Visceral Afferents - The Body's Inner Spies
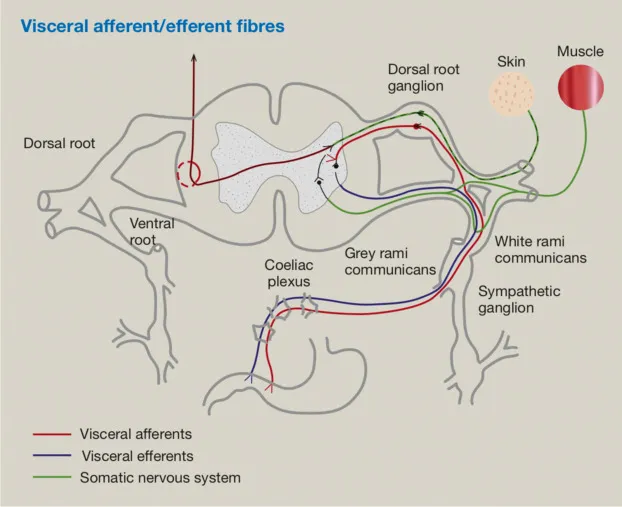
- Sensory fibers monitoring internal organs; cell bodies in dorsal root ganglia (DRG) or cranial nerve ganglia.
- Travel retrograde along autonomic pathways to the CNS.
- Pain Pathway:
- Above pelvic pain line: Follows sympathetic fibers.
- Below pelvic pain line: Follows parasympathetic (pelvic splanchnic) fibers.
- Non-Pain/Reflex Pathway: Primarily follows parasympathetic fibers (e.g., Vagus nerve for baroreflex).
- Mechanism for referred pain due to convergence with somatic afferents.
⭐ Visceral pain from pelvic organs (e.g., cervix, bladder base, prostate) below the pelvic pain line is referred to the S2-S4 dermatomes because it travels via pelvic splanchnic nerves.
Pain Pathways - The Pelvic Pain Line
-
The Pelvic Pain Line (PPL) is a conceptual line at the inferior peritoneal reflection that determines the pathway for visceral pain from pelvic organs.
-
Above PPL (Intraperitoneal):
- Structures: Uterine fundus/body, ovaries, fallopian tubes, sigmoid colon.
- Pathway: Afferent fibers follow sympathetic innervation retrogradely.
- Spinal Level: T12-L2.
-
Below PPL (Subperitoneal):
- Structures: Cervix, upper vagina, prostate, bladder.
- Pathway: Afferent fibers follow parasympathetic innervation (pelvic splanchnic nerves).
- Spinal Level: S2-S4.
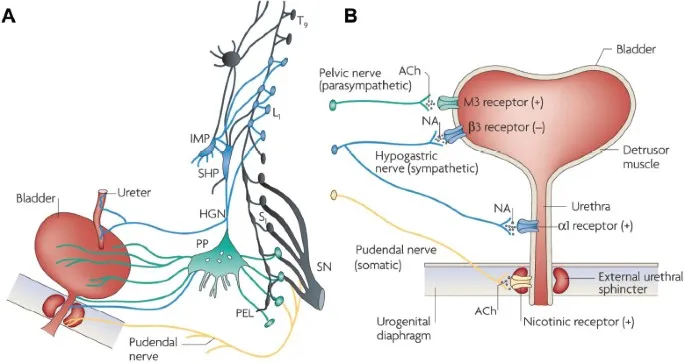
⭐ During labor, pain from uterine contractions (fundus/body) travels via sympathetic fibers to T10-L1, while pain from cervical dilation travels via parasympathetic fibers to S2-S4. This dual pathway is why epidural anesthesia is targeted to cover a wide range of spinal levels.
