Etiology & Risk Factors - Leaky Pipes, Bad Blood
- Surgical ("Leaky Pipes"): Most common cause.
- Inadequate hemostasis during surgery.
- Slipped ligature or dislodged clot from a vessel.
- Injury to adjacent vessels or organ parenchyma.
- Coagulopathic ("Bad Blood"):
- Pre-existing: Hemophilia, von Willebrand disease, platelet disorders.
- Acquired: Anticoagulant/antiplatelet meds (e.g., Warfarin, DOACs), dilutional coagulopathy from massive transfusion, DIC, uremia, liver failure.
- Medical:
- Postoperative hypertension stressing anastomoses.
- Hypothermia, which impairs the coagulation cascade.
⭐ The most common cause of postoperative bleeding is a technical error, i.e., inadequate mechanical hemostasis, not a primary coagulopathy.
Clinical Presentation & Diagnosis - Spotting Red Flags
-
Bleeding Manifestations:
- Overt: Visible blood from drains, wounds, or chest tubes; hematemesis, melena.
- Concealed: Signs of hypovolemia without obvious loss. Think retroperitoneum, thorax, or pelvis. Presents with tachycardia, hypotension, oliguria.
-
Diagnostic Workflow:
- Vitals & Exam: Check for tachycardia (often earliest sign), hypotension, cool/clammy skin, and ↓ urine output (< 0.5 mL/kg/hr).
- Labs: Serial CBC (Hgb/Hct), PT/INR, aPTT, fibrinogen.
- Imaging: Bedside FAST scan for quick assessment; CT angiography is gold standard for localizing the bleed.
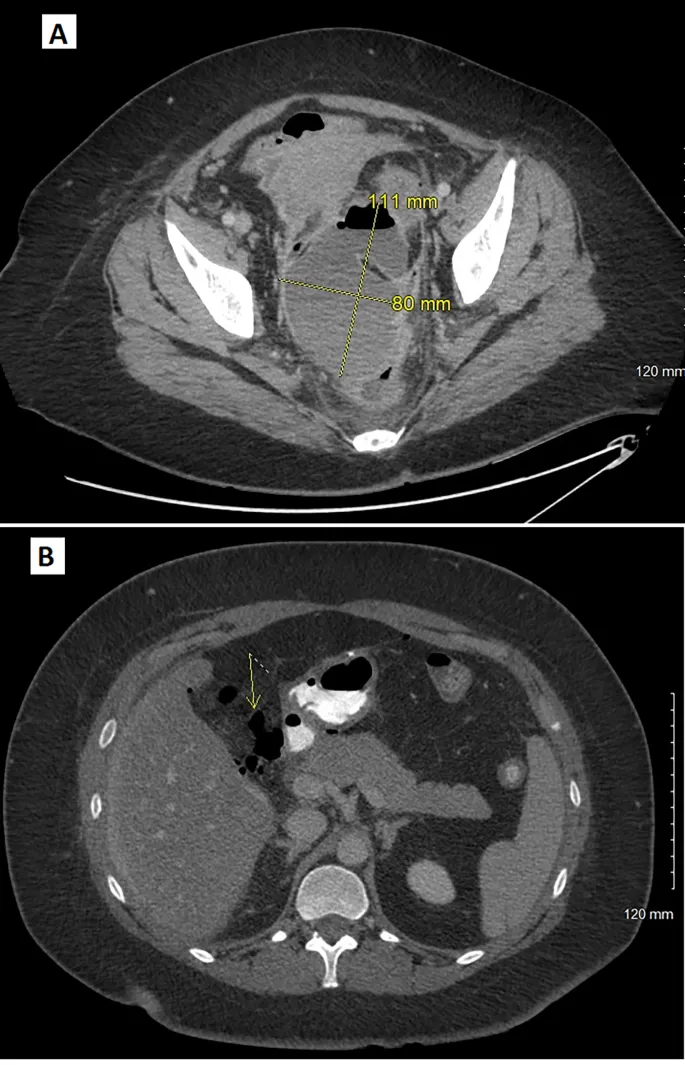
⭐ In acute hemorrhage, Hgb/Hct may be initially normal due to proportional loss of plasma and red cells. Serial measurements are key.
Management - Plugging the Dam
Initial stabilization is paramount. Follow resuscitation principles before targeting the source.
-
Initial Steps:
- Assess ABCs (Airway, Breathing, Circulation).
- Secure 2 large-bore IV lines.
- Begin aggressive fluid resuscitation with crystalloids (e.g., Normal Saline, Lactated Ringer's).
-
Transfusion Strategy:
- Administer blood products for hemodynamic instability or significant hemoglobin drop.
- Activate Massive Transfusion Protocol (MTP) for severe hemorrhage, targeting a ratio of $1:1:1$ (pRBCs:FFP:Platelets).
⭐ The Lethal Triad: Be vigilant for the deadly combination of acidosis, hypothermia, and coagulopathy in massive hemorrhage. Each component worsens the others, creating a vicious cycle.
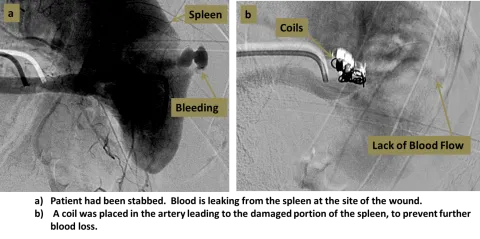
Complications & Special Cases - The Vicious Cycle
Uncontrolled bleeding progresses to hemorrhagic shock, a primary complication classified by severity.
| Class | Blood Loss | Heart Rate (bpm) | Blood Pressure | Mental Status |
|---|---|---|---|---|
| I | <15% | <100 | Normal | Normal |
| II | 15-30% | 100-120 | Normal / Orthostatic | Anxious |
| III | 30-40% | 120-140 | Hypotensive | Confused |
| IV | >40% | >140 | Profound ↓ | Lethargic |
- ⚠️ The Lethal Triad: A self-perpetuating cycle where hemorrhage causes:
- Hypothermia: Impairs clotting factor enzymatic activity.
- Acidosis: Reduces enzyme efficiency in the coagulation cascade.
- Coagulopathy: Worsens bleeding, completing the cycle.
- High-Risk Surgeries: Cardiac (especially on bypass), liver resections, major vascular surgery.
⭐ In massive transfusions, citrate in blood products chelates calcium, causing iatrogenic hypocalcemia. This is a critical, reversible driver of coagulopathy.
- Postoperative bleeding within 24 hours is most often due to technical error (e.g., a slipped ligature).
- Tachycardia is the earliest sign, often preceding hypotension and oliguria.
- A falling hematocrit is a key lab finding but may lag by several hours after acute blood loss.
- Delayed bleeding suggests erosion into a vessel or an underlying coagulopathy.
- Management is aggressive fluid resuscitation and prompt surgical re-exploration for significant, uncontrolled bleeding.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

