🌬️ Telescoping Trouble
Management focuses on non-operative reduction in stable patients.
- Initial Steps: IV fluids, NG tube decompression, surgical consult.
- Non-operative Reduction:
- Air (pneumatic) enema is the preferred method.
- Success rate is high (80-95%).
- Surgical Intervention:
- Indicated for failed enema or signs of ischemia/perforation.
- Involves manual reduction ("milking") or bowel resection if non-viable.
⭐ Recurrence after successful enema reduction is ~10%. Most recurrences happen within 72 hours of the procedure.
🌭 Radiology - Signs of the Sausage
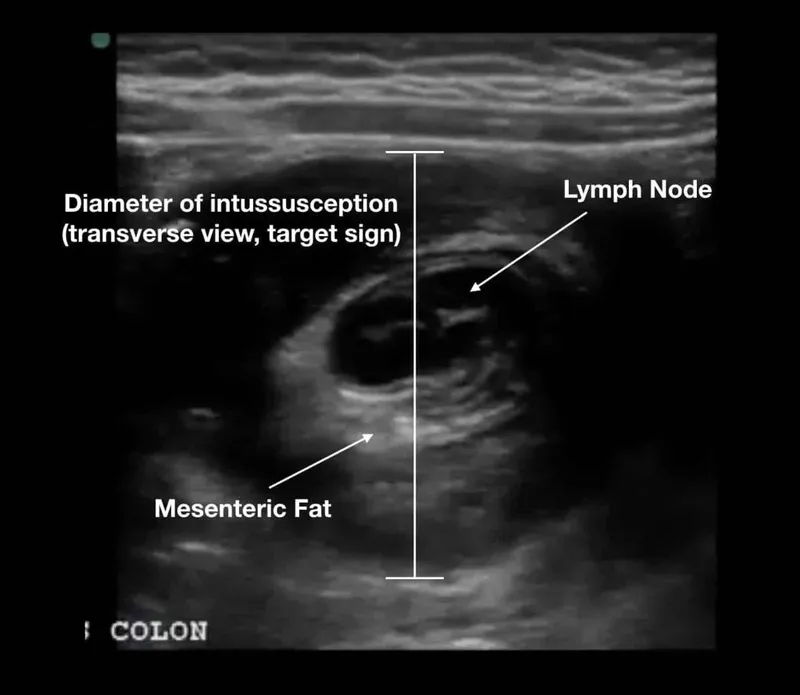
- Ultrasound (US): Gold standard diagnostic tool with >98% accuracy.
- Transverse view: Classic "target sign" or "donut sign" showing multiple concentric rings of bowel wall.
- Longitudinal view: "Pseudokidney sign" or "sandwich sign" representing the telescoped bowel.
- Abdominal X-ray (AXR): Often the initial test, but may be normal in ~25% of cases.
- Suggestive findings: Sausage-shaped mass, signs of SBO, and an empty RLQ (Dance's sign).
- Contrast/Air Enema: Confirmatory finding is the "crescent sign" where contrast fills the space between the intussusceptum and intussuscipiens.
⭐ The presence of free air (pneumoperitoneum) on imaging is an absolute contraindication to non-operative reduction.
🌬️ Management - The Great Unfolding
- Initial Steps: Stabilize first! IV fluids, NG tube decompression, and analgesia.
- Non-operative Reduction (First-Line): For stable patients without peritonitis.
- Air (Pneumatic) Enema: Preferred method. Higher success rate (~80-95%) and lower perforation risk compared to barium.
- Hydrostatic (Saline/Contrast) Enema: Alternative method.
- ⚠️ Contraindications: Peritonitis, perforation, shock.
- 💡 Max 3 attempts are typically made.
⭐ Recurrence after successful non-operative reduction occurs in ~5-10% of cases, usually within 24-48 hours. Observation is key.
- Surgical Intervention: Indicated for hemodynamic instability, peritonitis, perforation, or failed enema reduction.
- Procedure: Manual reduction ("milking" the bowel). Resection if bowel is gangrenous or a pathologic lead point is found.
⚠️ Complications - Perils of Pressure
- Bowel Perforation: Most feared complication of non-operative reduction.
- Cause: Excessive intraluminal pressure from air/contrast. Pressure should not exceed 120 mmHg.
- Signs: Sudden decompensation, fever, tachycardia, abdominal rigidity (peritonitis).
- Imaging: Free intraperitoneal air on X-ray or fluoroscopy.
- Management of Perforation:
- Immediate: Stop procedure, IV fluids, broad-spectrum antibiotics.
- Definitive: Emergent laparotomy for repair/resection.
⭐ Perforation risk is higher with symptoms > 48 hours, dehydration, and signs of peritonitis before the procedure.
⚡ High-Yield Points - Biggest Takeaways
- Non-operative reduction is the first-line treatment for stable patients without peritonitis.
- The preferred method is an air enema under fluoroscopic or ultrasound guidance; it has a lower perforation risk than barium.
- Absolute contraindications to enema are signs of perforation, peritonitis, or shock, which mandate immediate surgical exploration.
- Non-operative reduction is successful in >80% of cases, but recurrence can occur in 5-10%.
- Surgery is indicated for failed enemas or a suspected pathological lead point.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

