Wound Complications - The Unraveling
- Dehiscence: Post-op separation of fascial layers, often preceded by serosanguinous discharge.
- Evisceration: Protrusion of abdominal organs through the fascial defect. A surgical emergency.
Key Risk Factors: Infection, malnutrition (albumin < 3.5), obesity, ↑intra-abdominal pressure (coughing, ileus), steroid use.
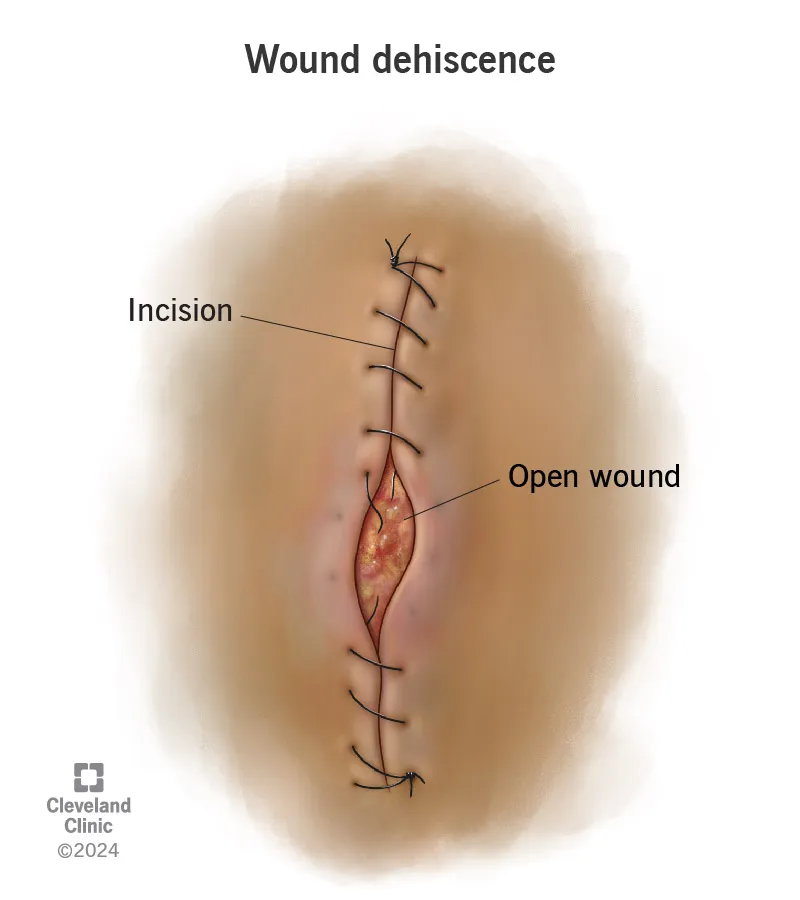
⭐ A sudden gush of "salmon-colored" (serosanguinous) fluid from the incision is a classic sign of impending fascial dehiscence.
Risk Factors - Setting the Stage
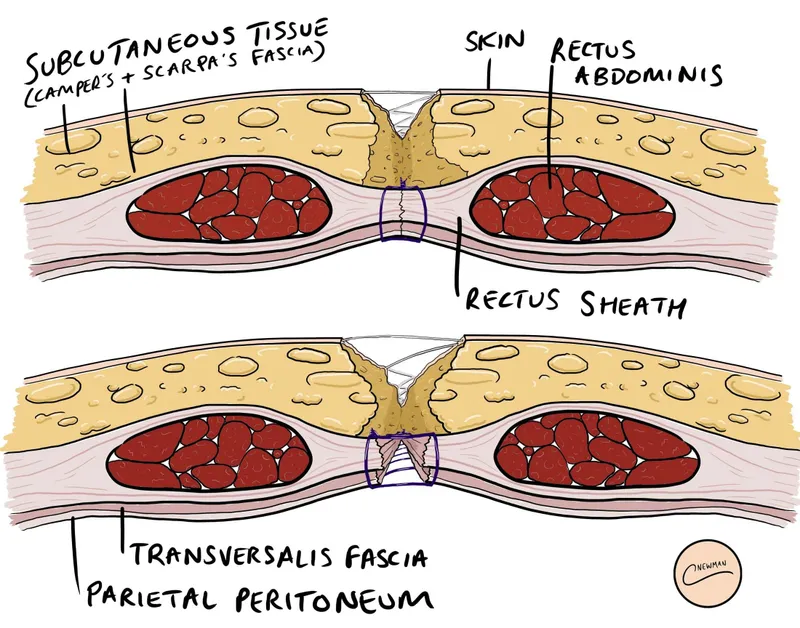
-
Patient-Specific Factors:
- Poor nutrition (Albumin < 3.5 g/dL, Vit C deficiency)
- Comorbidities: Diabetes, obesity (BMI > 30), jaundice, uremia
- Immunosuppression: Steroids, chemotherapy, advanced age
- Tissue hypoxia: Smoking, anemia
-
Local & Technical Factors:
- ↑ Intra-abdominal pressure: Coughing, vomiting, ileus, ascites
- Wound environment: Surgical site infection (SSI), hematoma
- Surgical technique: Improper suture placement, tension on closure
⭐ Most dehiscences occur on postoperative days 5-8, when wound tensile strength is minimal before significant collagen deposition.
