Rejection Basics - Host vs. Graft
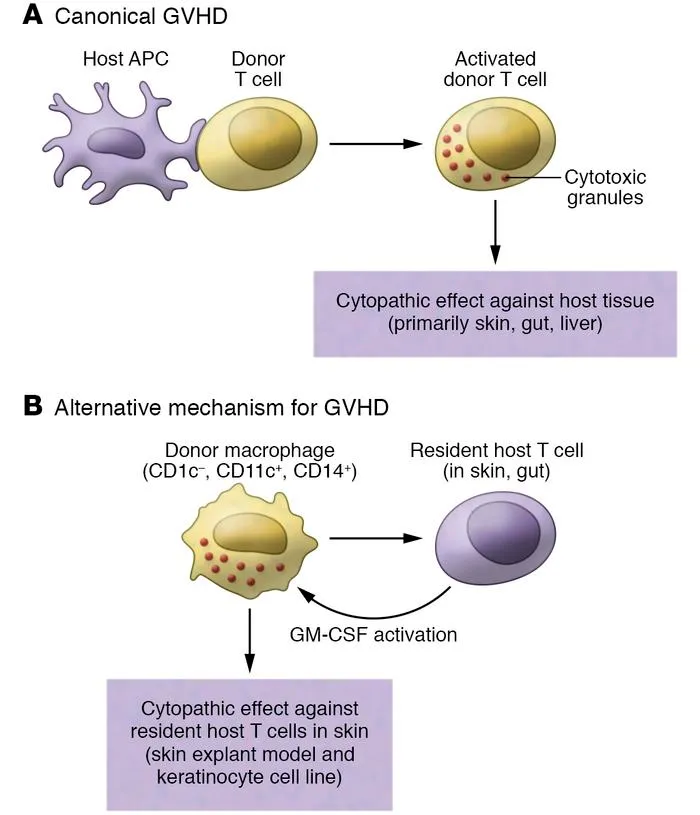
- Graft-vs-Host Disease (GVHD): Occurs when donor T-cells (from the graft) recognize the recipient's body (host) as foreign and mount an immune attack.
- Key Mediator: Donor T-lymphocytes, particularly cytotoxic T-cells, targeting host tissues.
- Common Manifestations (Triad):
- Skin: Maculopapular rash
- Liver: Jaundice, elevated liver enzymes
- GI Tract: Diarrhea, abdominal pain, nausea
⭐ GVHD is most commonly associated with bone marrow/stem cell and liver transplants.
The Drug Arsenal - Taming the T-Cell
- Primary Goal: Inhibit T-cell activation, the central driver of acute rejection. This process requires three distinct signals.
- Calcineurin Inhibitors (CNIs): Tacrolimus & Cyclosporine.
- Block Signal 1 by inhibiting calcineurin, preventing IL-2 production.
- Toxicity: Nephrotoxicity, neurotoxicity (tremor), HTN, hyperglycemia.
- mTOR Inhibitors: Sirolimus & Everolimus.
- Block Signal 3 by inhibiting mTOR, blocking IL-2-driven proliferation.
- Toxicity: Pancytopenia, delayed wound healing, hyperlipidemia.
- Antimetabolites: Mycophenolate Mofetil (MMF) & Azathioprine.
- Inhibit purine synthesis, starving proliferating lymphocytes.
- Toxicity: MMF (GI distress), Azathioprine (myelosuppression).
⭐ CNI-induced nephrotoxicity is a major cause of chronic allograft dysfunction, causing afferent arteriole vasoconstriction and chronic fibrosis.
Toxicities & Side Effects - The Nasty Sidekicks
-
Calcineurin Inhibitors (Tacrolimus, Cyclosporine):
- Nephrotoxicity: Acute (afferent arteriole vasoconstriction) & chronic (fibrosis).
- Neurotoxicity: Tremors, headache, seizures.
- Metabolic: Hypertension, ↑ lipids, ↑ glucose (esp. Tacrolimus).
- Cyclosporine-specific: Gingival hyperplasia, Hirsutism.
-
Antiproliferatives:
- Mycophenolate (MMF): GI distress (diarrhea), leukopenia.
- Azathioprine: Dose-related myelosuppression (check TPMT), pancreatitis.
-
mTOR Inhibitors (Sirolimus, Everolimus):
- Pancytopenia, poor wound healing, mouth ulcers (stomatitis).
- Hyperlipidemia/Hypertriglyceridemia.
-
Corticosteroids (Prednisone):
- Cushingoid features, osteoporosis, hyperglycemia, avascular necrosis, cataracts.
⭐ Calcineurin inhibitor nephrotoxicity is a major cause of long-term allograft dysfunction. It's primarily mediated by dose-dependent vasoconstriction of the afferent arterioles, leading to a ↓ GFR.
Clinical Regimens - The Balancing Act
-
Induction Therapy (Peri-transplant): High-dose agents to prevent hyperacute/acute rejection.
- Antibodies: Basiliximab (IL-2R blocker), Alemtuzumab, Antithymocyte Globulin.
- High-dose corticosteroids.
-
Maintenance Therapy (Lifelong): A multi-drug approach to prevent chronic rejection.
- Cornerstone: Calcineurin Inhibitor (CNI) (e.g., Tacrolimus) + Antimetabolite (e.g., Mycophenolate Mofetil) ± Corticosteroids.
-
Rejection Treatment: For acute episodes, typically pulse high-dose corticosteroids.
⭐ The primary challenge is balancing under-immunosuppression (risk of rejection) against over-immunosuppression, which leads to opportunistic infections (CMV, BK virus) and malignancy (PTLD, skin cancer).
High‑Yield Points - ⚡ Biggest Takeaways
- Calcineurin inhibitors (e.g., Tacrolimus) are the backbone of therapy but are highly nephrotoxic.
- Antimetabolites (e.g., Mycophenolate) inhibit lymphocyte proliferation, causing bone marrow suppression.
- mTOR inhibitors (e.g., Sirolimus) block T-cell signaling but classically impair wound healing.
- Corticosteroids are used for induction and managing acute rejection.
- Induction therapy with IL-2R antagonists (Basiliximab) prevents early acute rejection.
- Prophylaxis against PCP and CMV is a standard of care.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

