Indications & Contraindications - The Gatekeepers' List
-
Indications: Generally, end-stage heart disease with <1 year life expectancy.
- Refractory cardiogenic shock, NYHA Class III-IV HF
- Intractable angina or malignant arrhythmias
- LVEF <20%
- Peak VO₂ <14 mL/kg/min
-
Contraindications:
- Absolute:
- Active malignancy
- Severe, irreversible pulmonary hypertension (PVR >5 Wood units)
- Irreversible end-organ damage (e.g., liver, kidney)
- Active systemic infection
- Relative:
- Age >70
- Poorly controlled diabetes
- Active substance abuse
- Psychosocial instability
- Absolute:
⭐ Exam Favorite: Irreversible pulmonary hypertension (high Pulmonary Vascular Resistance) is a critical absolute contraindication, as the donor right ventricle is not accustomed to high afterload and will fail.
Donor-Recipient Matching - The Perfect Match
Key matching criteria aim to minimize rejection and maximize graft survival.
- ABO Blood Group: Must be identical or compatible.
- Panel Reactive Antibody (PRA): Screens for pre-formed HLA antibodies. A high PRA indicates sensitization, making matching difficult.
- Size Match: Donor weight should be within 30% of the recipient's weight.
⭐ Cytomegalovirus (CMV) status is critical. A CMV-negative recipient should ideally receive a CMV-negative heart to prevent primary infection, a major cause of post-transplant morbidity.
Surgical Procedure - The New Engine Swap
- Standard Approach: Median sternotomy & initiation of cardiopulmonary bypass (CPB).
- Orthotopic Transplant (Biatrial Technique): Recipient's heart is explanted, leaving posterior walls of the atria with vena cavae and pulmonary veins intact.
- Anastomosis Sequence: Left atrium → Right atrium → Pulmonary artery → Aorta.
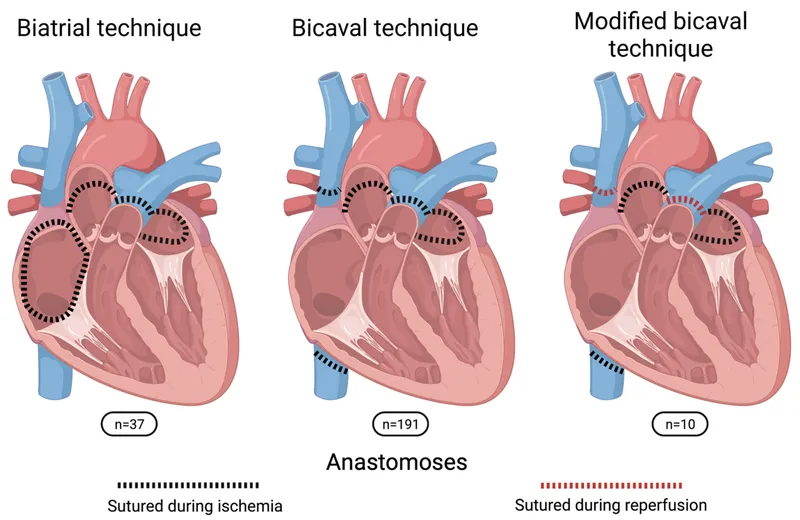
⭐ EKG Finding: The recipient's native sinoatrial (SA) node remnant can remain functional, leading to two P-waves (one from donor, one from recipient) on post-op EKG.
Immunosuppression & Rejection - Taming the Defenses
-
Induction Therapy: Basiliximab (IL-2R antagonist) at time of transplant.
-
Maintenance (Triple Drug Regimen):
- Calcineurin Inhibitor (CNI): Tacrolimus (preferred) or Cyclosporine.
- Antiproliferative: Mycophenolate Mofetil (MMF) or Azathioprine.
- Corticosteroids: Prednisone, with gradual taper.
-
Types of Rejection:
- Hyperacute: Minutes; pre-formed antibodies; causes thrombosis.
