Initial Assessment - First Glance
- Anatomy & Age: Location (e.g., distal limb, pressure area) and duration (acute vs. chronic).
- Bleeding & Borders: Active hemorrhage? Well-defined or irregular edges?
- Color & Circulation: Assess wound bed (red, yellow, black) and periwound tissue perfusion.
- Dimensions: Measure Length x Width x Depth in cm.
- Exudate & Edema: Note fluid type (serous, purulent) and amount; check for surrounding swelling.
⭐ A wound failing to heal by 3 months is typically classified as chronic. This timeframe is critical for escalating care and investigating underlying etiologies like ischemia or infection.
Wound Bed - Reading the Tissues
-
Assess tissue types (Viability):
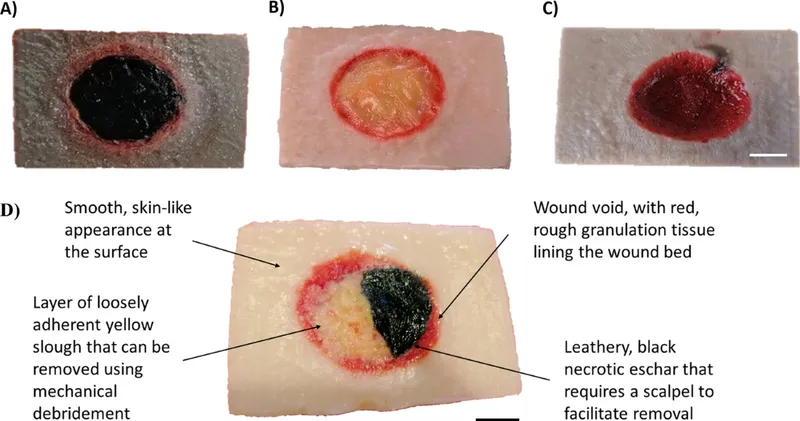
- Granulation: Beefy red, bumpy, moist. Indicates healthy healing.
- Epithelial: Pink/translucent, new skin growing from edges.
- Slough: Yellow, tan, or white. Stringy or fibrinous. Non-viable tissue requiring removal.
- Eschar: Black or brown, dry, leathery, necrotic tissue. Non-viable.
-
Identify Tissue Percentage: Estimate the percentage of each tissue type in the wound bed (e.g., 70% granulation, 30% slough).
-
Exudate Assessment: Note color, consistency, and amount.
- Serous (clear), Sanguineous (bloody), Serosanguineous (pinkish), Purulent (pus).
⭐ In a non-infected, stable heel ulcer with dry eschar and poor arterial flow, do not debride. The eschar acts as a physiologic cover.
Infection & Edges - Spotting Trouble
-
Clinical Signs of Infection:
- 📌 IFEE: Induration, Fever, Erythema, Edema.
- Also: ↑ pain, purulent or malodorous discharge, localized warmth.
- Systemic signs: Leukocytosis, fever > 38.5°C.
- Quantitative swab culture: > 10^5 CFU/g of tissue is diagnostic.
-
Wound Edge Assessment:
- Healthy: Pink, attached, migrating across the wound base (epithelializing).
- Unhealthy:
- Macerated: White, boggy from excess moisture.
- Epibole: Rolled, thickened edges that have stopped migrating.
- Fibrotic/Calloused: Hard, raised, non-progressive.
- Undermining/Tunneling: Indicates deeper tissue damage.
⭐ Acute wound infections (<30 days) are most commonly caused by S. aureus. Chronic or delayed infections suggest biofilm or atypical organisms.
High‑Yield Points - ⚡ Biggest Takeaways
- The gold standard for wound culture is a tissue biopsy, not a surface swab, to distinguish infection from colonization.
- Assess lower extremity ulcers with an Ankle-Brachial Index (ABI); an ABI < 0.9 is highly suggestive of peripheral artery disease (PAD).
- A positive probe-to-bone test is highly specific for osteomyelitis in diabetic foot ulcers.
- Wood's lamp examination helps identify certain pathogens, like Pseudomonas (green fluorescence).
- Healthy wounds show red granulation tissue; yellow slough and black eschar require debridement.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

