Virchow's Triad - The Clotting Trifecta
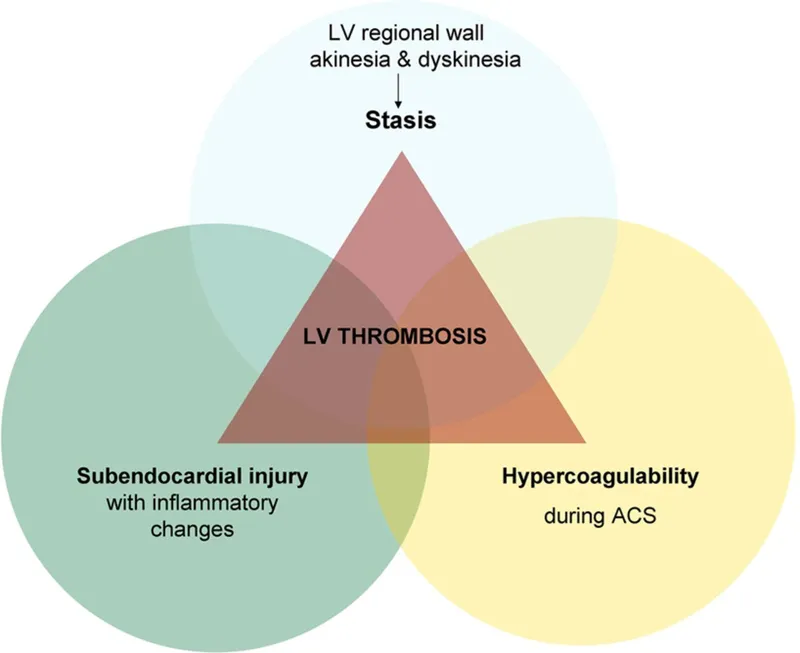
Three primary abnormalities in blood composition, flow, and vessel wall that predispose to thrombosis. 📌 Mnemonic: SHE
- Stasis: Reduced blood flow.
- Immobilization (post-op, paralysis, long travel).
- Cardiac dysfunction (atrial fibrillation, heart failure).
- Hypercoagulability: Increased tendency to clot.
- Inherited: Factor V Leiden, prothrombin gene mutation.
- Acquired: Malignancy, pregnancy, OCPs, sepsis.
- Endothelial Injury: Damage to the vessel lining.
- Trauma, surgery, IV catheters, atherosclerosis.
⭐ Factor V Leiden is the most common inherited thrombophilia, causing resistance to activated protein C.
DVT Diagnosis & Management - Deep Trouble Leg Day
- Diagnosis:
- Wells Score: Stratifies pre-test probability. >2 = DVT likely.
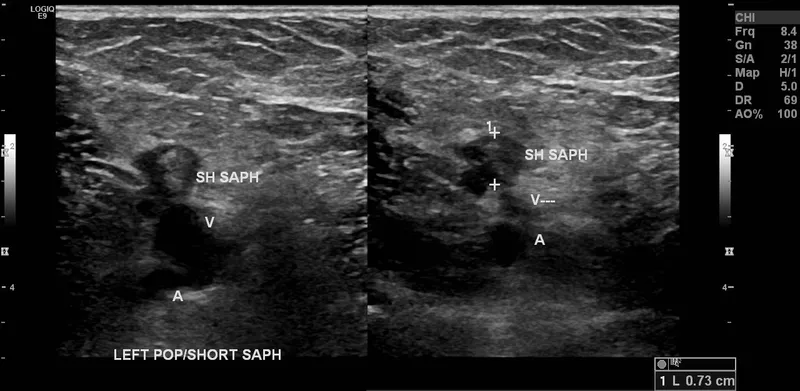
- First-line Imaging: Compression ultrasonography with Doppler. Shows non-compressible vein.
- D-Dimer: High negative predictive value. Used to rule out DVT in low-probability patients (Wells score <2).
- Management:
- Anticoagulation: LMWH or DOACs (e.g., apixaban, rivaroxaban) for at least 3 months.
- IVC Filter: For patients with contraindications to anticoagulation (e.g., active bleeding).
⭐ Phlegmasia Cerulea Dolens: A rare, limb-threatening complication of massive DVT causing venous outflow obstruction, intense pain, cyanosis, and edema.
