Methionine Metabolism - The Sulfur Start
- Essential amino acid Methionine is converted to S-adenosylmethionine (SAM), the universal methyl donor, in an ATP-dependent reaction.
- SAM donates its methyl group, becoming S-adenosylhomocysteine (SAH), then Homocysteine.
- Homocysteine (Hcy) is a critical branch point.
- Remethylation: Hcy → Methionine. Requires vitamins B12 and Folate.
- Transsulfuration: Hcy → Cysteine. Requires vitamin B6 (PLP).
⭐ Elevated homocysteine is an independent risk factor for thrombotic events (atherosclerosis, DVT) and ectopia lentis.
📌 Mnemonic: To get UP to Methionine, you need B12/Folate. To go OUT to Cysteine, you need B6.
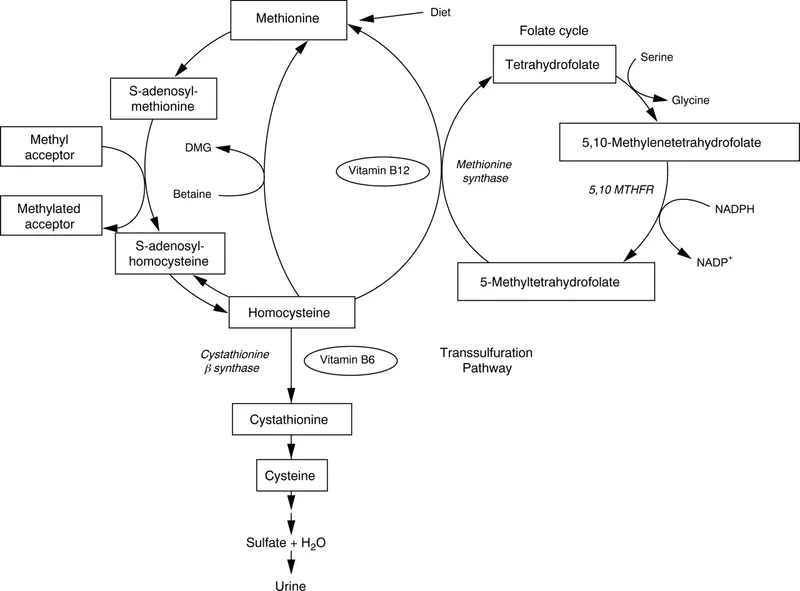
Homocysteine's Crossroads - Recycle or Remove
Homocysteine (Hcy) is metabolized via two main pathways: remethylation (recycling) or transsulfuration (removal). The pathway choice depends on methionine levels.
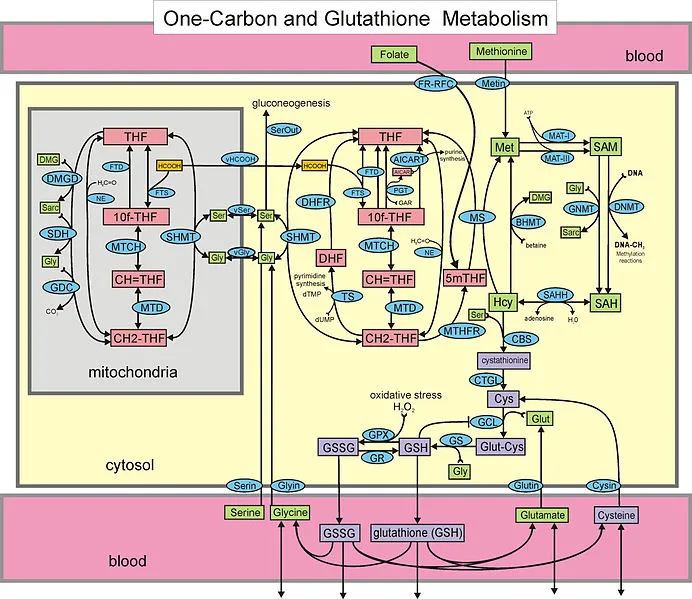
-
Remethylation (Recycle): Active when methionine is low.
