🌊 Pathophysiology - Backward Flow Blues
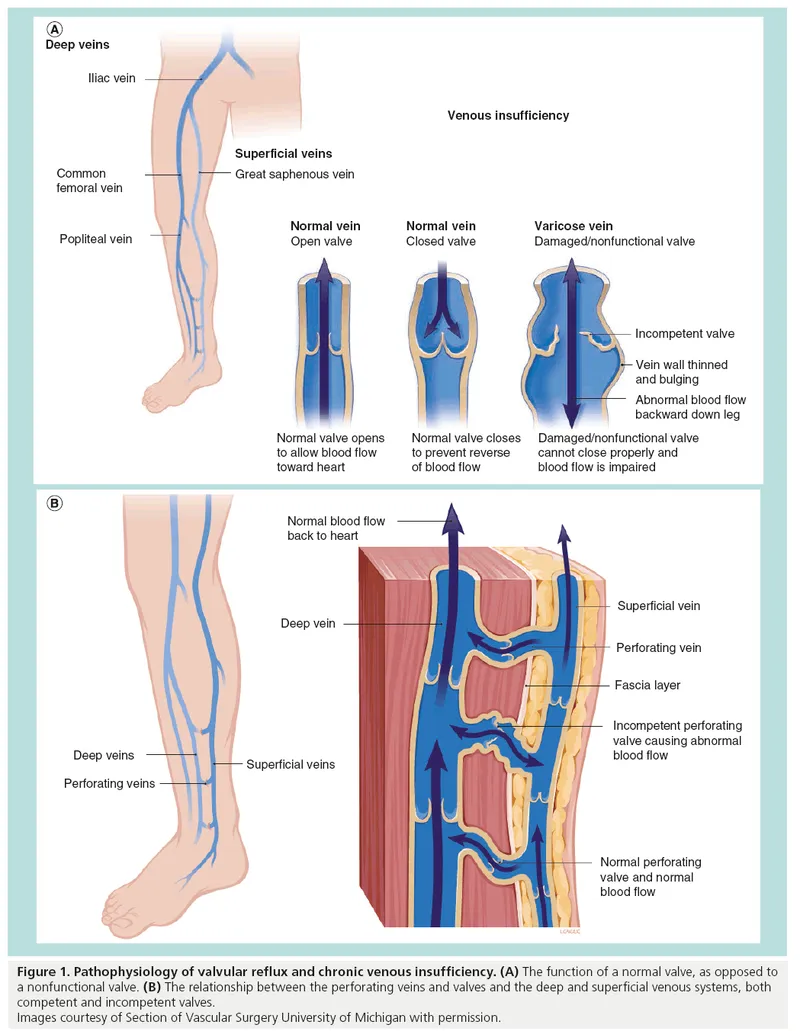
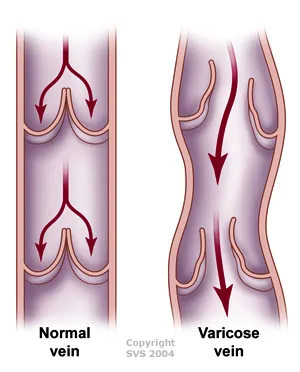
- Core Defect: Venous valve incompetence allows retrograde blood flow (reflux), leading to sustained ambulatory venous hypertension.
- Primary vs. Secondary:
- Primary: Idiopathic/degenerative valve failure (most common).
- Secondary: Post-thrombotic syndrome (DVT damages valves).
- Calf Muscle Pump: Failure (e.g., immobility) is a key contributor, impairing venous return and worsening stasis.
⭐ The most common site of reflux is the saphenofemoral junction (SFJ), where the Great Saphenous Vein (GSV) joins the common femoral vein.
🦵 Legs in Distress
- Symptoms: Dull ache, heaviness, throbbing, cramping, itching.
- Worsens with prolonged standing/sitting; relieved by leg elevation.
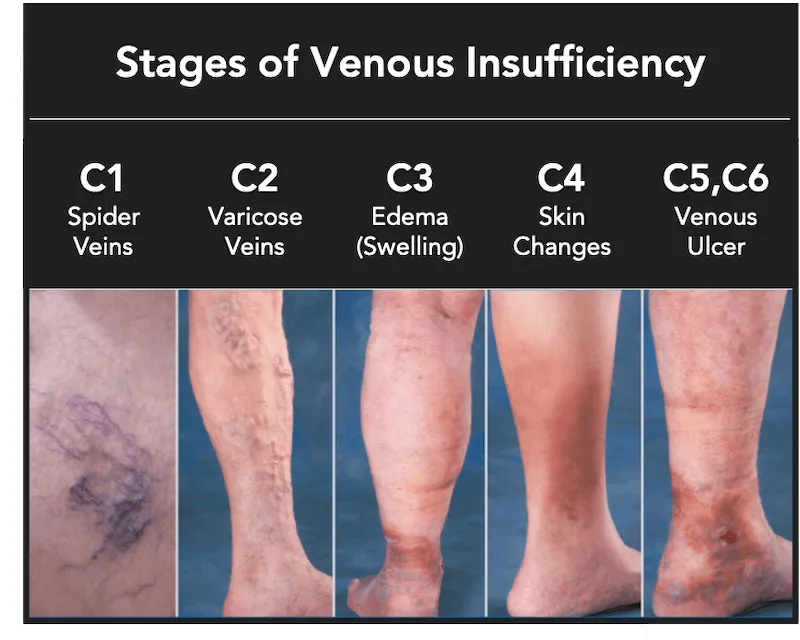
- Signs (Progressive):
- Telangiectasias (<1 mm) & reticular veins (1-3 mm).
