Indications & Contraindications - The 'Go or No-Go' Code
Decisions hinge on injury mechanism and signs of life (SOL).
-
Primary Indications (Penetrating > Blunt):
- Penetrating Thoracic Trauma: Witnessed arrest with prehospital CPR < 15 min.
- Blunt Trauma: Witnessed arrest with prehospital CPR < 10 min & PEA.
- Persistent post-injury hypotension (SBP < 60 mmHg) despite aggressive resuscitation.
-
Absolute Contraindications:
- No SOL in the field.
- Asystole as presenting rhythm (unless tamponade is suspected).
- Severe, non-survivable brain injury.
- CPR duration exceeding time limits.
⭐ Exam Favorite: The highest survival rates are seen in patients with isolated penetrating cardiac injuries (e.g., stab wounds) who lose pulses in the emergency department.
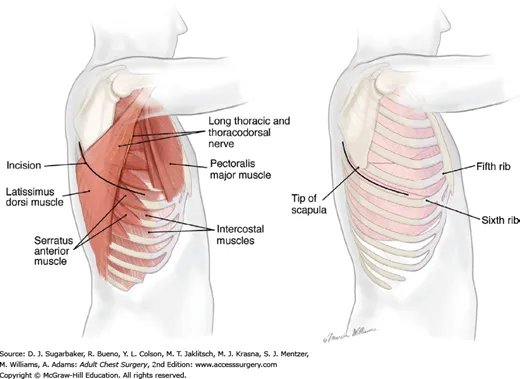
Procedure Steps - The Thoracotomy Tango
- Incision & Entry:
- Anterolateral thoracotomy in the 4th or 5th intercostal space (inframammary crease).
- Use scalpel, then bluntly dissect with fingers or clamps through intercostal muscles.
- Divide the pleura to enter the chest.
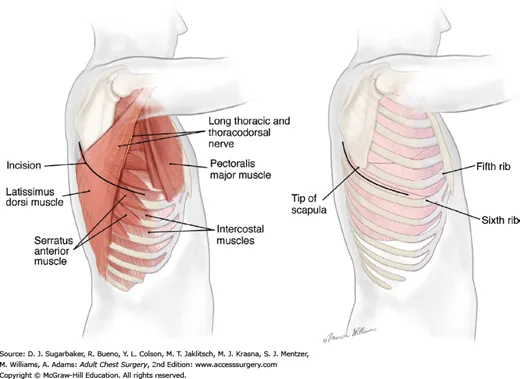
- The Dance Floor:
- Insert rib spreaders (Finochietto) with the handle down.
- Retract the lung posteriorly.
- Core Moves:
- Pericardiotomy: Incise pericardium anterior to the phrenic nerve.
- Cardiac Repair: Use finger pressure, sutures, or staples.
- Aortic Cross-Clamping: Occlude descending aorta to redirect blood flow to coronaries/brain.
⭐ High-Yield: Cross-clamp the descending thoracic aorta just distal to the origin of the left subclavian artery to preserve cerebral and coronary perfusion without compromising spinal cord blood flow unnecessarily.
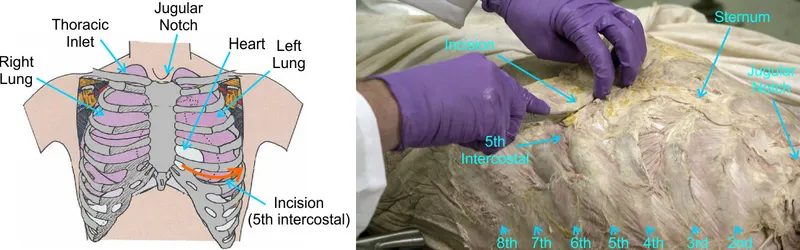
Anatomy & Key Maneuvers - Navigating the Red Sea
- Incision: Left anterolateral thoracotomy in the 5th intercostal space (ICS), from sternum to posterior axillary line.
- Pericardiotomy: Open pericardial sac anterior to the phrenic nerve to release tamponade.
- Maneuvers:
- Aortic Cross-Clamping: Controls infra-diaphragmatic bleeding; improves coronary perfusion.
- Hilar Control: Twist or clamp hilum for massive pulmonary hemorrhage.
- Internal Cardiac Massage: Direct manual compression of the heart.
⭐ To avoid paralysis of the hemidiaphragm, the pericardiotomy incision must be made anterior to the phrenic nerve.
Outcomes & Complications - The Final Tally
- Survival Rates: Highly dependent on mechanism and location of injury.
- Penetrating Thoracic Trauma: ~10-15%
- Blunt Trauma: <2%
- Neurologic Sequelae: Anoxic brain injury is the most feared complication in survivors; many have significant permanent deficits.
- Common Complications:
- Infection (empyema, mediastinitis)
- Coagulopathic bleeding
- Phrenic nerve injury
- Iatrogenic organ damage
⭐ Survival is exceedingly rare in blunt trauma patients who have had no signs of life in the field.
- Resuscitative thoracotomy is a last-resort procedure for patients in extremis from penetrating chest trauma.
- Primary goals are to relieve cardiac tamponade, control intrathoracic hemorrhage, and perform open cardiac massage.
- A left anterolateral thoracotomy in the 5th intercostal space is the standard approach.
- Cross-clamping the descending aorta is crucial to redirecting blood flow to the brain and heart.
- Survival is extremely low, especially following blunt trauma (<2%).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

