SSI Classification - Skin Deep or More
- Superficial Incisional SSI:
- Involves only skin and subcutaneous tissue.
- Occurs within 30 days post-procedure.
- Presents with purulent drainage, positive cultures, or localized inflammation.
- Deep Incisional SSI:
- Affects deep soft tissues (fascia, muscle).
- Occurs within 90 days (no implant) or up to 1 year (with implant).
- Organ/Space SSI:
- Involves any organ or anatomical space opened or manipulated during surgery.
- Timeline is identical to Deep Incisional SSI.
⭐ Staphylococcus aureus is the most frequent pathogen isolated from SSIs.

Risk Factors & Bugs - Who's at Risk?
- Patient Factors:
- Obesity (BMI > 30), smoking, malnutrition
- Poorly controlled diabetes (HbA1c > 7%)
- Immunosuppression (steroids, chemotherapy)
- Nasal colonization with S. aureus
- Procedural Factors:
- Wound classification (Dirty > Contaminated)
- Prolonged duration, emergency surgery
- Hypothermia, poor surgical technique
- Common Pathogens:
- Staphylococcus aureus: Most common cause.
- Coagulase-negative staphylococci: With prosthetic implants.
- Gram-negatives/anaerobes (E. coli, Bacteroides): GI/GU surgery.
⭐ Rapidly progressing infections (<48 hrs) with severe pain and systemic signs suggest aggressive pathogens like S. pyogenes or Clostridium perfringens.
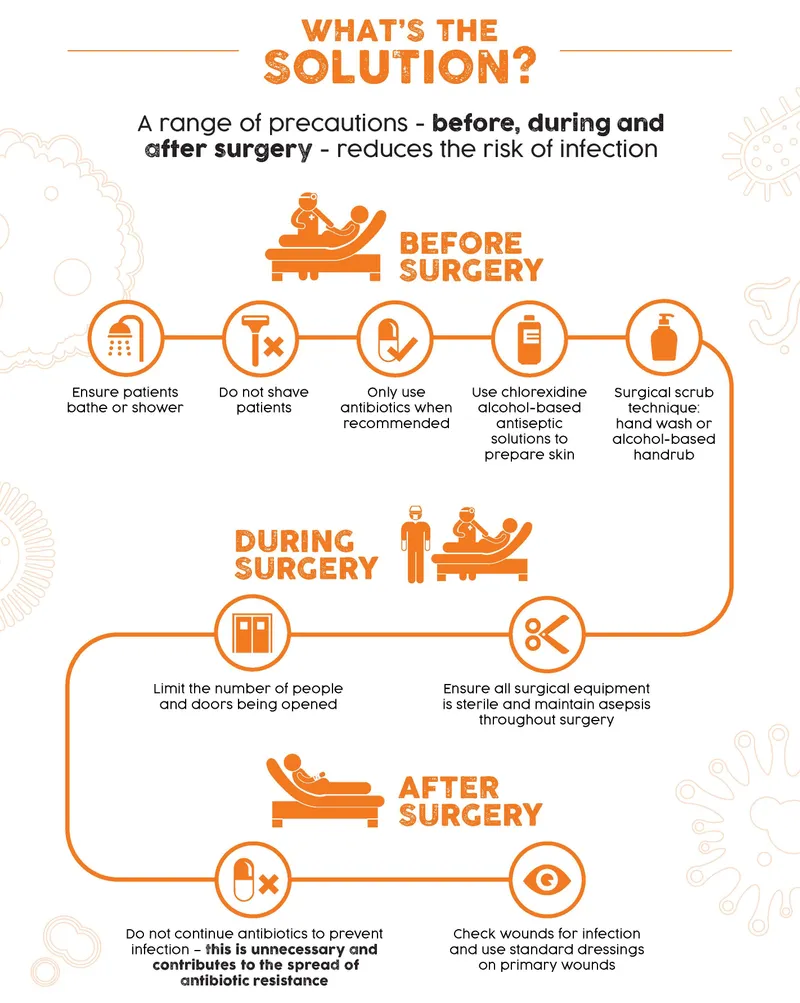
Prevention - Guarding the Gateway
- Pre-operative Prep:
- Optimize patient: Control glucose (<180 mg/dL), cease smoking (4-6 wks prior), improve nutrition.
- Pre-op shower with chlorhexidine gluconate (CHG).
- Nasal mupirocin for known MRSA/MSSA carriers.
- Intra-operative Shield:
- Antimicrobial Prophylaxis:
- Administer within 60 mins before incision (120 mins for vancomycin/fluoroquinolones).
- Common agent: Cefazolin.
- Redose for long procedures or significant blood loss.
- Aseptic Technique:
- Skin prep: Chlorhexidine-alcohol preferred.
- Maintain normothermia and glycemic control.
- Antimicrobial Prophylaxis:
- Post-operative Care:
- Sterile dressing for 24-48 hours.
- Discontinue prophylactic antibiotics within 24 hours of surgery completion.
⭐ The most common organism causing SSIs is Staphylococcus aureus. Prophylactic antibiotics are not for treating infection but for reducing the bacterial burden at the time of incision.
Diagnosis & Treatment - Spot and Stop
- Diagnosis:
- Clinical signs: New/worsening pain, erythema, induration, warmth, purulent drainage.
- Systemic signs: Fever >38°C, leukocytosis.
- Definitive: Wound culture & sensitivity.
- Imaging (CT/US) for suspected deep/organ space abscesses.

- Treatment Algorithm:
- Antibiotics: Tailor to culture. Empiric therapy targets Staph aureus (Vancomycin for MRSA risk). For GI/GU source, add gram-negative & anaerobic coverage.
⭐ Most SSIs manifest 5-7 days post-op. Infection in the first 48 hours suggests highly virulent organisms like Streptococcus pyogenes (Group A Strep) or Clostridium perfringens.
High‑Yield Points - ⚡ Biggest Takeaways
- Staphylococcus aureus is the most common cause of surgical site infections (SSIs).
- Administer prophylactic antibiotics, usually Cefazolin, within 60 minutes before the initial incision.
- Use Vancomycin for prophylaxis in patients with a history of MRSA colonization.
- A new-onset fever occurring post-operative day 5 to 7 is highly suspicious for an SSI.
- The cornerstone of management is source control, including incision and drainage of any abscess.
- For colorectal surgeries, prophylaxis must cover gram-negative and anaerobic organisms.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