Presentation & Diagnosis - Spotting the Split
- Wound Dehiscence: Partial or complete separation of fascial layers, often concealed beneath intact skin.
- Patient may report a sudden “popping” sensation during straining.
- Profuse serosanguinous (salmon-colored) drainage is a pathognomonic sign.
- Wound Evisceration: Protrusion of intra-abdominal contents (e.g., omentum, bowel) through the separated layers. This is a surgical emergency.
- Diagnosis: Primarily clinical, confirmed by gentle probing of the incision with a sterile applicator.
⭐ Most cases occur between postoperative days 5-8, when wound tensile strength is at its minimum before significant collagen deposition.
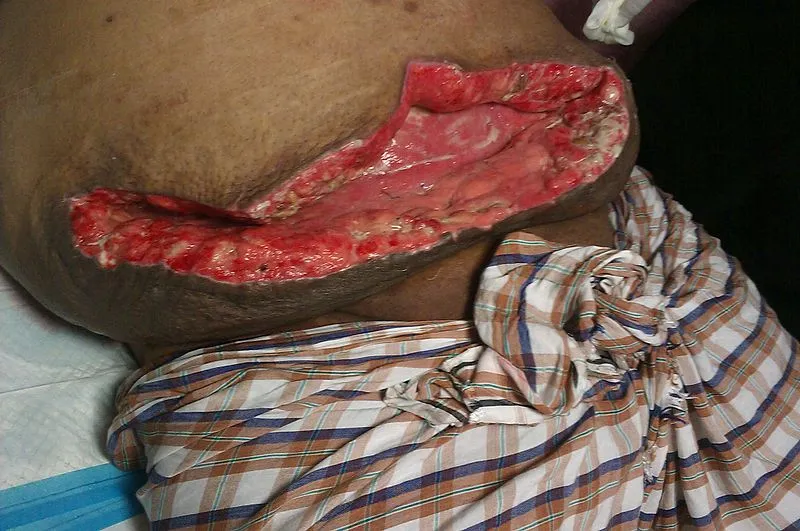
Management - The Fix-It Plan
Immediate intervention is critical, especially for evisceration. The management strategy depends entirely on the integrity of the fascial layer.
⭐ Surgical evisceration is a surgical emergency with a mortality rate of up to 15-20%, often due to sepsis and fluid/electrolyte loss.
Prevention - Closing the Door
- Pre-operative Optimization: Address modifiable risk factors. Control blood glucose, improve nutritional status (protein, vitamins), and encourage smoking cessation.
- Intra-operative Technique:
- Achieve a tension-free fascial closure.
- Use slowly-absorbing or non-absorbable sutures.
- Place sutures 1 cm from the fascial edge and 1 cm apart.
- Avoid tissue ischemia by not tying sutures too tightly.
⭐ A suture length to wound length (SL:WL) ratio of 4:1 or greater significantly reduces dehiscence risk.
High‑Yield Points - ⚡ Biggest Takeaways
- Wound dehiscence is the separation of fascial layers; evisceration involves organ protrusion through the defect.
- Both typically occur 5-8 days post-op, often heralded by a "popping" sensation and serosanguinous (salmon-colored) drainage.
- The most critical risk factor is inadequate fascial closure; others include obesity, malnutrition, and ↑ intra-abdominal pressure.
- Evisceration is a surgical emergency; immediately cover protruding contents with sterile, saline-soaked dressings.
- Definitive management for both is an urgent return to the operating room for fascial re-closure.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