- Hcy is converted back to methionine by methionine synthase.
- Requires Vitamin B₁₂ and Folate (B₉).
-
Transsulfuration (Remove): Active when methionine/cysteine are high.
- Hcy is irreversibly converted to cysteine.
- Key enzyme: Cystathionine β-synthase (CBS).
- Requires Vitamin B₆ (pyridoxine).
⭐ Classic homocystinuria is most commonly caused by a deficiency in Cystathionine β-synthase (CBS), leading to elevated homocysteine and methionine. Patients present with thromboembolic events, lens dislocation, and skeletal abnormalities.
Homocystinuria - A Sticky Situation
Autosomal recessive deficiency of cystathionine β-synthase (CBS), leading to ↑ homocysteine & methionine. Requires co-factor pyridoxal phosphate (B6).
- Clinical Features:
- Ocular: Ectopia lentis (lens dislocation) → downward & inward.
- Skeletal: Marfanoid habitus, osteoporosis, kyphosis.
- Vascular: Thromboembolism (atherosclerosis, DVT, stroke) is a major cause of morbidity/mortality.
- Neurologic: Intellectual disability, seizures.
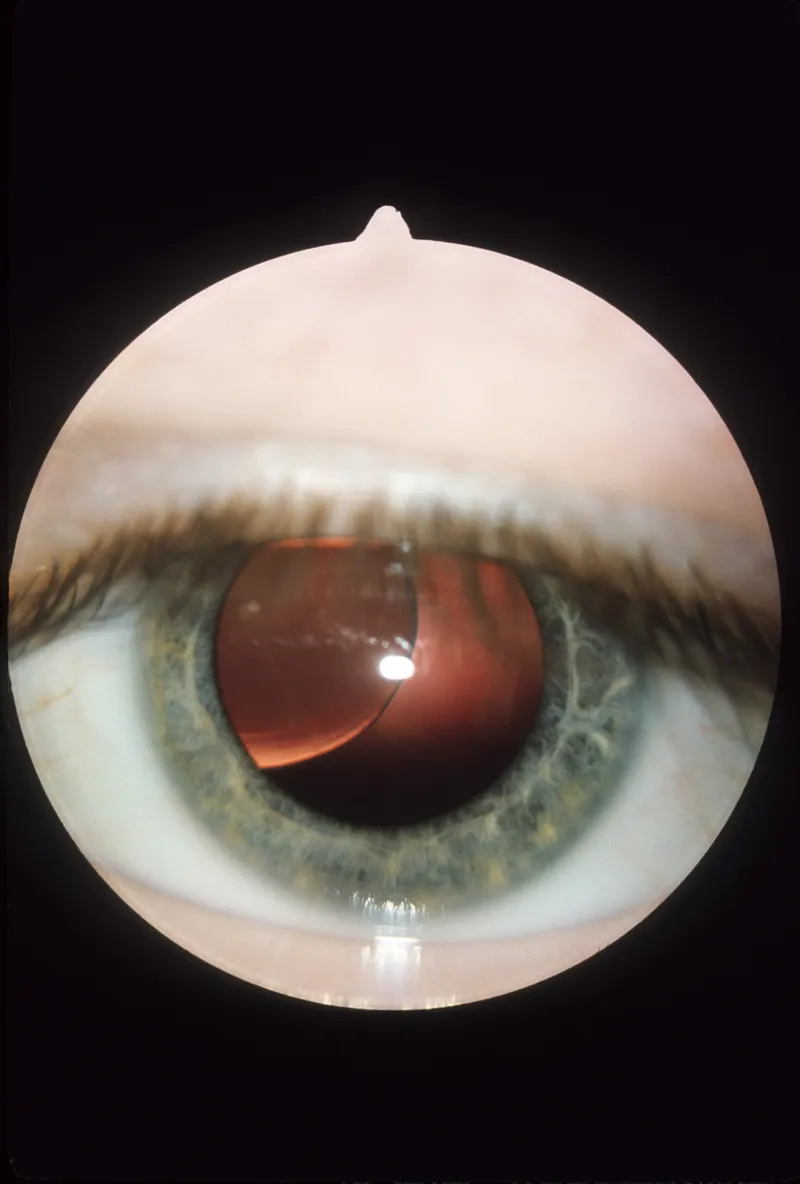
⭐ Homocysteine is prothrombotic, causing endothelial damage and increasing the risk of premature atherosclerosis, venous thrombosis, and stroke.
