Initial Assessment - Pregnant & Puzzled
- Prioritize maternal stabilization: a stable mother is the best fetal resuscitative measure. 📌 MFA: Mother First, Always.
- Standard ATLS protocol (ABCDEs) with key modifications:
- A/B: Assume difficult airway; ↓ functional residual capacity means rapid desaturation.
- C: Aggressive fluid resuscitation. Manually displace uterus to the left to relieve aortocaval compression after 20 weeks gestation.
- Establish 2 large-bore IVs.
- Secondary survey includes fetal & uterine assessment:
- Cardiotocography for viable fetus (≥24 weeks).
- Check for vaginal bleeding, amniotic fluid, or uterine contractions.
⭐ A pregnant patient can lose up to 30-35% of her blood volume before showing signs of hypotension, as physiologic hypervolemia masks early shock.
Primary Survey - Mama's ABCs
- A (Airway): High risk of difficult intubation due to airway edema. Low threshold for definitive airway.
- B (Breathing): ↑ O₂ demand. Provide high-flow supplemental O₂. Chest tube insertion site is higher (e.g., 3rd-4th intercostal space) due to the elevated diaphragm.
- C (Circulation):
- Secure 2 large-bore IVs. Aggressive fluid resuscitation.
- Crucial: Perform left uterine displacement (LUD) by tilting the patient 15-30° to the left to decompress the inferior vena cava (IVC).
- ⚠️ Hypotension is a late and ominous sign; significant blood loss (30-35%) can occur before vitals change.
⭐ Exam Favorite: Fetal distress (tachycardia, bradycardia, late decelerations) is often the first sign of maternal hypovolemia, appearing long before maternal hypotension.
Secondary Survey - Baby's Check-in
- Fetal Heart Tones (FHTs): Initial check with Doppler; confirms viability.
- Cardiotocography (CTG): Continuous monitoring for ≥4-6 hours for all viable pregnancies post-trauma.
- Monitors for contractions & fetal distress (e.g., decelerations).
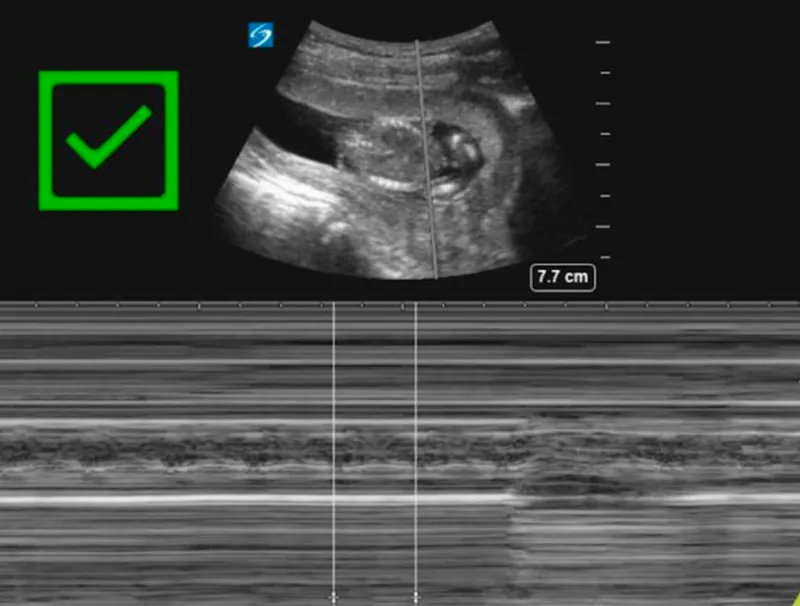
- Bedside Ultrasound:
- Check for fetal cardiac activity, placental location (r/o previa), and amniotic fluid volume.
- Not sensitive for abruption initially.
- Kleihauer-Betke (KB) Test: Consider if concerned for feto-maternal hemorrhage to quantify bleed & guide RhoGAM dose.
- Rho(D) Immunoglobulin: Administer to all Rh-negative mothers after trauma.
⭐ High-Yield: The most common cause of fetal death after trauma is maternal death or shock. However, placental abruption is the most frequent serious pregnancy-specific complication.
Specific Injuries - Trauma's Triple Threat
Trauma can precipitate three catastrophic obstetric emergencies. Rapid differentiation is key, as clinical overlap exists but management diverges critically.
| Injury | Key Presentation | Fetal Heart Rate (FHR) | Management Pearls |
|---|---|---|---|
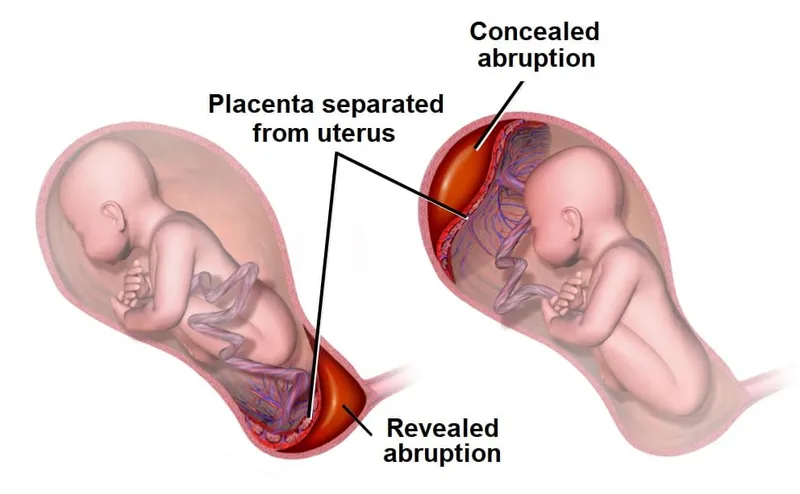
| Placental Abruption | Painful vaginal bleeding (can be concealed), uterine hypertonus, tender/firm uterus. | Late decelerations, ↓ variability, sinusoidal pattern. | Kleihauer-Betke test for feto-maternal hemorrhage. Immediate C-section for distress. |
| Uterine Rupture | Sudden, severe abdominal pain; loss of fetal station; easily palpable fetal parts. | Profound bradycardia, terminal decelerations, loss of FHR. | High risk with prior classical C-section. Emergency laparotomy & delivery. |
| Amniotic Fluid Embolism | Sudden CV collapse, severe hypoxia, seizures, rapid disseminated intravascular coagulation (DIC). | Catastrophic FHR changes (sudden bradycardia). | Supportive care is paramount (ACLS, massive transfusion protocol). |
📌 Mnemonic (AFE): Remember the triad of Hypotension, Hypoxia, and Hemorrhage (DIC).
High‑Yield Points - ⚡ Biggest Takeaways
- Maternal stabilization is always the first priority; a healthy mother is necessary for a healthy fetus.
- Place patient in the left lateral decubitus position to prevent aortocaval compression and improve venous return.
- Placental abruption is the most common pregnancy-specific complication of trauma, often presenting with vaginal bleeding and uterine tenderness.
- Administer Rho(D) immune globulin to all Rh-negative pregnant trauma patients.
- Use the Kleihauer-Betke test to screen for fetomaternal hemorrhage.
- Continuous fetal monitoring is crucial if the fetus is viable (typically >24 weeks).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