Referred Pain - Cross-Wired Signals
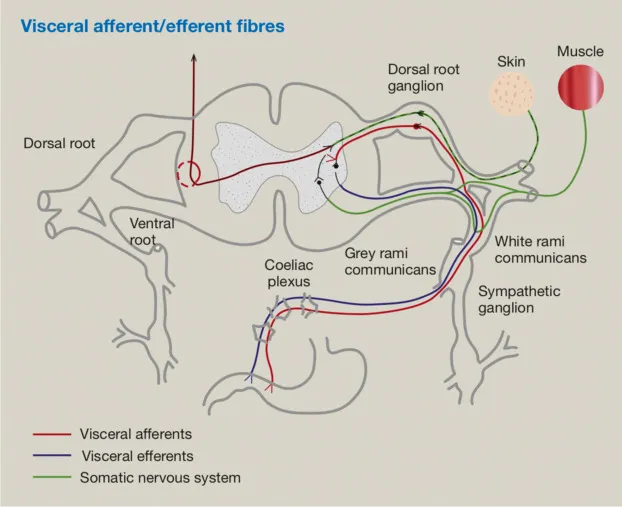
- Core Concept: Pain originating from an internal organ (visceral) is perceived as coming from a specific surface area of the body (somatic).
- Neural Basis: Visceral afferent (sensory) neurons and somatic afferent neurons from a dermatome converge and synapse on the same second-order neuron in the spinal cord's dorsal horn.
- Brain Interpretation: The brain, more accustomed to somatic signals, misinterprets the origin of the visceral pain, localizing it to the corresponding somatic dermatome.
⭐ Diaphragmatic Irritation: The phrenic nerve (C3, C4, C5) innervates the diaphragm. Irritation (e.g., by a subphrenic abscess or gallbladder inflammation) causes referred pain to the supraclavicular region (shoulder), which is supplied by the C3 and C4 dermatomes.
Reflex Pathways - Unconscious Sensing
- Visceral afferents mediate reflexes below conscious perception, vital for homeostasis.
- Receptors: Baroreceptors, chemoreceptors, and mechanoreceptors continuously monitor the internal environment.
- Primary Pathway:
- Afferent signals travel retrograde along parasympathetic (esp. Vagus n.) and sympathetic nerves.
- Central destination: Nucleus of the Solitary Tract (NTS) in the medulla.
- NTS integrates sensory data to modulate autonomic output via reflex arcs.
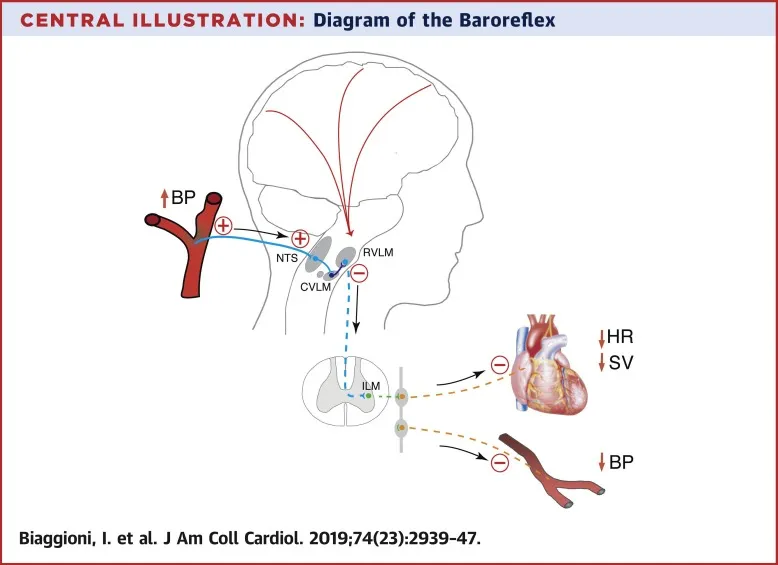
⭐ The Nucleus of the Solitary Tract (NTS) is the key visceral sensory integration center. Lesions can lead to severe autonomic dysfunction, including orthostatic hypotension or hypertensive crises.
High‑Yield Points - ⚡ Biggest Takeaways
- Visceral afferent fibers travel alongside autonomic nerves (sympathetic and parasympathetic) back to the CNS.
- Cell bodies of visceral afferents reside in the dorsal root ganglia or cranial nerve ganglia.
- Visceral pain afferents generally follow sympathetic pathways retrograde.
- Afferents for normal physiological reflexes (e.g., baroreflex) typically travel with parasympathetic fibers.
- Referred pain is the convergence of visceral and somatic afferents at the same spinal cord segment.
- Pain from pelvic organs below the pelvic pain line travels via parasympathetic fibers (S2-S4).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

