Transition of Care - The Great Escape Plan
- Goal: Ensure a safe, seamless, and coordinated handover to the next care setting (e.g., PCP, skilled nursing facility, home health) to prevent complications and readmissions.
- Core Components:
- Medication Reconciliation: Meticulously compare pre-admission, in-hospital, and new discharge medications. This is the highest-yield step to prevent adverse drug events.
- Patient/Family Education: Use the "teach-back" method to confirm understanding of diet, activity, wound care, and red-flag symptoms (e.g., fever, ↑pain).
- Follow-up: Schedule specific follow-up appointments before the patient leaves the hospital.
⭐ High-Yield Fact: Inadequate care transitions are a primary driver of hospital readmissions, with nearly 20% of Medicare patients being readmitted within 30 days.
Discharge Components - The Handover Playbook
📌 Mnemonic: IDEAL Discharge
- Include the patient & family in discharge planning.
- Discuss key areas:
- Medication reconciliation (purpose, dose, frequency).
- Warning signs & symptoms requiring action.
- Diet and activity restrictions.
- Educate on the condition & management plan in plain language.
- Assess understanding using the "teach-back" method.
- Listen to and address all questions and concerns.
⭐ High-Yield Fact: Poor handovers are a leading cause of preventable readmissions. The "teach-back" method is crucial, as patients immediately forget 40-80% of medical information.
High-Risk Patients - Spotting the Vulnerable
- Core Principle: Proactively identify patients at high risk for adverse post-discharge outcomes (readmission, ED visits, medication errors).
- Key Risk Domains:
- Clinical: Multiple comorbidities (CHF, COPD, DM), polypharmacy (>5 meds), prior hospitalizations.
- Functional: Impaired ADLs/IADLs, cognitive decline, poor health literacy.
- Socio-demographic: Advanced age (>80), lack of social support, low socioeconomic status.
⭐ The LACE Index is a key tool predicting 30-day readmission or death. It assesses: Length of stay, Acuity of admission, Charlson Comorbidity Index, and Emergency department visits in the last 6 months. A score >10 indicates high risk.
Handoff Communication - Closing the Loop
- Goal: Ensure seamless, safe transfer of patient care responsibility, preventing medical errors during transitions.
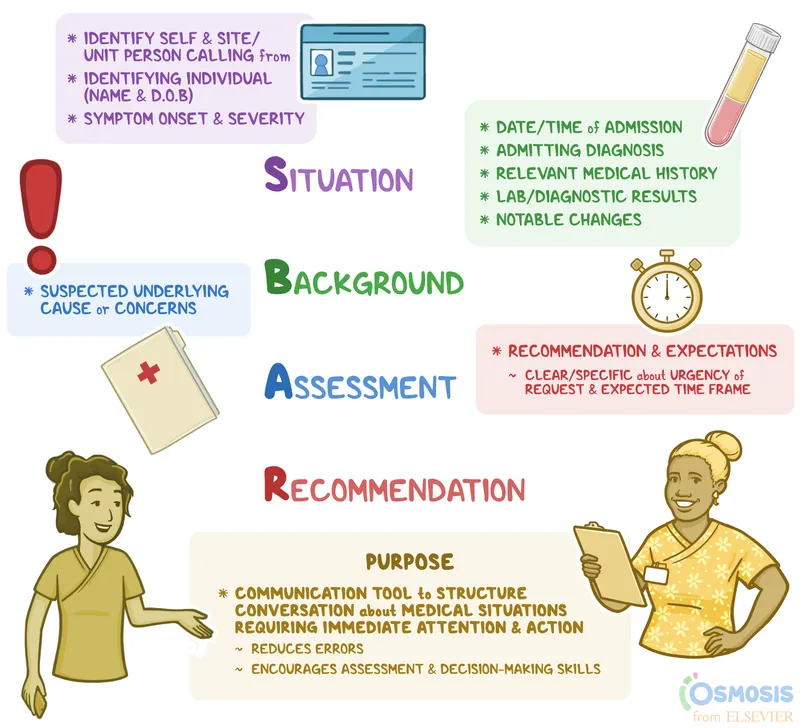
- Framework: Use standardized methods. 📌 SBAR is a high-yield, structured model for clear communication.
- Situation: Patient identity, location, and primary concern.
- Background: Procedure performed, relevant PMH, allergies, code status.
- Assessment: Current vitals, stability, potential risks (e.g., bleeding, infection).
- Recommendation: Explicit care plan, pending tasks, and "if-then" contingency instructions.
- Closing the Loop: The receiving provider verbally repeats back critical information to confirm understanding. The sender then verifies the accuracy of this read-back.
⭐ The Joint Commission reports that communication failures are a root cause in over 70% of sentinel events, making effective handoffs a top patient safety priority.
High-Yield Points - ⚡ Biggest Takeaways
- Early, proactive discharge planning, ideally initiated pre-operatively, is crucial for reducing readmissions.
- A multidisciplinary team (physicians, nurses, social workers, therapists) is central to effective care transition.
- Patient and family education on medications, diet, activity restrictions, and warning signs is paramount.
- Medication reconciliation at discharge is a critical step to prevent adverse drug events.
- Ensure a safe home environment and arrange for necessary durable medical equipment (DME) before discharge.
- Provide clear, written discharge summaries and schedule follow-up appointments prior to the patient leaving.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

