Phases of Healing - The Repair Crew
⭐ Collagen Cross-Talk: The transition from pliable Type III collagen (granulation tissue) to strong Type I collagen is critical for wound strength. Deficiencies in this process (e.g., vitamin C, copper) lead to poor healing and dehiscence.
Wound Classification - Sorting the Damage
- Class I (Clean):
- Uninfected, no inflammation; tracts not entered.
- Examples: Hernia repair, breast biopsy.
- SSI Risk: <2%.
- Class II (Clean-Contaminated):
- Respiratory, GI, or GU tracts entered under controlled conditions.
- Examples: Elective cholecystectomy, lung resection.
- SSI Risk: 3-5%.
- Class III (Contaminated):
- Open, fresh accidental wounds or major sterile break (e.g., GI spillage).
- Examples: Penetrating trauma, inflamed appendectomy.
- SSI Risk: 5-15%.
- Class IV (Dirty/Infected):
- Existing clinical infection (pus) or perforated viscera.
- Examples: Abscess I&D, perforated diverticulitis.
- SSI Risk: >15% (up to 40%).
⭐ This classification is a key predictor of Surgical Site Infection (SSI) risk and directly guides the use of prophylactic antibiotics.
Wound Management - The Clean-Up Job
- Goal: Create a clean, moist, and protected environment for healing.
- Initial Steps: Hemostasis, irrigation (isotonic saline), and assessment.
- Debridement: Removal of necrotic/foreign material.
- Autolytic: Uses body's own enzymes (e.g., hydrocolloids).
- Enzymatic: Topical collagenase.
- Mechanical: Wet-to-dry dressings, irrigation.
- Surgical: Sharp debridement for extensive necrosis.
⭐ Exam Favorite: Wet-to-dry dressings are a form of mechanical debridement but are non-selective, potentially removing healthy granulation tissue upon removal and causing pain.
Healing Factors & Complications - When Things Go Wrong
- Systemic Factors Impairing Healing:
- Nutrition: Deficiencies in Protein, Vitamin C, Zinc.
- Comorbidities: Diabetes (↓ leukocyte function), PVD (ischemia).
- Lifestyle: Smoking (vasoconstriction, ↓ O₂), chronic alcohol use.
- Medications: Corticosteroids, chemotherapy, radiation.
- Local Factors:
- Infection: Most common cause of delayed healing.
- Poor Perfusion/Hypoxia: Inadequate blood supply.
- Technique: Excessive suture tension, tissue trauma.
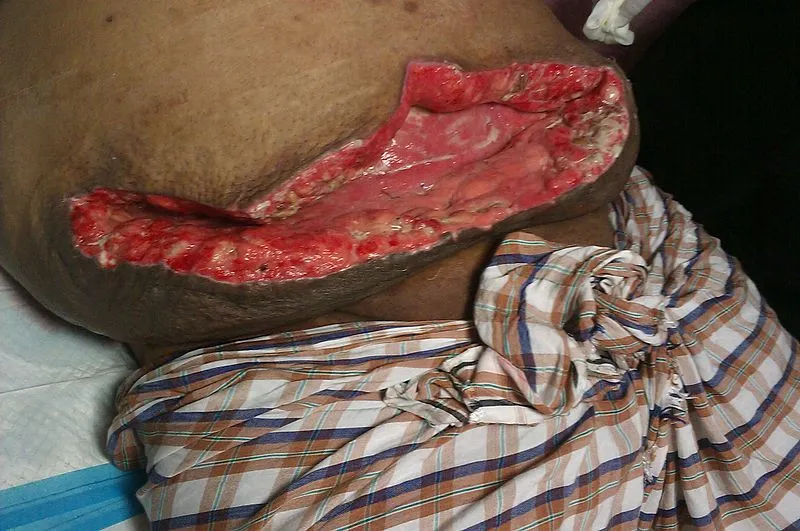
- Specific Complications:
- Dehiscence: Fascial separation.
- Evisceration: Organ protrusion (surgical emergency).
- Hypertrophic Scar: Collagen confined to wound boundaries.
- Keloid: Collagen extends beyond wound; common in darker skin tones.
⭐ A sudden gush of serosanguinous or "salmon-colored" fluid from an incision 5-8 days post-op is a classic sign of impending fascial dehiscence.
High-Yield Points - ⚡ Biggest Takeaways
- Primary intention sutures clean wounds; secondary intention leaves contaminated wounds open to granulate.
- Wound dehiscence (fascial separation) is a surgical emergency, often preceded by serosanguinous drainage.
- Staph aureus is the most common pathogen in post-op wound infections.
- Keep initial surgical dressings clean and dry for 24-48 hours.
- Healing requires adequate protein, vitamin C, and zinc.
- Evisceration (organ protrusion) requires immediate OR with sterile saline-soaked dressings.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

