Nutritional Assessment - Sizing Up The Patient
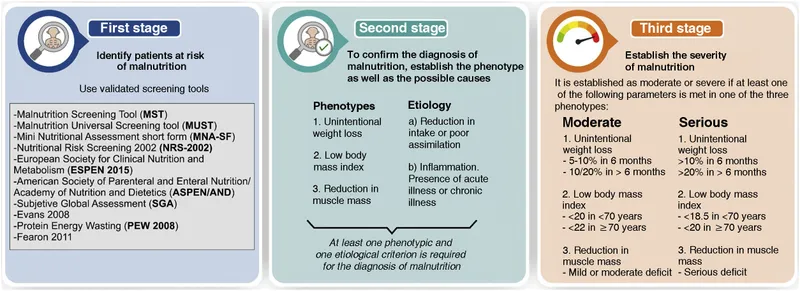
- Screening Tools: Identify at-risk patients using:
- Nutritional Risk Screening (NRS-2002): Score ≥ 3 indicates high risk.
- Malnutrition Universal Screening Tool (MUST).
- Key Markers:
- Prealbumin (PAB): Most sensitive indicator for acute nutritional changes (2-day half-life).
- Albumin: Marker for chronic malnutrition (20-day half-life); < 3.0 g/dL is significant.
- BMI: $BMI = kg/m^2$.
⭐ Prealbumin's short half-life (~2 days) makes it a superior marker for acute changes in nutritional status compared to albumin (~20 days).
Indications & Timing - The When and Why
-
Indications for Nutritional Support:
- Inadequate oral intake anticipated for > 7-10 days.
- Severe malnutrition (e.g., albumin < 3.0 g/dL, weight loss > 10-15%).
- Hypercatabolic states: major trauma, severe sepsis, burns.
-
Timing: Early initiation is key. Prefer enteral routes if the gut is functional.
⭐ In moderately malnourished patients, delaying surgery for 7-10 days to provide preoperative nutritional support can reduce postoperative complications.
Enteral vs. Parenteral - Gut Instincts
📌 Mnemonic: 'If the gut works, use it!'
Prioritize Enteral Nutrition (EN) whenever the GI tract is functional, even if trophic ('trickle') feeds are all that is tolerated.
-
Enteral Nutrition (EN): "Tube Feeds"
- Route: Nasogastric, PEG, or jejunostomy tube.
- Benefits: Maintains gut integrity, ↓ infection risk, ↓ bacterial translocation, cheaper.
- Contraindications: Mechanical bowel obstruction, ileus, hemodynamic instability (shock), intractable vomiting/diarrhea.
-
Parenteral Nutrition (PN): "IV Feeds"
- Indication: Non-functional or inaccessible GI tract for > 7 days.
- Types:
- Total (TPN): Central line. For long-term support.
- Peripheral (PPN): Peripheral IV. Short-term (< 2 weeks), lower calorie.
- Risks: Catheter-related bloodstream infection (CRBSI), hyperglycemia, electrolyte shifts, hepatic steatosis.
⭐ Enteral nutrition helps maintain gut mucosal integrity and reduces the risk of bacterial translocation compared to parenteral nutrition.
Complications & Monitoring - Navigating The Risks
- Refeeding Syndrome: Potentially fatal shift in fluids & electrolytes.
- ⚠️ Key findings: Severe ↓$PO₄³⁻$, ↓$K⁺$, ↓$Mg²⁺$, and vitamin (thiamine) deficiency.
- Occurs in chronically malnourished patients started on aggressive nutritional support.
⭐ The hallmark of refeeding syndrome is severe hypophosphatemia, which can lead to cardiac failure, rhabdomyolysis, and seizures.
-
Parenteral Nutrition (PN) Complications:
- Infectious: Central line-associated bloodstream infection (CLABSI).
- Metabolic: Hyperglycemia, hypertriglyceridemia.
- Hepatic: Cholestasis, steatosis (fatty liver).
-
Monitoring Schedule:
- Daily: Glucose, electrolytes (PO₄³⁻, K⁺, Mg²⁺).
- Weekly: Liver function tests (LFTs), triglycerides.
High‑Yield Points - ⚡ Biggest Takeaways
- Enteral nutrition (EN) is strongly preferred over parenteral nutrition (PN) to preserve gut mucosal integrity and prevent bacterial translocation.
- Initiate nutritional support if a patient is unlikely to resume oral intake within 5-7 days.
- Key risks of PN include central line infections (CLABSI), refeeding syndrome, and liver dysfunction.
- Refeeding syndrome is characterized by severe hypophosphatemia upon re-feeding a malnourished patient.
- Prealbumin is a more sensitive indicator of acute nutritional changes than albumin.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