- Varicose veins: Dilated, tortuous superficial veins >3 mm.
- Pitting edema, stasis dermatitis (eczema).
- Hyperpigmentation (hemosiderin staining).
- Lipodermatosclerosis: Fibrosis of skin/subcutaneous tissue ("inverted champagne bottle" leg).
- Venous ulcers: Shallow, irregular borders, typically over the medial malleolus.
⭐ Symptoms often do not correlate with the size or number of visible varicose veins.
🩺 Diagnosis - Spotting the Backup
- Primary Tool: Venous Duplex Ultrasound is the gold standard.
- Confirms diagnosis by showing venous reflux > 0.5 seconds.
- Maps anatomy of incompetent superficial, deep, and perforator veins.
- Clinical Staging: CEAP classification grades severity (C0-C6).
- Pre-Treatment Check:
- Ankle-Brachial Index (ABI) is crucial before compression therapy.
⭐ An ABI < 0.9 indicates coexisting Peripheral Artery Disease (PAD). High-compression stockings are contraindicated as they can worsen arterial ischemia.
🩹 Management: Compression & Closure
-
Conservative ("Squeezing")
- First-line: Leg elevation, exercise (calf muscle pump), weight management.
- Compression Therapy: Graded stockings are mainstay.
- 20-30 mmHg: For symptomatic varicose veins & mild edema.
- 30-40 mmHg: For severe CVI, healed ulcers, lymphedema.
- ⚠️ Check Ankle-Brachial Index (ABI) first; contraindicated in severe PAD (ABI < 0.5).
-
Procedural ("Sealing")
- Endovenous Thermal Ablation (EVTA): Laser or radiofrequency.
- First-line for symptomatic great saphenous vein (GSV) incompetence.
- Mechanism: Thermal energy → endothelial damage → vein fibrosis & occlusion.
- Sclerotherapy:
- Injection of a sclerosant (e.g., polidocanol).
- Best for smaller reticular veins or telangiectasias.
- Ligation & Stripping:
- More invasive, largely replaced by ablation.
- Endovenous Thermal Ablation (EVTA): Laser or radiofrequency.
⭐ Post-procedure, duplex US is crucial to confirm successful vein occlusion and to screen for procedure-related deep vein thrombosis (DVT).
💥 Complications - When Veins Rebel
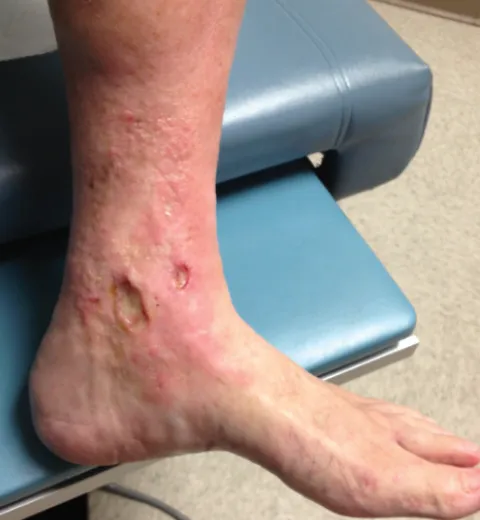
- Stasis Dermatitis: Eczematous rash, pruritus, and hemosiderin deposition (brawny discoloration) from chronic venous hypertension and RBC extravasation.
- Lipodermatosclerosis: Subcutaneous fibrosis and inflammation, leading to a hardened, "inverted champagne bottle" leg.
- Venous Ulcers: Shallow, irregular, exudative ulcers.
⭐ Classically located over the medial malleolus. Contrast with painful arterial ulcers on toes or pressure points.
- Superficial Thrombophlebitis: Painful, palpable, indurated cord.
- Bleeding/Infection: Varicosities can rupture with minor trauma; cellulitis can complicate ulcers.
⚡ Biggest Takeaways
- Chronic venous insufficiency (CVI) stems from incompetent venous valves, causing reflux and venous hypertension.
- Presents with pitting edema, stasis dermatitis (hemosiderin deposition), and lipodermatosclerosis.
- Venous stasis ulcers, especially over the medial malleolus, are a key complication.
- Duplex ultrasound is the diagnostic test of choice to confirm reflux.
- Initial treatment is conservative: leg elevation and compression therapy.
- Refractory cases are treated with endovenous ablation or sclerotherapy.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

