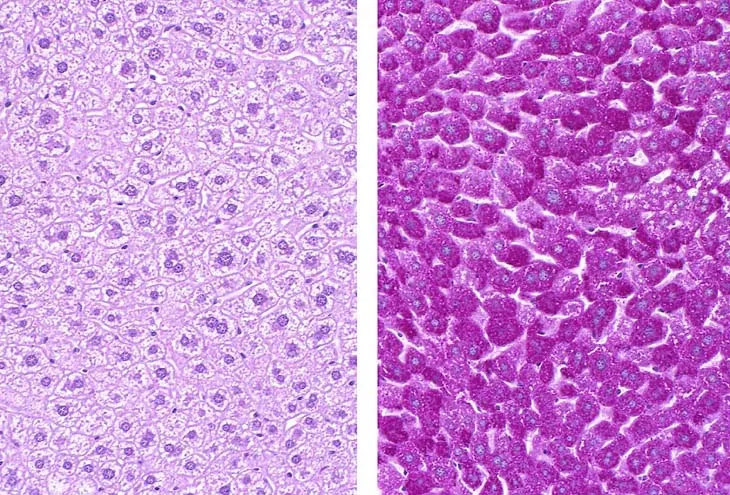
- Periodic acid-Schiff (PAS) stain: Stains glycogen magenta. Tissue is PAS-positive.
- Diastase Digestion: Pre-treatment with diastase enzyme digests glycogen; the PAS stain will then be negative.
- Imaging:
- Ultrasound/CT/MRI: Primarily to assess hepatomegaly and detect liver adenomas, a common complication in GSD I.
⭐ In GSDs, the PAS stain is positive, revealing glycogen accumulation. Crucially, this staining disappears after treatment with diastase (diastase-labile), confirming the substance is indeed glycogen.
High‑Yield Points - ⚡ Biggest Takeaways
- Initial labs for a suspected GSD include blood glucose, lactate, uric acid, and lipids.
- Definitive diagnosis requires enzyme assays on liver or muscle biopsy or, increasingly, genetic testing.
- Von Gierke (Type I) classically shows severe hypoglycemia, lactic acidosis, hyperuricemia, and hyperlipidemia.
- Pompe disease (Type II) is unique for its massive cardiomegaly and profound hypotonia with normal glucose.
- McArdle disease (Type V) presents with exercise intolerance, myoglobinuria, and a characteristic flat venous lactate curve with exercise.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

