Esophageal Atresia - Tube Troubles

- Developmental failure of the tracheoesophageal septum to fuse, leading to an incomplete esophagus.
- Most common variant (~85%) is proximal esophageal atresia with a distal tracheoesophageal fistula (TEF).
- Presents with polyhydramnios in utero. Neonates show excessive drooling, choking, and cyanosis during feeding.
- Diagnosis confirmed by inability to pass a nasogastric tube into the stomach.
⭐ 📌 Associated with VACTERL syndrome: Vertebral defects, Anal atresia, Cardiac defects, Tracheo-Esophageal fistula, Renal anomalies, and Limb abnormalities.
Gastric & Duodenal Defects - Exit Blocks
-
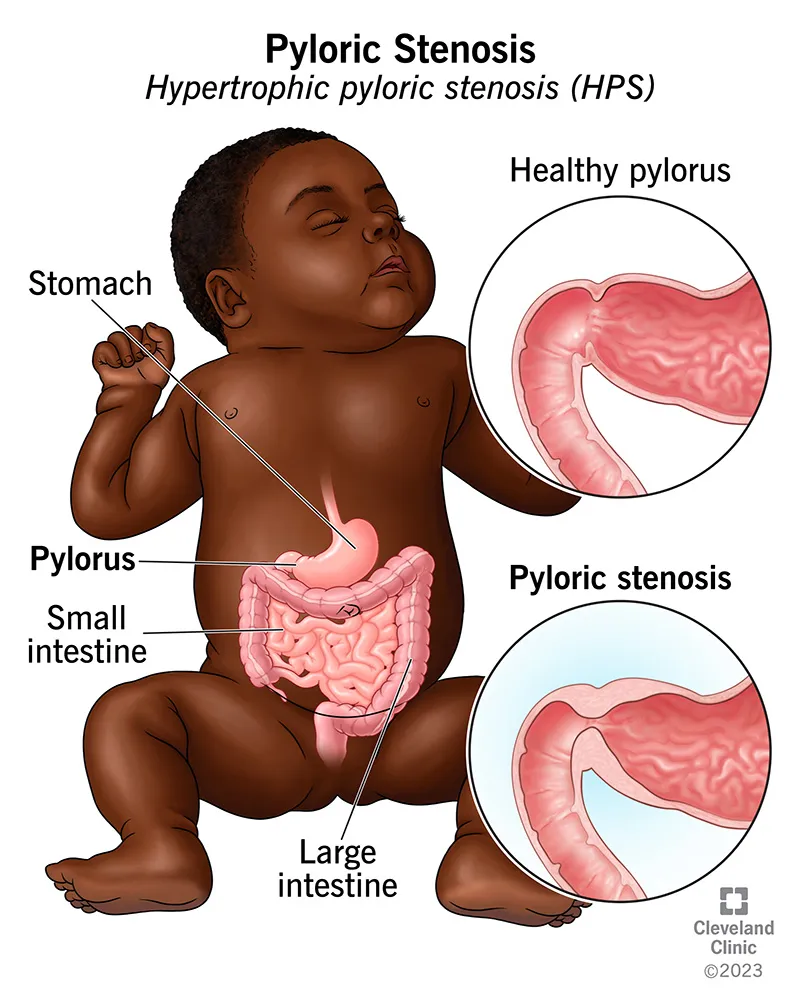
Pyloric Stenosis: Most common gastric outlet obstruction in infants. Presents at 2-8 weeks.
- Clinical: Projectile non-bilious vomiting, palpable epigastric "olive" mass, visible peristalsis.
- Labs: Hypokalemic, hypochloremic metabolic alkalosis due to vomiting HCl.
- Dx: Abdominal ultrasound.
-
Duodenal Atresia: Congenital failure of duodenum to recanalize.
- Clinical: Bilious vomiting within hours of birth.
- X-ray: "Double bubble" sign (air in stomach and proximal duodenum).
-
Annular Pancreas: Ventral pancreatic bud abnormally encircles the 2nd part of the duodenum, causing obstruction.
⭐ "Double bubble, double trouble": The "double bubble" sign of duodenal atresia is frequently associated with Down syndrome.
Midgut Malrotation - Twisted Guts
- Pathophysiology: Failure of the midgut to complete its normal 270° counter-clockwise rotation during fetal development.
- Anatomy: Cecum remains in the RUQ, fixed by fibrous Ladd's bands, which can compress the duodenum.
- Presentation: Bilious vomiting in a neonate is the hallmark sign.
- Complication: Midgut volvulus - intestine twists around the superior mesenteric artery (SMA), leading to ischemia and necrosis.
- Diagnosis: Upper GI series shows abnormal position of the ligament of Treitz.
⭐ Bilious emesis in the first few days of life is a surgical emergency until proven otherwise, often indicating malrotation.

Abdominal Wall Defects - Innies vs. Outies
-
Omphalocele ("Innie")
- Midline herniation of abdominal contents (liver, bowel) into the base of the umbilical cord.
- Sealed by a membranous sac (peritoneum + amnion).
- Caused by failed fusion of lateral embryonic folds.
-
Gastroschisis ("Outie")
- Paraumbilical (typically right) full-thickness wall defect.
- Uncovered bowel herniation; exposed to amniotic fluid, causing inflammation.
- Due to vascular insult (omphalomesenteric artery occlusion).
⭐ Omphalocele has a high rate of associated anomalies: Trisomies 13, 18, 21, cardiac defects, and Beckwith-Wiedemann syndrome.
Hindgut & Remnants - Final Hurdles
- Hirschsprung Disease
- Cause: Failed migration of neural crest cells to the distal colon → aganglionic segment (Auerbach & Meissner plexuses absent).
- Presentation: Failure to pass meconium within 48 hours, bilious vomiting, abdominal distension.
- Diagnosis: Rectal suction biopsy is the gold standard, revealing no ganglion cells.
- Imperforate Anus
- Cause: Incomplete separation of the cloaca or failed breakdown of the anal membrane.
- Presentation: No anal opening; meconium may pass via a fistula to the urethra, perineum, or vagina.
- Associated with VACTERL syndrome.
⭐ Hirschsprung disease is strongly associated with Down syndrome (Trisomy 21).

High‑Yield Points - ⚡ Biggest Takeaways
- Tracheoesophageal fistula classically presents with polyhydramnios, followed by choking and cyanosis with the first feed.
- Duodenal atresia is defined by the "double-bubble" sign on X-ray and its strong association with Down syndrome.
- Pyloric stenosis causes non-bilious projectile vomiting and a palpable "olive-like" mass at 2-6 weeks of age.
- Meckel's diverticulum (Rule of 2s) is the most common anomaly, often causing painless rectal bleeding.
- Hirschsprung disease is an aganglionic megacolon causing failure to pass meconium in a newborn.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

