Atelectasis - The Collapsing Lung Blues
- Most common post-op pulmonary complication, peaks at 24-48 hours.
- Pathophysiology: Alveolar collapse from airway obstruction (mucus plugs) and shallow breathing, leading to a V/Q mismatch.
- Findings: ↓ breath sounds, dullness to percussion, hypoxemia.
- CXR shows opacification and volume loss.
- Prevention/Treatment: Incentive spirometry, deep breathing exercises, and early mobilization.
⭐ On physical exam, look for tracheal deviation towards the side of collapse, a key distinguishing feature.
📌 Mnemonic (Post-Op Fever): "Wind" (atelectasis) is the primary cause on days 1-2.
Pneumonia - Unwanted Lung Guests
- Pathophysiology: Post-op atelectasis impairs secretion clearance, leading to bacterial growth. Aspiration is a key mechanism.
- Timeline: Typically develops >48 hours after surgery (Hospital-Acquired Pneumonia - HAP).
- Risk Factors: Ventilation >48h, age >65, COPD, smoking, thoracic/abdominal surgery.
- Diagnosis:
- New infiltrate on chest X-ray.
- Fever, leukocytosis, purulent sputum, ↓ O₂ sat.
- Prevention:
- Pre-op: Smoking cessation.
- Post-op: Early mobilization, incentive spirometry, good analgesia.
- Management: Empiric antibiotics covering gram-negatives (Pseudomonas) & S. aureus.
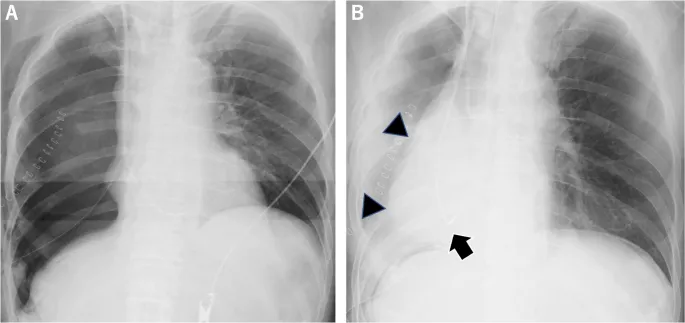
⭐ High-Yield: Ventilator-Associated Pneumonia (VAP) is a subtype of HAP developing >48 hours after endotracheal intubation. Key prevention includes semi-recumbent positioning and oral hygiene.
Aspiration & ARDS - The Domino Effect
-
Aspiration: Inhalation of gastric contents into lungs, a common trigger for severe pulmonary complications.
- Risk Factors: Anesthesia, opioids, GERD, NG tube, emergency surgery.
- Manifests as:
- Pneumonitis: Chemical injury from gastric acid. Rapid onset (hours) of dyspnea, hypoxia, low-grade fever.
- Pneumonia: Bacterial infection. Slower onset (days), productive cough, consolidation.
-
ARDS Progression: Aspiration is a primary cause of ARDS.
- Hallmarks: Refractory hypoxemia and bilateral pulmonary infiltrates on CXR, not due to heart failure.
- Key Metric: PaO₂/FiO₂ ratio <300 mmHg.
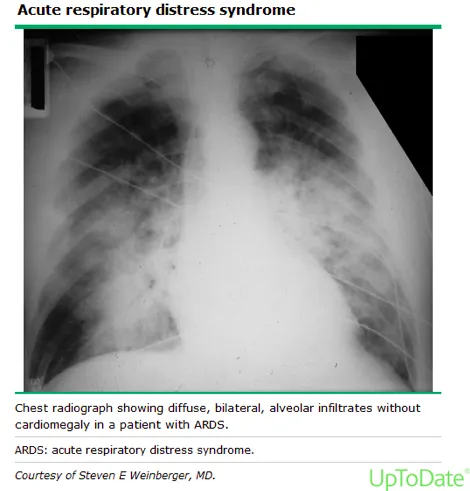
⭐ High-Yield: The cornerstone of ARDS management is lung-protective ventilation with low tidal volumes (~6 mL/kg ideal body weight) to prevent barotrauma, which has been shown to decrease mortality.
Pulmonary Embolism - Clot on the Move
-
Pathophysiology: Rooted in Virchow's Triad: stasis (e.g., post-op immobilization), hypercoagulability (e.g., malignancy, OCPs), and endothelial injury (e.g., surgery, trauma). Most PEs arise from lower extremity DVTs.
-
Clinical Picture: Sudden-onset tachypnea, pleuritic chest pain, dyspnea, and tachycardia. Massive PE can present with syncope, hypotension, and right heart failure.
-
Diagnosis:
- Use Wells score to stratify risk.
- D-dimer is sensitive for ruling out PE in low-risk patients.
- CT Pulmonary Angiography (CTPA) is the definitive diagnostic standard.
-
Management:
- Anticoagulation is the mainstay (Heparin, LMWH, DOACs).
- For massive PE causing hemodynamic instability: thrombolysis or surgical embolectomy.
⭐ Exam Favorite: While often tested, the classic ECG finding of S1Q3T3 (deep S wave in lead I, Q wave in lead III, inverted T wave in lead III) has low sensitivity for PE.
High‑Yield Points - ⚡ Biggest Takeaways
- Atelectasis is the most common cause of post-op fever within 48 hours; prevent with incentive spirometry.
- Postoperative pneumonia typically presents 3-5 days later with productive cough and consolidation.
- Pulmonary embolism (PE) causes sudden-onset dyspnea and is a major cause of preventable death.
- Aspiration pneumonitis is a chemical lung injury from gastric contents, distinct from aspiration pneumonia.
- Major risks: smoking, COPD, obesity, and thoracic/upper abdominal surgery.
- Prevention is key: early ambulation, pain control, and deep breathing.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

