👶 Pathophysiology - Wrong Pipes, Big Trouble
-
Tracheoesophageal Fistula (TEF): Abnormal connection between trachea & esophagus.
-
Esophageal Atresia (EA): Esophagus ends in a blind pouch.
-
Embryology: Failure of the tracheoesophageal septum to separate the primitive foregut into trachea and esophagus during weeks 4-5 of gestation.
-
Gross Classification (Most Common Types):
- Type C (85%): EA with distal TEF.
- Type A (8%): Isolated EA (no fistula).
- Type E/H-type (4%): TEF without EA.
⭐ TEF/EA is a key component of the VACTERL association (Vertebral, Anal, Cardiac, Tracheo-Esophageal, Renal, Limb defects).
👶 Clinical Manifestations - The Newborn Bubble Test
- Classic Triad (The 3 C's):
- Choking
- Coughing
- Cyanosis, especially during the first feeding attempt.
- Key Observations:
- Excessive salivation, drooling, and frothy bubbles from the mouth.
- Respiratory distress from aspiration of saliva and/or gastric contents.
- Prenatal History:
- Often associated with maternal polyhydramnios due to impaired fetal swallowing of amniotic fluid.
- Associated Anomalies:
- 📌 VACTERL association is seen in ~50% of cases.
⭐ Inability to pass a nasogastric (NG) tube beyond 10-12 cm is a classic diagnostic sign; the tube coils in the blind esophageal pouch.
🔎 Diagnosis - Spot the Dead End
- Primary Step: Inability to pass a nasogastric (NG) tube into the stomach. The tube meets resistance and coils in the upper esophagus.
- Confirmation: A chest/abdominal X-ray is the key diagnostic imaging study.
- Shows: Coiled NG tube in the blind esophageal pouch.
- Differentiates: The pattern of bowel gas is critical for classification.
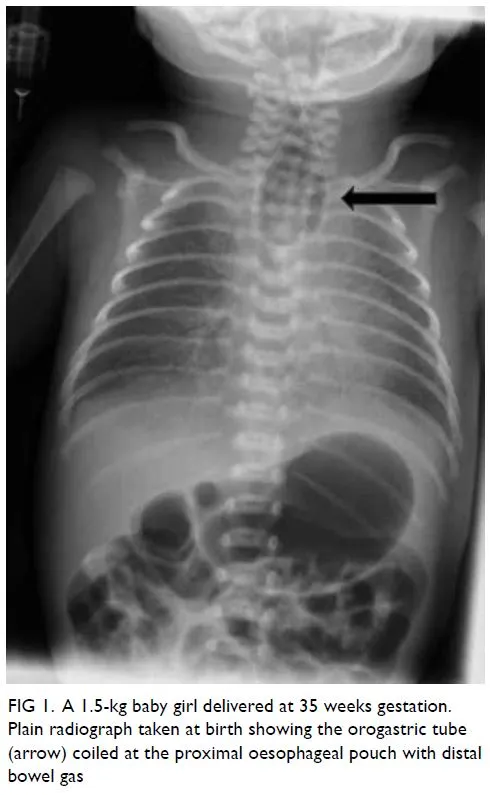
⭐ A gas-filled stomach confirms a patent distal fistula (Type C), the most common variant. A gasless abdomen indicates pure atresia (Type A) or a rare variant without a distal connection.
- Definitive Localization: Bronchoscopy may be used preoperatively to precisely locate the fistula.
✂️ Management - The Surgical Hook-Up
-
Initial Stabilization:
- NPO (Nil Per Os) to prevent aspiration.
- Elevate head of bed.
- Continuous suction of the blind upper esophageal pouch.
-
Pre-operative Workup:
- Crucial to rule out associated anomalies.
⭐ VACTERL Workup: Echocardiogram (cardiac), renal ultrasound, and vertebral X-rays are essential before surgery.
-
Surgical Repair:
- Definitive: Right-sided thoracotomy.
- Ligation of the fistula.
- Primary end-to-end anastomosis of esophageal segments.
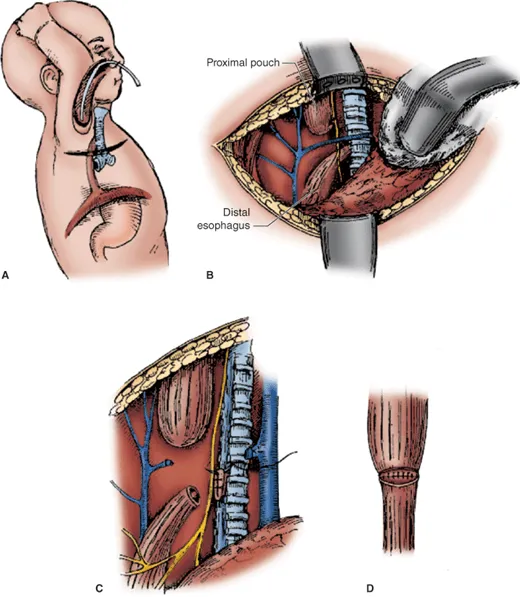
- Post-operative Care:
- Chest tube for drainage.
- Gastrostomy tube (G-tube) for initial feeding.
- Contrast esophagram around post-op day 5-7 to check for leaks.
⚠️ Complications - Post-Op Pitfalls
- Early (Days to Weeks)
- Anastomotic leak: Presents with sepsis, pneumothorax.
- Esophageal stricture: Dysphagia, may require dilation.
- Recurrent fistula: Choking, cyanosis with feeds.
- Late (Months to Years)
- Gastroesophageal reflux (GERD)
- Tracheomalacia: Barky cough, stridor.
- Esophageal dysmotility
⭐ GERD is the most frequent long-term complication, often requiring lifelong management.
⚡ Biggest Takeaways
- Most common type (C): Esophageal atresia with a distal TEF (~85%).
- Classic triad: Newborn with excessive secretions, choking/cyanosis with feeds, and respiratory distress.
- Diagnosis: Inability to pass an NG tube, which appears coiled on CXR. Air in the stomach confirms a distal fistula.
- Associated anomalies: Screen for VACTERL (Vertebral, Anal, Cardiac, TEF, Renal, Limb).
- Pre-op management: NPO, head elevation, and continuous suction of the blind esophageal pouch.
- Post-op complications: Anastomotic leak, esophageal stricture, and tracheomalacia.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

