Circle of Willis - The Brain's Roundabout
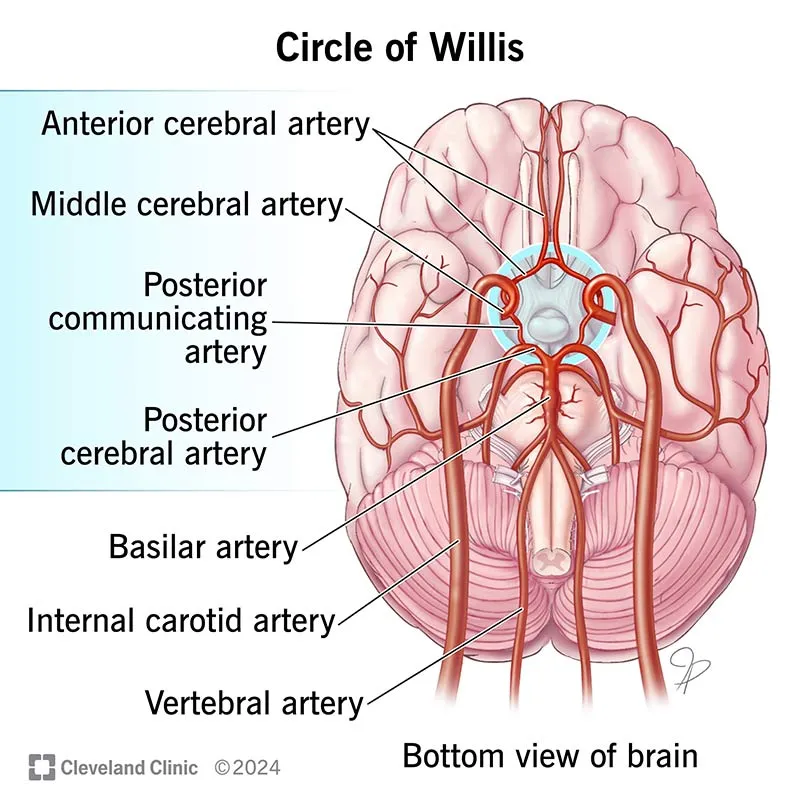
An arterial anastomosis at the base of the brain, providing collateral circulation. Formed by:
- Anterior Circulation (from Internal Carotids):
- Anterior Cerebral Artery (ACA)
- Middle Cerebral Artery (MCA)
- Posterior Circulation (from Vertebral Arteries → Basilar Artery):
- Posterior Cerebral Artery (PCA)
- Communicating Arteries:
- Anterior Communicating (AComm): Connects the two ACAs.
- Posterior Communicating (PComm): Connects PCA to the ICA/MCA.
⭐ Aneurysm Hotspot: The most common site for saccular (berry) aneurysms is the junction of the Anterior Communicating Artery (AComm) with the Anterior Cerebral Artery (ACA).
Anterior Circulation - Front-End Failures
-
Anterior Cerebral Artery (ACA)
- Presentation: Contralateral paralysis & sensory loss, lower limb > upper limb.
- Key Signs: Frontal lobe signs (disinhibition, personality changes), urinary incontinence.
- 📌 Mnemonic: A in ACA for Abdominal muscles down to feet (midline).
-
Middle Cerebral Artery (MCA)
- Presentation: Contralateral paralysis & sensory loss, upper limb & face > lower limb.
- Key Signs (Hemisphere Dependent):
- Dominant: Aphasia (Broca's, Wernicke's, or global).
- Non-Dominant: Hemineglect, anosognosia.
- Homonymous hemianopia (contralateral) is common.
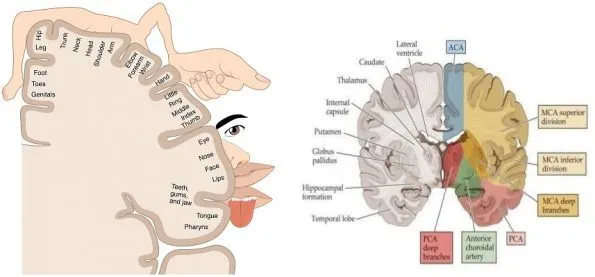
⭐ Exam Favourite: MCA strokes are the most common type of ischemic stroke. A resulting global aphasia (impaired fluency, comprehension, and repetition) indicates a large lesion affecting both Broca's and Wernicke's areas.
Posterior Circulation - Back-End Blackouts
- Posterior Cerebral Artery (PCA):
- Supplies the occipital lobe.
- Occlusion causes contralateral homonymous hemianopia with macular sparing.
- Can also cause alexia (inability to read) without agraphia (inability to write).
- Basilar Artery:
- Complete occlusion leads to catastrophic "Locked-in Syndrome."
- Affects the pons, causing quadriplegia and mutism with preserved consciousness and vertical eye movements.
- Cerebellar Arteries (PICA & AICA):
- General signs: Vertigo, nystagmus, ipsilateral ataxia.
- PICA → Lateral Medullary (Wallenberg) Syndrome:
- Ipsilateral: Facial pain/temp loss, Horner's syndrome.
- Contralateral: Body pain/temp loss.
- Hoarseness & dysphagia.

⭐ Wallenberg syndrome (PICA occlusion) spares the corticospinal tracts, so patients present with dramatic sensory and cerebellar signs but notably have minimal motor weakness.
Lacunar Strokes - Tiny Territory Trouble
- Pathophysiology: Occlusion of single, deep-penetrating arteries (e.g., lenticulostriate, thalamoperforating).
- Etiology: Strongly associated with chronic hypertension and diabetes, leading to lipohyalinosis and microatheroma.
- Classic Syndromes:
- Pure Motor: Contralateral paralysis (face, arm, leg).
- Pure Sensory: Contralateral numbness/paresthesia.
- Ataxic Hemiparesis: Ipsilateral ataxia with contralateral motor weakness.
- Dysarthria-Clumsy Hand: Slurred speech and clumsiness in one hand.
⭐ Key feature: Absence of cortical signs (e.g., aphasia, neglect, visual field loss).

High‑Yield Points - ⚡ Biggest Takeaways
- ACA stroke classically presents with contralateral lower extremity deficits, greater than upper.
- MCA stroke is most common, affecting the contralateral face and arm; look for aphasia (dominant) or hemineglect (non-dominant).
- PCA stroke causes contralateral hemianopia with macular sparing.
- Basilar artery occlusion can lead to catastrophic “locked-in” syndrome.
- PICA strokes cause Wallenberg syndrome (lateral medullary), with vertigo, dysphagia, and ipsilateral ataxia.
- Lacunar strokes cause pure motor or sensory deficits.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