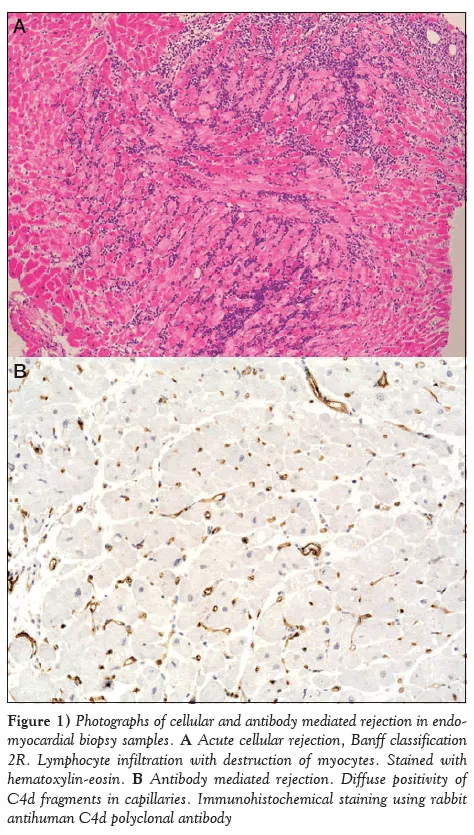
- Acute Cellular: 1-12 weeks; T-cell mediated; diagnosed via biopsy.
- Antibody-Mediated (AMR): Can occur anytime; donor-specific antibodies (DSAs).
- Chronic: >1 year; leads to Cardiac Allograft Vasculopathy (CAV).
⭐ Endomyocardial biopsy is the gold standard for monitoring and diagnosing acute cardiac allograft rejection, revealing lymphocytic infiltrate and myocyte damage.
Complications & Prognosis - The Long Road Ahead
- Infection: Highest risk in first year. Prophylaxis is key.
- Timeline: Bacterial (early) → Opportunistic (CMV, Pneumocystis) → Fungal (late).
- Malignancy: Due to ↓ immune surveillance.
- Most common: Skin cancers (Squamous Cell > Basal Cell).
- Post-transplant Lymphoproliferative Disorder (PTLD), often EBV-driven.
- Graft Failure:
- Acute/chronic rejection.
- Cardiac Allograft Vasculopathy (CAV).
⭐ Cardiac Allograft Vasculopathy (CAV) is a diffuse, accelerated form of coronary artery disease and the leading cause of graft failure >1 year post-transplant.
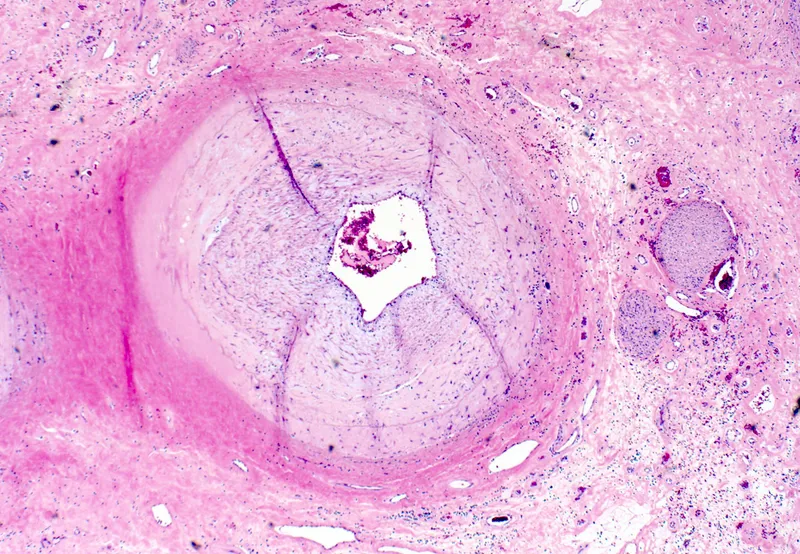
- Prognosis: Median survival is ~12-13 years. 1-year survival >85%.
High‑Yield Points - ⚡ Biggest Takeaways
- Orthotopic transplantation is the standard for end-stage heart failure refractory to medical therapy.
- Key contraindications include irreversible pulmonary hypertension, active malignancy, and systemic infection.
- Endomyocardial biopsy is the gold standard for diagnosing acute cellular rejection.
- Cardiac Allograft Vasculopathy (CAV) is a major long-term cause of graft failure, presenting as diffuse coronary stenosis.
- Lifelong triple-drug immunosuppression increases risk of infection (CMV) and malignancy.
- The denervated donor heart has a higher resting heart rate and is unresponsive to atropine.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

