Anastomotic Leak - When Stitches Go Rogue
Breakdown of a surgical anastomosis, a major cause of post-op morbidity/mortality.
- Presentation: Typically post-op day 5-7.
- Fever, tachycardia, abdominal pain, ileus.
- Peritonitis if free intra-abdominal leak.
- Wound drainage may show purulent or enteric contents.
- Risk Factors: Tension on anastomosis, poor blood supply, malnutrition (Albumin <3 g/dL), steroids, smoking, obesity, radiation.
- Diagnosis:
- Labs: ↑WBC, ↑CRP.
- Imaging: CT with oral/rectal contrast is the gold standard.
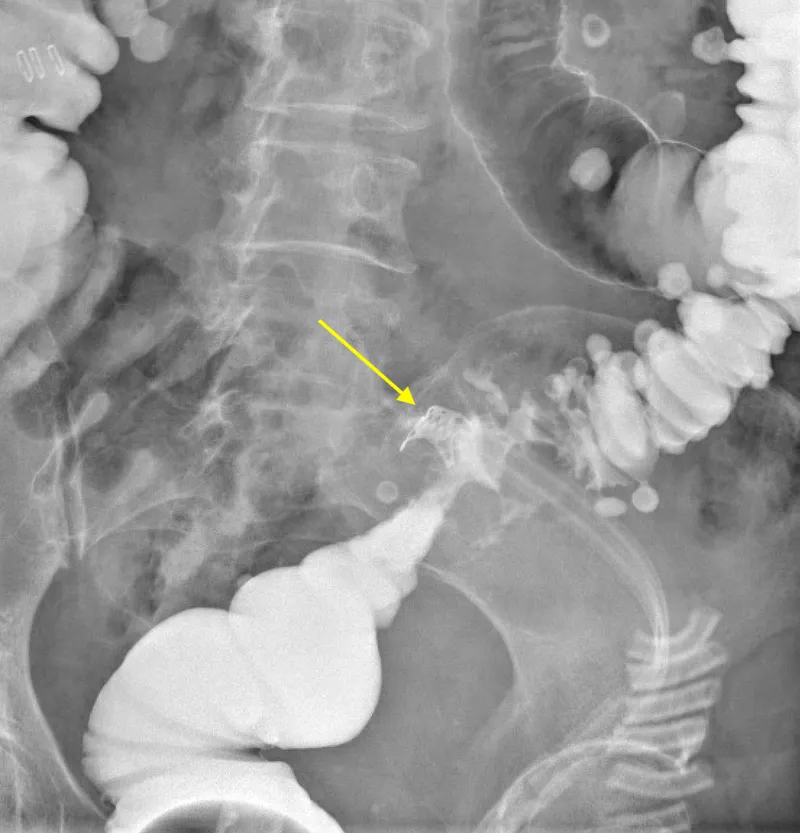
⭐ High-Yield: The most common presentation is unexplained tachycardia and fever around post-operative day 5-7. Maintain a high index of suspicion.
- Management:
Clinical Picture - Spotting the Seepage
- Onset: Typically post-op days 5-7.
- Systemic Signs (SIRS):
- Fever (>38°C), persistent tachycardia (>90 bpm), hypotension.
- Local Signs:
- New or worsening abdominal pain & tenderness.
- Peritonitis: guarding, rebound tenderness.
- Prolonged ileus.
- Wound/Drain Output:
- Change in character: serosanguinous → purulent, bilious, or feculent.
- Unexpectedly high drain output.
- Labs: ↑ WBC (leukocytosis), ↑ CRP.
⭐ Unexplained, persistent tachycardia is often the earliest sign of an anastomotic leak.
