Indications & Selection - Sweet New Glands
- Primary Indication: Type 1 Diabetes (T1DM) with severe, life-threatening complications, often alongside renal failure.
- Main Categories:
- Simultaneous Pancreas-Kidney (SPK): Most common. For T1DM with end-stage renal disease (ESRD).
- Pancreas After Kidney (PAK): For T1DM patients with a prior kidney transplant.
- Pancreas Transplant Alone (PTA): For T1DM with severe metabolic instability (e.g., hypoglycemic unawareness) but adequate renal function.
- Core Criteria: C-peptide negative, adequate cardiac reserve.
⭐ The most common procedure is the Simultaneous Pancreas-Kidney (SPK) transplant for T1DM patients who also require a kidney.
Surgical Techniques - Plumbing the Pancreas
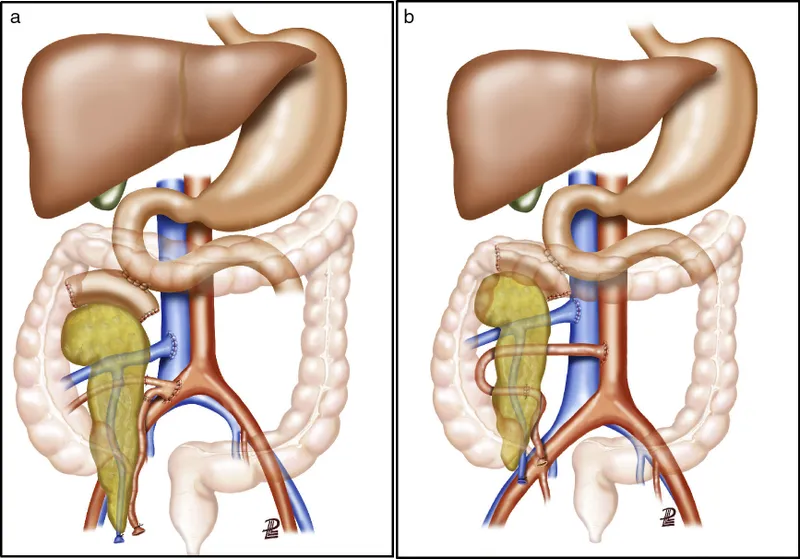
- Goal: Anastomose donor pancreas vessels & manage exocrine drainage.
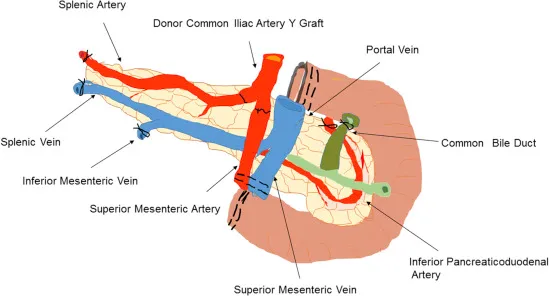
- Vascular Anastomosis:
- Arterial Supply: Donor iliac artery Y-graft (supplying splenic & superior mesenteric arteries) connected to recipient's iliac artery.
- Venous Drainage: Donor portal vein connected to recipient's superior mesenteric or iliac vein.
- Exocrine Drainage:
- Enteric (most common): Donor duodenum to recipient jejunum.
- Bladder (historic): Donor duodenum to recipient bladder; allows urine amylase monitoring for rejection.
⭐ The vast majority of transplants now use enteric drainage due to lower rates of metabolic acidosis, reflux pancreatitis, and UTIs.
Immunosuppression - Rejection Rejection!
- Induction & Maintenance: Typically a triple-drug regimen.
- Calcineurin Inhibitor (e.g., Tacrolimus)
- Antimetabolite (e.g., Mycophenolate Mofetil)
- Corticosteroids
- Acute Rejection: Suspect with unexplained hyperglycemia & ↑ serum amylase/lipase. Biopsy is gold standard for diagnosis.
- Treatment: Initially with steroid boluses. Use lymphocyte-depleting agents (e.g., ATG) for steroid-resistant cases.
⭐ Venous thrombosis is the most common non-immunologic cause of early graft loss.
Complications - Transplant Troubles
- Early Graft Loss:
- Vascular Thrombosis: Venous > Arterial. Often requires graft pancreatectomy. A leading cause of technical failure.
- Rejection:
- Acute Cellular (ACR): T-cell mediated. Dx: Biopsy. Tx: Steroids, anti-T-cell antibodies.
- Chronic: Antibody-mediated, leads to fibrosis/vasculopathy.
- Infections (immunosuppression-related):
- CMV, Polyomavirus (BK virus), fungal infections.
- Surgical/Anastomotic:
- Leaks: From enteric or bladder drainage sites.
- Graft Pancreatitis: Presents with ↑ serum amylase/lipase.
⭐ Venous thrombosis is the leading cause of non-immunologic graft failure in the early post-operative period.
Islet Cell Transplant - Just the Cells, Ma'am
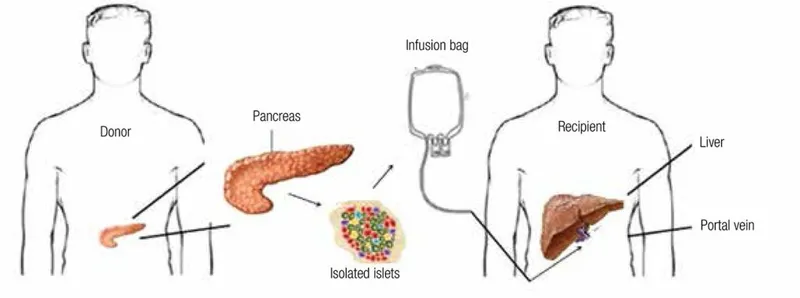
- Concept: Minimally invasive procedure where islets are isolated from a donor pancreas and infused into the recipient's portal vein.
- Primary Indication: Type 1 diabetes with severe hypoglycemia unawareness and glycemic lability, despite optimal medical management.
- Mechanism: Islets lodge in the liver sinusoids, engraft, and secrete insulin directly into the portal circulation.
⭐ Exam Favorite: A major limitation is the need for a large islet mass, often requiring cells from 2 or more donor pancreata for a single recipient to achieve insulin independence.
High‑Yield Points - ⚡ Biggest Takeaways
- SPK transplant (Simultaneous Pancreas-Kidney) is the most common procedure for Type 1 diabetes with ESRD.
- Vascular thrombosis is the leading cause of early graft loss, especially in the first 24-48 hours.
- Enteric drainage is now preferred over bladder drainage to avoid metabolic acidosis and urologic complications.
- Acute rejection presents with rising serum amylase/lipase and hyperglycemia; biopsy is diagnostic.
- Lifelong triple-drug immunosuppression is mandatory, increasing risk for opportunistic infections like CMV.
- Islet cell transplantation is less invasive but offers lower rates of long-term insulin independence.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