- Diagnosis & Treatment:
- Screening: ↑ Homocysteine in urine/plasma.
- Treatment: High doses of Vitamin B6 (pyridoxine) for responsive forms. Supplement with folate and Vitamin B12. Betaine promotes remethylation of homocysteine to methionine.
Cystinuria - The COLA Problem
- Pathophysiology: Autosomal recessive defect in the dibasic amino acid transporter (SLC3A1/SLC7A9 genes) in the proximal convoluted tubule & intestine.
- Impairs reabsorption of Cystine, Ornithine, Lysine, Arginine (📌 COLA).
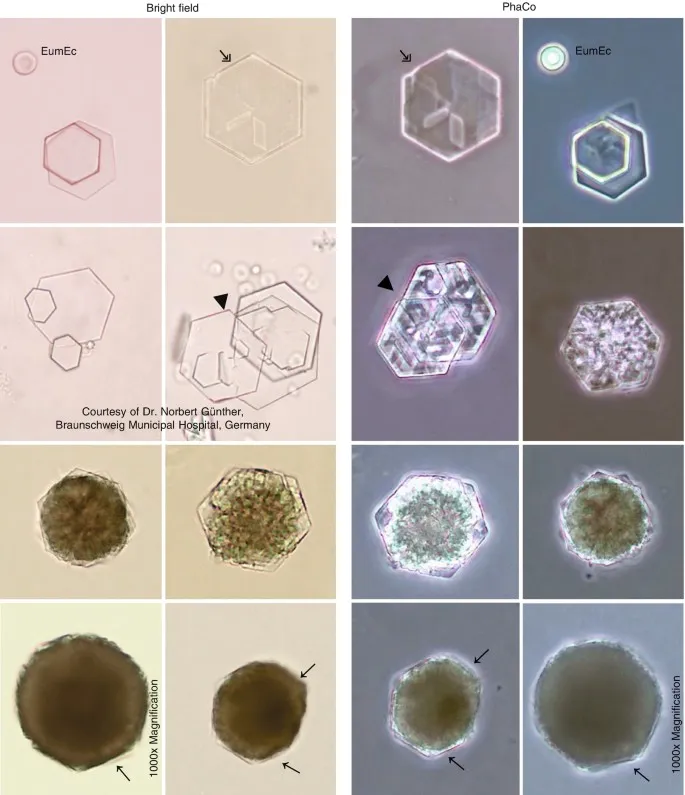
- Clinical Manifestations: Recurrent hexagonal cystine kidney stones, often presenting in young adults. Cystine is poorly soluble in acidic urine.
- Diagnosis:
- Urinalysis: Pathognomonic hexagonal crystals.
- Positive sodium cyanide-nitroprusside test.
- Management:
- ↑ Fluid intake (> 3L/day).
- Urine alkalinization (e.g., potassium citrate).
- Chelating agents (penicillamine, tiopronin) for severe cases.
⭐ Unlike radiolucent uric acid stones, cystine stones are radiopaque due to their sulfur content.
High‑Yield Points - ⚡ Biggest Takeaways
- Methionine generates S-adenosylmethionine (SAM), the universal methyl donor, and homocysteine.
- Homocystinuria (most often cystathionine β-synthase deficiency) causes marfanoid habitus, thromboembolism, and downward lens dislocation.
- Key cofactors: Vitamin B6 (pyridoxine) for the transsulfuration pathway and Vitamin B12/Folate for remethylation.
- Cystinuria, a transporter defect, leads to recurrent hexagonal cystine kidney stones.
- High homocysteine is a major risk factor for atherosclerosis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

