Perioperative CVA - Brain Attack on Deck
Perioperative stroke: a neurological deficit of vascular cause, occurring within 30 days of surgery. Primarily ischemic (~80%) due to embolism or hypoperfusion.
- Risk Factors: Advanced age (>65), prior CVA/TIA, cardiac surgery (esp. CABG), carotid stenosis, atrial fibrillation, intraoperative hypotension.
| Feature | Ischemic CVA | Hemorrhagic CVA |
|---|---|---|
| Pathophysiology | Embolus, thrombus, watershed infarct | Vessel rupture, often from HTN |
| Key Feature | Focal deficit, often follows embolization | ↑ICP signs (headache, vomiting) |
⭐ > Highest risk is in cardiac surgery involving cardiopulmonary bypass due to aortic manipulation and potential for air/atheromatous emboli.
Post-Op Delirium & POCD - Confusion in the Wards
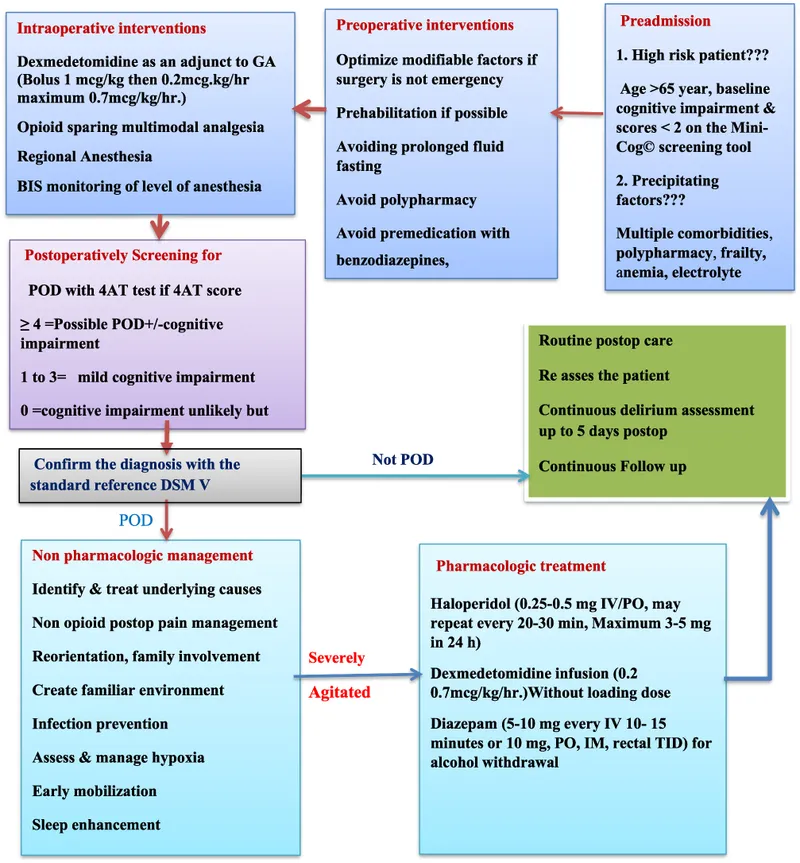
- Post-Op Delirium: An acute, fluctuating disturbance in attention, awareness, and cognition. It's a common complication, especially in elderly patients.
- POCD (Postoperative Cognitive Dysfunction): A more subtle and persistent decline in memory and concentration after anesthesia, lasting weeks to months.
- Risk Factors: Advanced age (>65), pre-existing dementia/cognitive impairment, major surgery (cardiac, orthopedic), polypharmacy.
- Precipitants: Infection (UTI, pneumonia), hypoxia, electrolyte disturbances, pain, and medications (e.g., benzodiazepines, anticholinergics).
⭐ High-Yield: The Confusion Assessment Method (CAM) is a key diagnostic tool, requiring features 1 (acute onset/fluctuating course) AND 2 (inattention), plus EITHER 3 (disorganized thinking) OR 4 (altered level of consciousness).
Post-Op Seizures - The Brain's Short Circuit
- Etiologies: Metabolic disturbances (hyponatremia, hypoglycemia, hypocalcemia), hypoxia, drug toxicity (e.g., local anesthetics, meperidine), alcohol/benzodiazepine withdrawal, or underlying epilepsy.
- Immediate Management:
⭐ Exam Favorite: Suspect acute hyponatremia as a cause in post-TURP or hysteroscopy patients due to absorption of hypotonic irrigation fluids.
Peripheral Nerve Injuries - Nerves Under Pressure
- Most are traction or compression neuropathies from poor positioning.
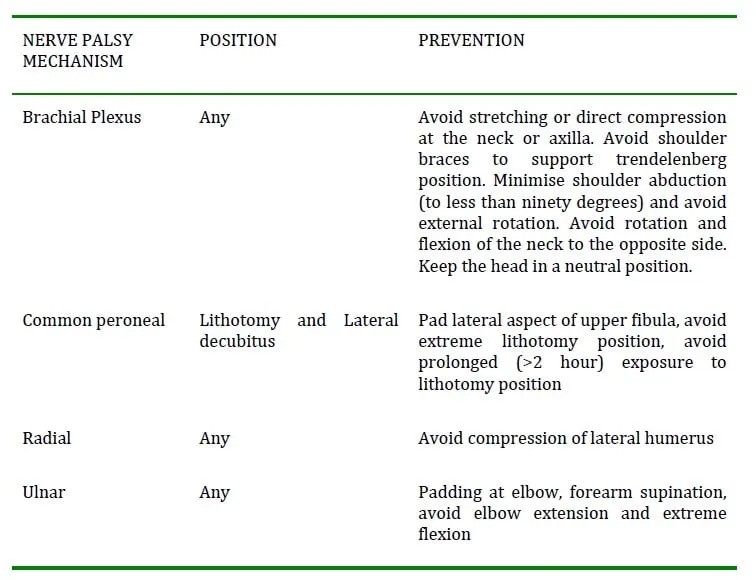
| Nerve | Mechanism of Injury | Presentation |
|---|---|---|
| Ulnar | Pressure on medial elbow (supine) | Claw hand (4th/5th digits), ↓ sensation |
| Radial | Arm over screen, compression in axilla | Wrist drop, ↓ grip strength |
| Common Peroneal | Stirrups, lateral knee pressure | Foot drop, ↓ dorsiflexion/eversion |
| Brachial Plexus | Arm abduction >90°, shoulder braces | Varies; arm/hand weakness/numbness |
📌 PED: Peroneal Everts & Dorsiflexes.
High-Yield Points - ⚡ Biggest Takeaways
- Central Pontine Myelinolysis results from rapid hyponatremia correction, causing spastic quadriplegia and pseudobulbar palsy.
- Postoperative delirium is common in the elderly; rule out reversible causes like hypoxia, infection, and medications.
- Perioperative stroke risk is increased by atrial fibrillation, carotid disease, and intraoperative hypotension.
- Post-op seizures can be triggered by metabolic disturbances, hypoxia, or substance withdrawal.
- Peripheral nerve injuries are usually due to improper positioning, affecting the brachial plexus or common peroneal nerve.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

