Pain Assessment - Gauging the Hurt
- Core Principle: Pain is subjective, the "fifth vital sign." Patient's report is key.
- 📌 PQRST Mnemonic: Provocation/Palliation, Quality, Radiation, Severity, Time.
- Pain Scales: Standardize severity assessment.
- Numeric Rating Scale (NRS): 0-10 scale, most common.
- Visual Analog Scale (VAS): 100mm line from "no pain" to "worst pain."
- Faces Pain Scale-Revised (FPS-R): For children or cognitive impairment.
- FLACC Scale: For non-verbal patients (Face, Legs, Activity, Cry, Consolability).
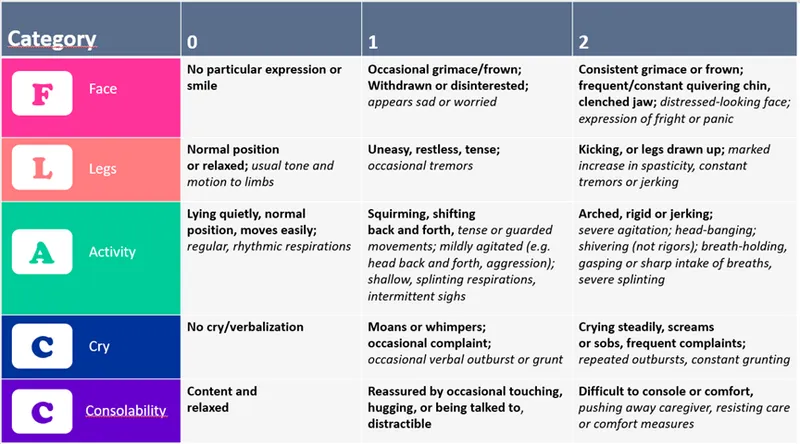
⭐ Patient self-report is the gold standard for pain assessment, more reliable than physiologic signs (e.g., tachycardia, hypertension), which can be non-specific.
Analgesic Arsenal - The Drug Cabinet
- Non-opioids: Foundation of multimodal analgesia.
- Acetaminophen: Central action. Max dose 4g/day. Risk of hepatotoxicity.
- NSAIDs (e.g., Ibuprofen, Ketorolac): Inhibit COX enzymes. ⚠️ Risk of GI bleeds & renal injury.
- Opioids: For moderate-to-severe pain; use lowest effective dose.
- Agonists: Morphine, hydromorphone, fentanyl.
- Delivery: Patient-Controlled Analgesia (PCA) common.
- Side Effects: ⚠️ Respiratory depression, sedation, constipation.
- Local Anesthetics:
- Bupivacaine, Ropivacaine for epidurals & nerve blocks.
- Adjuvant Analgesics:
- Gabapentinoids for neuropathic pain.
- Low-dose Ketamine as an NMDA antagonist.
⭐ Ketorolac (an NSAID) use is limited to ≤5 days due to significant renal and GI toxicity risk.
Delivery Modalities - Smart Systems
-
Patient-Controlled Analgesia (PCA)
- Patient self-administers small, pre-set opioid doses (e.g., morphine, hydromorphone).
- Components: On-demand bolus, a lockout interval (5-10 min) to prevent overdose, and an optional basal infusion.
- Benefit: Empowers patients, leading to better pain control and potentially lower total opioid consumption.
- 📌 Mnemonic: PCA for Patient Controls Administration.
-
Epidural Analgesia
- Catheter in epidural space delivers local anesthetic + opioid (e.g., bupivacaine + fentanyl).
- Superior pain control for major abdominal/thoracic surgery.
⭐ High-Yield: Epidurals can cause sympathetic blockade, leading to hypotension and bradycardia. Monitor vitals closely.
-
Continuous Peripheral Nerve Blocks
- Catheter placed near a specific nerve/plexus (e.g., femoral, brachial).
- Infuses local anesthetic for targeted, prolonged analgesia.

Opioid Side Effects - Handling Hazards
- Respiratory Depression: Most severe risk. Monitor RR; if <12/min, consider intervention.
- Constipation: Universal side effect. Begin prophylaxis with stimulant + softener (e.g., Senna + Docusate). 📌 "Mush and Push."
- Nausea & Vomiting: Common. Treat with antiemetics like ondansetron.
- Pruritus: Especially with neuraxial opioids. Manage with antihistamines or low-dose naloxone.
- Sedation: Dose-dependent. Reduce dose or consider opioid rotation.
⭐ Naloxone's half-life (60-90 min) is shorter than most opioids. Patients can re-sedate after naloxone wears off, necessitating vigilant monitoring and potential redosing.
High‑Yield Points - ⚡ Biggest Takeaways
- Multimodal analgesia is the standard, using non-opioid analgesics (NSAIDs, acetaminophen) and regional techniques to reduce opioid requirements.
- The most feared opioid side effect is respiratory depression. Also monitor for sedation, nausea, and postoperative ileus.
- Patient-Controlled Analgesia (PCA) is effective but carries overdose risk, especially with continuous basal rates in opioid-naïve patients.
- Epidural analgesia offers superior pain control for major thoracoabdominal surgery but risks hypotension (sympathectomy) and epidural hematoma.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