Pulmonary Embolism - Lethal Lung Lodger
- Pathophysiology: Occlusion of pulmonary arteries, most commonly from a dislodged deep vein thrombus (DVT).
-
Presentation: Sudden-onset dyspnea, pleuritic chest pain, tachypnea, and tachycardia. Hemoptysis can occur.
- 📌 Virchow's Triad (risk factors): Stasis, Hypercoagulability, Endothelial injury.
-
Diagnosis:
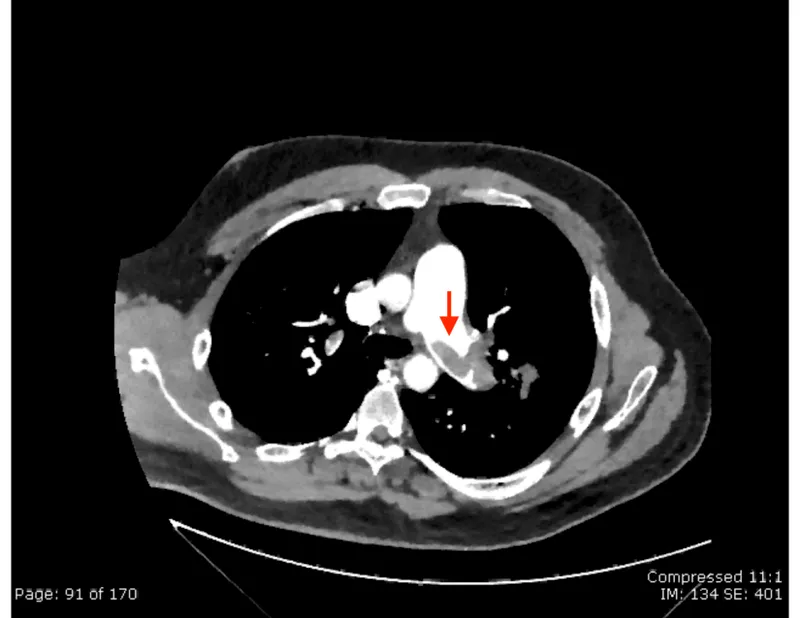
- Best initial test: CT Pulmonary Angiography (CTPA) is the gold standard.
- V/Q Scan: Used if CTPA is contraindicated (e.g., renal failure, contrast allergy).
- D-dimer: High negative predictive value; useful to rule out PE in low-risk patients.
⭐ Physiological Dead Space: In PE, ventilated lung segments are not perfused, leading to a profound ventilation/perfusion (V/Q) mismatch. This is the primary cause of hypoxemia.
- Management:
- Anticoagulation: Immediate start with Heparin or LMWH, bridged to Warfarin or a DOAC.
- Thrombolysis: For massive PE with hemodynamic instability.
VTE Prophylaxis - Clot Blockers United
- Risk Stratification: Use the Caprini score to guide therapy intensity for surgical patients.
- Mechanical Methods: Primarily for patients at high risk of bleeding.
- Intermittent Pneumatic Compression (IPCs).
- Graduated Compression Stockings (GCS).
- Pharmacological Agents: The mainstay for moderate-to-high risk patients.
- LMWH: Enoxaparin 40mg SC daily.
- UFH: 5000 units SC q8-12h.
- Fondaparinux: Use if history of HIT.
- Early Ambulation: A crucial baseline intervention for all postoperative patients.
⭐ Pharmacologic prophylaxis is contraindicated in patients with active bleeding, severe bleeding diathesis, or a platelet count < 50,000/μL.
📌 VTE Prevention: Very Early ambulation, Thrombotics, External compression.
- Virchow's triad (stasis, hypercoagulability, endothelial injury) is the cornerstone of pathophysiology.
- Pulmonary embolism (PE) is the most common preventable cause of death in hospitalized patients.
- Major risk factors include orthopedic/pelvic surgery, malignancy, and prolonged immobility.
- Prophylaxis is key: early ambulation, pneumatic compression, and pharmacologic agents (LMWH).
- Diagnose DVT with duplex ultrasound; diagnose PE with CT angiography.
- Treatment involves systemic anticoagulation; consider an IVC filter if contraindicated.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

