🚨 Signs of Trouble
-
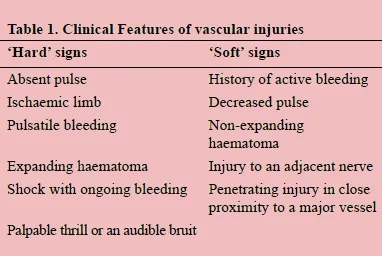
Hard Signs (→ Immediate OR)
- Pulsatile external bleeding
- Rapidly expanding hematoma
- Palpable thrill or audible bruit
- Absent distal pulses
- Signs of distal ischemia (limb threat)
- 📌 6 P's: Pain, Pallor, Pulselessness, Paresthesia, Paralysis, Poikilothermia
-
Soft Signs (→ Further Investigation)
- History of significant hemorrhage at scene
- Diminished distal pulses (vs. absent)
- Non-expanding hematoma
- Bony injury (e.g., fracture/dislocation)
- Neurologic deficit in an adjacent nerve
⭐ Hard signs mandate immediate surgical exploration. Soft signs or an Ankle-Brachial Index (ABI) < 0.9 prompt further diagnostic imaging, typically a CT Angiogram (CTA).
🩺 Diagnosis - Finding the Leak
-
Initial Assessment: Ankle-Brachial Index (ABI) is a rapid, non-invasive screening tool.
- Formula: $ABI = \frac{P_{ankle}}{P_{brachial}}$
- An ABI < 0.9 is highly suggestive of arterial injury.
-
Diagnostic Pathway:
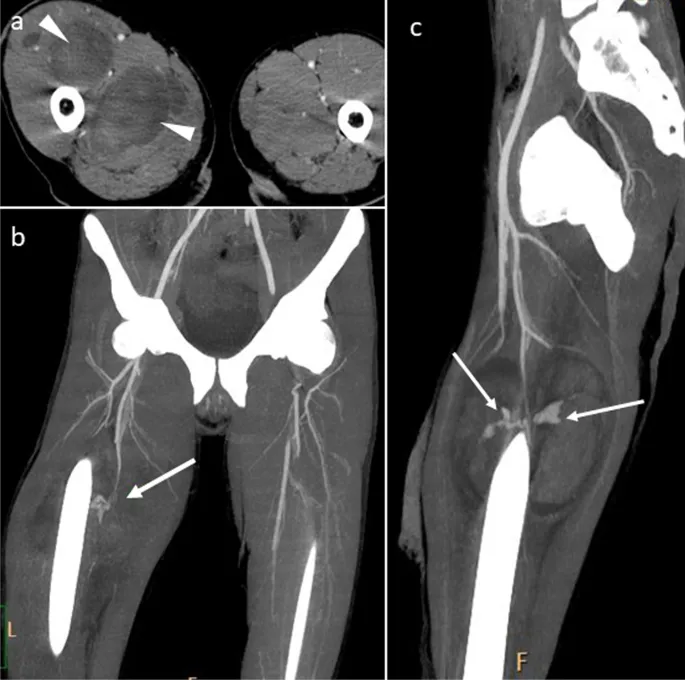
- Definitive Imaging:
- CT Angiography (CTA): The gold standard for hemodynamically stable patients. It's fast, widely available, and accurately identifies the injury (e.g., transection, pseudoaneurysm).
- Conventional Angiography: Most accurate; reserved for equivocal CTA or planned endovascular intervention.
⭐ An ABI < 0.9 in a patient with extremity trauma is a critical threshold. It mandates further imaging (usually CTA) even if distal pulses are palpable.
🩹 Management - Plugging the Holes
-
Initial Control:
- Direct Pressure: First-line for external bleeding.
- Tourniquet: For extremity exsanguination. Apply proximal; note time.
- Damage Control: In unstable patients, use temporary shunts or ligation.
-
Decision Pathway:
- Definitive Repair:
- Primary Repair: Simple lacerations.
- Patch Angioplasty: Vein patch for larger defects.
- Interposition Graft: For segmental loss.
- Ligation: Non-critical arteries or life-saving.
- Endovascular: Stent-grafts, embolization.
⭐ Reversed saphenous vein is the ideal conduit for most extremity arterial repairs due to its resistance to infection and good size match.
💡 Consider prophylactic fasciotomy for significant ischemia-reperfusion to prevent compartment syndrome.
💥 Complications - The Aftermath
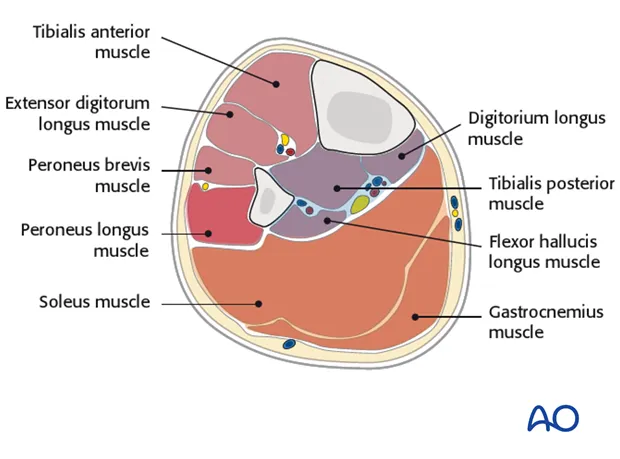
- Compartment Syndrome
- 📌 6 P's: Pain out of proportion, Pallor, Paresthesias, Pulselessness (late), Paralysis (late), Poikilothermia.
- Dx: Compartment pressure > 30 mmHg or Delta P (Diastolic BP - Compartment P) < 20-30 mmHg.
- Tx: Emergent fasciotomy.
- Reperfusion Injury
- Mechanism: ↑ Oxygen free radicals & inflammatory cascade post-revascularization.
- Leads to: Rhabdomyolysis (↑ CK), hyperkalemia, metabolic acidosis, AKI.
- Other
- Thrombosis/Embolism
- Infection (especially with grafts)
- Late: Pseudoaneurysm, Arteriovenous Fistula (AVF)
⭐ Pain out of proportion to injury is the earliest and most sensitive sign of compartment syndrome. Pulselessness is a very late and ominous finding.
⚡ Biggest Takeaways
- Hard signs (pulsatile bleed, expanding hematoma, bruit/thrill, absent pulses) mandate immediate surgical exploration.
- Soft signs (proximity injury, diminished pulses) or an ABI < 0.9 require further imaging, typically CTA.
- Always suspect popliteal artery injury with any posterior knee dislocation or complex knee injury; get an ABI/CTA.
- Compartment syndrome is a clinical diagnosis (pain out of proportion); requires emergent fasciotomy.
- Initial hemorrhage control is direct pressure; use a tourniquet for uncontrolled extremity bleeding.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