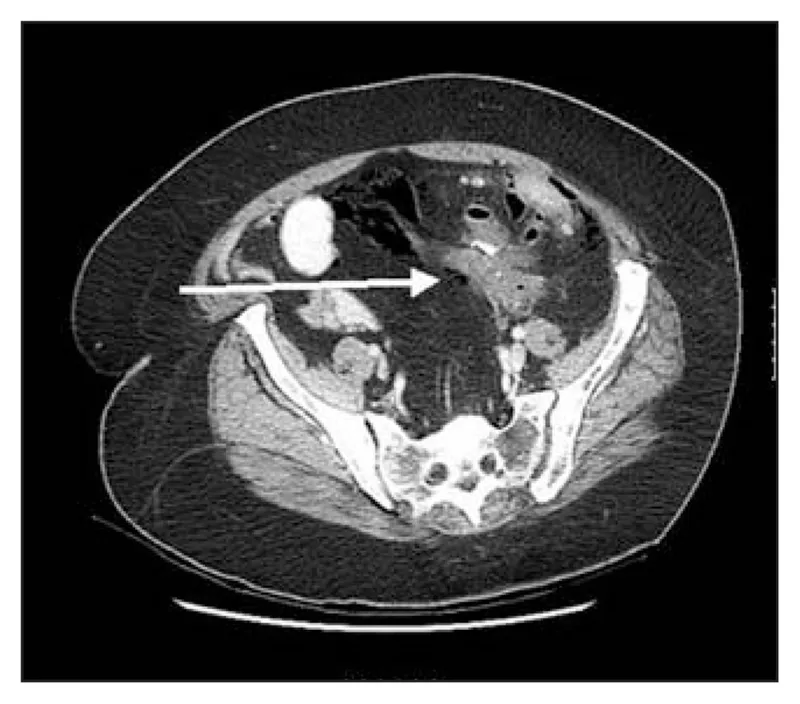
Diagnostic Workup - Confirming the Breach
-
Lab Markers:
- ↑ C-reactive protein (CRP) is the most sensitive early marker.
- Leukocytosis, acidosis, and electrolyte shifts are common but non-specific.
-
Imaging Gold Standard:
- CT Scan (Abdomen/Pelvis) with Contrast:
- IV contrast: Identifies abscesses, inflammation, and perfusion defects.
- Oral or Rectal contrast: (Water-soluble, e.g., Gastrografin) Directly visualizes contrast extravasation from the lumen.
- CT Scan (Abdomen/Pelvis) with Contrast:
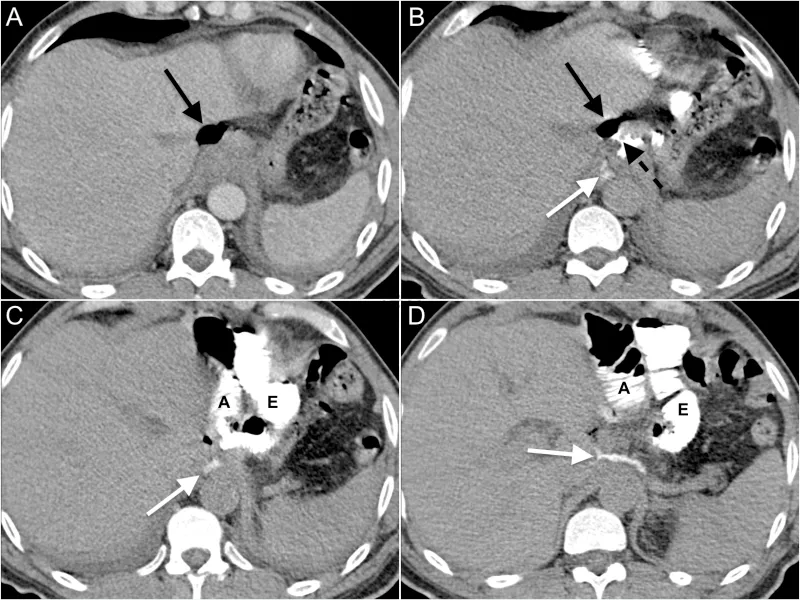
⭐ CRP Trajectory is Key: A single CRP value is less informative than the trend. A failure of CRP to fall by post-operative day 3, or a secondary rise, is highly predictive of a leak, often preceding clinical signs.
Leaky Gut Fix - Damage Control
Initial management focuses on resuscitation and source control. Stabilize the patient (ABCs), administer broad-spectrum IV antibiotics, and confirm with a CT scan (oral/rectal contrast).
- Management hinges on patient stability & leak containment.
- Conservative approach: For stable patients with small, contained leaks.
- Operative approach: For unstable patients or those with diffuse peritonitis. The goal is source control, not necessarily immediate definitive repair.
⭐ Most anastomotic leaks present on post-operative days 5-7. Fever, tachycardia, and abdominal pain are the classic triad.
High‑Yield Points - ⚡ Biggest Takeaways
- Anastomotic leak is a major cause of post-op morbidity, typically presenting on days 5-7 with fever, tachycardia, and abdominal pain.
- Key risk factors include malnutrition, smoking, steroid use, and tension on the anastomosis.
- CT scan with oral or rectal contrast is the diagnostic gold standard, showing fluid collections or contrast extravasation.
- Management is dictated by stability: unstable patients require emergent laparotomy; stable patients may be managed non-operatively.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

