🔩 Core concept - Hip Hardware 101
- Total Hip Arthroplasty (THA) Components:
- Acetabular Cup: Replaces socket; typically titanium, porous-coated for bone ingrowth.
- Liner: Fits inside cup; common material is ultra-high-molecular-weight polyethylene (UHMWPE).
- Femoral Head: Replaces ball; usually ceramic or cobalt-chrome.
- Femoral Stem: Inserts into femur; titanium or cobalt-chrome alloy.
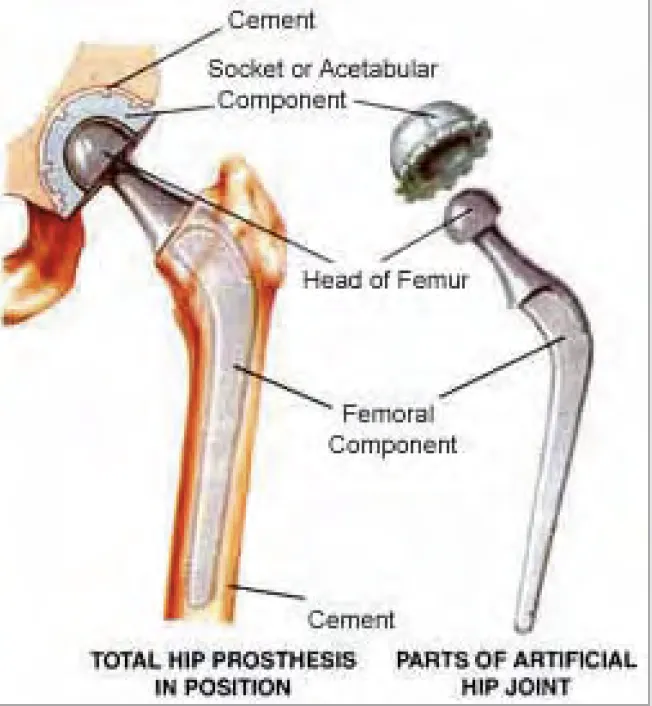
- Fixation Methods:
- Cementless (Press-fit): Relies on bone ingrowth; preferred in younger patients with good bone.
- Cemented (PMMA): For immediate fixation; used in older patients or poor bone quality.
⭐ Bearing Surfaces: The head-liner articulation is critical. Ceramic-on-polyethylene offers low wear rates, reducing the risk of periprosthetic osteolysis from wear debris-a major cause of long-term failure.
🤕 Clinical Manifestations - The Failing Hip
- Pain: Primary symptom, typically a dull, aching groin pain.
- May radiate to the buttock, anterior thigh, or knee.
- Worsens with activity and weight-bearing; can progress to rest/night pain.
- Stiffness & Functional Decline:
- ↓ range of motion, especially internal rotation.
- Difficulty with ADLs (e.g., putting on socks, tying shoes).
- Antalgic gait (limp) and reduced walking distance.
- Physical Exam:
- Pain with passive hip motion.
- Possible Trendelenburg sign (abductor weakness).
⭐ Pearl: Hip pathology often presents as isolated knee pain via the obturator nerve (L2-L4). Always examine the hip in patients with knee pain.
🔎 Diagnosis - Spotting the Damage
- History & Physical: Insidious-onset groin/thigh pain, morning stiffness < 30 minutes, pain worsened by activity. A key physical exam finding is decreased internal rotation of the hip.
- Imaging: Weight-bearing Anteroposterior (AP) Pelvis and lateral hip X-rays are the primary diagnostic tools.
⭐ Radiographic findings are paramount for diagnosis. 📌 Mnemonic: JSN-OSS (Joint Space Narrowing, Osteophytes, Subchondral Sclerosis, Subchondral Cysts).
🔩 Management - The Surgical Fix
- Total Hip Arthroplasty (THA): Replaces the damaged femoral head and acetabulum with prosthetic components.
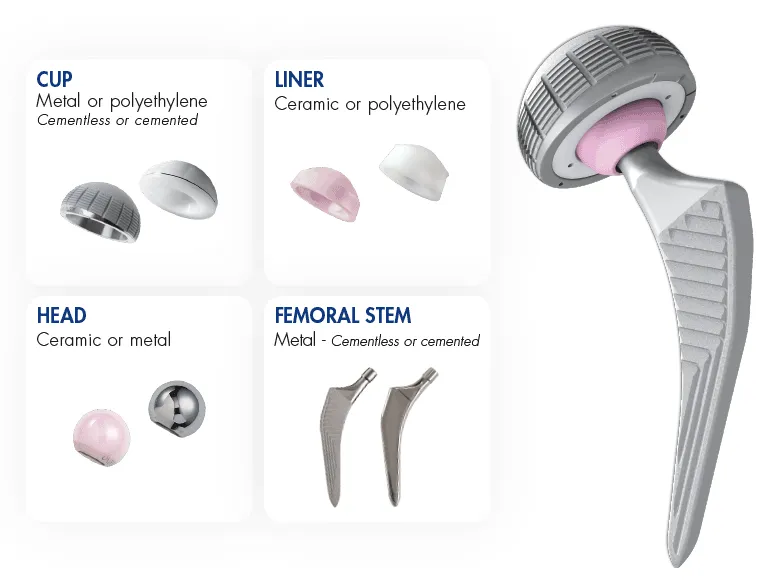
- Components & Fixation:
- Cementless: Press-fit for bone ingrowth; used in younger, active patients with good bone stock.
- Cemented: Uses bone cement for immediate fixation; common in older patients or those with osteoporosis.
- Bearing Surfaces:
- Metal-on-Polyethylene: Most common standard.
- Ceramic-on-Polyethylene/Ceramic: Lower wear rates, often for younger patients.
⭐ Posterior Approach: Most common surgical approach. Carries the highest risk of posterior hip dislocation and sciatic nerve injury. Post-op precautions include avoiding hip flexion >90°, adduction, and internal rotation.
⚠️ Complications - Post-Op Pitfalls
- Dislocation: Most common early complication.
- Posterior approach: ↑ risk. Presents as shortened, internally rotated leg.
- Anterior approach: ↓ risk.
- Infection:
- Acute (<3 mo): S. aureus, Strep.
- Chronic (>3 mo): S. epidermidis (biofilm).
- VTE (DVT/PE): Major cause of morbidity/mortality; requires prophylaxis.
- Nerve Injury: Sciatic (posterior approach), Femoral (anterior approach).
- Late Failure:
- Aseptic Loosening: Most common cause. Polyethylene wear debris → osteolysis.
- Periprosthetic fracture.
⭐ A patient with a recent posterior approach hip arthroplasty presenting with sudden hip pain, a shortened, and internally rotated limb likely has a prosthesis dislocation.
⚡ Biggest Takeaways
- Severe osteoarthritis is the leading indication for total hip arthroplasty (THA).
- The posterior surgical approach is most common but carries a higher risk of sciatic nerve injury and posterior dislocation.
- Hip dislocation is the most frequent early complication, presenting with a shortened, internally rotated leg.
- Aseptic loosening, caused by polyethylene wear debris, is the most common reason for late implant failure.
- Prosthetic joint infection is a devastating complication; suspect S. aureus early and S. epidermidis late.
- Venous thromboembolism (VTE) is a major risk requiring routine pharmacologic prophylaxis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

