🩸 Pathophysiology - Blood Flow Blockade
- Sudden cessation of arterial flow to a limb.
- Mechanisms:
- Arterial Embolism (~80%): Clot from a proximal source (e.g., heart in A-fib) lodges distally.
- Onset: Abrupt, no prior claudication.
- In-situ Thrombosis (~20%): Clot forms on pre-existing atherosclerotic plaque (PAD).
- Onset: More gradual, often with prior claudication.
- Arterial Embolism (~80%): Clot from a proximal source (e.g., heart in A-fib) lodges distally.
⭐ Atrial fibrillation is the most common source of peripheral arterial emboli.
- Cellular Impact: Ischemia → anaerobic metabolism → cell death. Nerves & muscles most vulnerable; irreversible damage after 4-6 hours.
🦵 Clinical Manifestations - The Sinister Six Ps
📌 Mnemonic for classic signs of acute arterial occlusion. Progression reflects worsening ischemia.
- Pain: Severe, sudden onset, often the first symptom.
- Pallor: Pale or mottled skin (livedo reticularis).
- Pulselessness: Diminished or absent distal pulses.
- Paresthesia: Numbness, tingling; an early sign of nerve dysfunction.
- Paralysis: Motor weakness; a late and ominous sign.
- Poikilothermia: Coolness of the limb to touch ("perishingly cold").
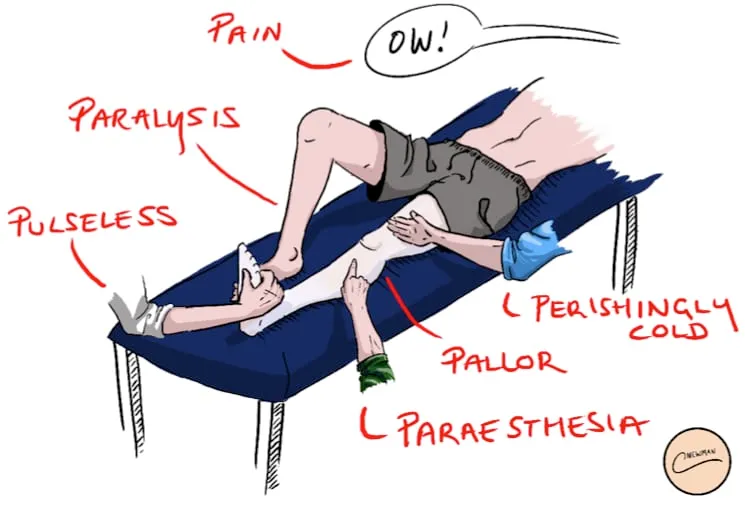
⭐ Paresthesia and paralysis are late findings. Their presence indicates a severely threatened limb, requiring immediate revascularization to prevent irreversible nerve and muscle damage.
⏱️ Diagnosis - Racing the Clock
- Clinical: Suspect with the 6 P's (Pain, Pallor, Pulselessness, Paresthesia, Paralysis, Poikilothermia).
- Initial Tests:
- Bedside Arterial Doppler: Confirms absent signals.
- Ankle-Brachial Index (ABI): Often < 0.4 or unmeasurable.
- Definitive Imaging: CT Angiography (CTA) is the gold standard to precisely locate the occlusion.
- Staging: Rutherford classification determines limb viability and urgency.
⭐ Paresthesia (sensory loss) is the first sign of nerve ischemia, indicating a threatened limb. Paralysis (motor loss) follows, signaling a more advanced, immediately threatened state (Rutherford IIb).
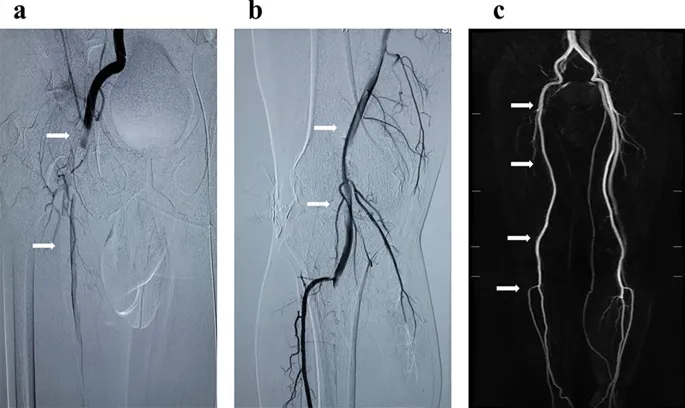
🩸 Management - Restoring the Flow
- Start immediate IV Heparin (bolus + infusion) to prevent thrombus propagation and protect collateral circulation.
- Treatment is guided by limb viability (Rutherford Classification).
- Catheter-Directed Thrombolysis (CDT):
- Infusion of alteplase (tPA) directly into the clot.
- ⚠️ Contraindicated: recent surgery/trauma, stroke (<3 mo), active bleeding.
- Surgical Revascularization:
- Embolectomy: Fogarty balloon catheter retrieves embolus.
- Bypass: Creates a new path around a thrombosed atherosclerotic segment.
- Amputation:
- For irreversible damage (Rutherford Class III) to prevent systemic toxicity.
⭐ Reperfusion Injury: After restoring flow, monitor for compartment syndrome. Key signs are severe pain on passive stretch and a tense, swollen limb. Measure compartment pressures; if >30 mmHg, perform an emergent fasciotomy.
💥 Complications - The Aftermath
- Reperfusion Injury: Restoration of blood flow releases damaging substances.
- Systemic: Hyperkalemia (arrhythmias), metabolic acidosis, rhabdomyolysis.
- Local: Edema, inflammation, free radical damage.
- Compartment Syndrome: Swelling in a closed fascial space increases pressure, compromising flow.
- ⚠️ Key Sign: Pain on passive stretch.
- Dx: Compartment pressure > 30 mmHg.
- Tx: Emergent fasciotomy.
- Acute Kidney Injury (AKI): Myoglobinuria from rhabdomyolysis causes renal tubular necrosis.
⭐ Post-reperfusion hyperkalemia is a major risk, potentially causing fatal cardiac arrhythmias. Monitor ECG and potassium levels vigilantly.
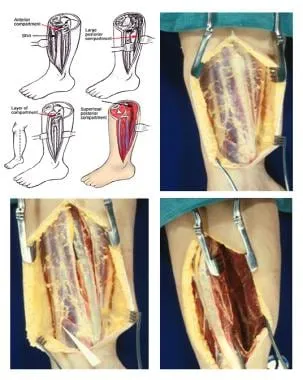
⚡ Biggest Takeaways
- Acute limb ischemia is a vascular emergency presenting with the 6 P's (Pain, Pallor, Pulselessness, Paresthesia, Paralysis, Poikilothermia).
- Immediate anticoagulation with IV heparin is the crucial first step for all patients to prevent thrombus propagation.
- Management depends on limb viability: viable limbs get urgent angiography and revascularization (catheter-directed thrombolysis or surgery).
- Threatened limbs (sensory/motor deficits) require emergent surgical revascularization to prevent tissue loss.
- Non-viable limbs (profound paralysis, absent Doppler signals) require amputation.
- Watch for reperfusion injury, leading to compartment syndrome, rhabdomyolysis, and hyperkalemia.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

