🦴 Pathology & Classification - The Bone-Break Blueprint
A fracture is a break in the continuity of bone. Key descriptors include location, pattern, displacement, and skin integrity (open vs. closed).
-
Common Fracture Patterns:
-
Open Fractures (Gustilo-Anderson Classification): | Type | Wound Size | Injury Characteristics | | :--- | :--- | :--- | | I | < 1 cm | Clean, minimal soft tissue damage | | II | > 1 cm | Moderate soft tissue damage, no flap needed | | IIIA | > 10 cm | High energy, adequate soft tissue coverage | | IIIB | > 10 cm | Periosteal stripping, requires flap coverage | | IIIC | > 10 cm | Associated arterial injury requiring repair |* Pediatric Physeal Fractures (Salter-Harris):
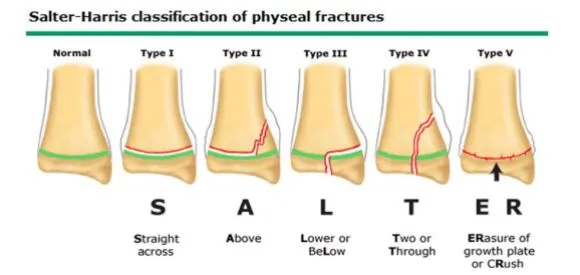 📌 SALTER Mnemonic: Straight, Above, Lower, Through, ERasure/cRush.
📌 SALTER Mnemonic: Straight, Above, Lower, Through, ERasure/cRush.
⭐ Salter-Harris Type II (fracture through physis and metaphysis) is the most common. Type V has the worst prognosis due to risk of growth arrest.
🦴 Radiology - Reading the Cracks
- Rule of Twos: A fundamental principle for adequate imaging.
- 2 Views: At least two orthogonal views (e.g., AP & Lateral at $90^\circ$).
- 2 Joints: Image the joint above and below the suspected fracture.
- 2 Sides: Compare with the contralateral side, especially in pediatrics.
- 2 Occasions: Repeat imaging if high clinical suspicion persists despite negative initial X-rays.
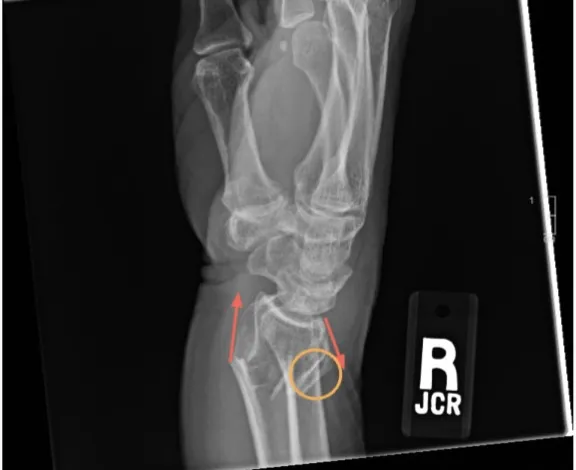
- Describing Fractures (The 4 A's):
- Alignment: Relationship of the longitudinal axes of fracture fragments.
- Angulation: Deviation of the distal fragment from the normal axis.
- Apposition: Percentage of fracture surface contact.
- Displacement: Shift of the distal fragment relative to the proximal.
⭐ A negative X-ray does not rule out a fracture. High-risk injuries (e.g., scaphoid, femoral neck) with negative initial films warrant further imaging (CT/MRI) or repeat X-rays in 7-14 days.
- Special Views: Often required for anatomically complex areas (e.g., scaphoid view, ankle mortise view).
🧩 Management - Putting Pieces Together
- Initial Fracture Management Flowchart:
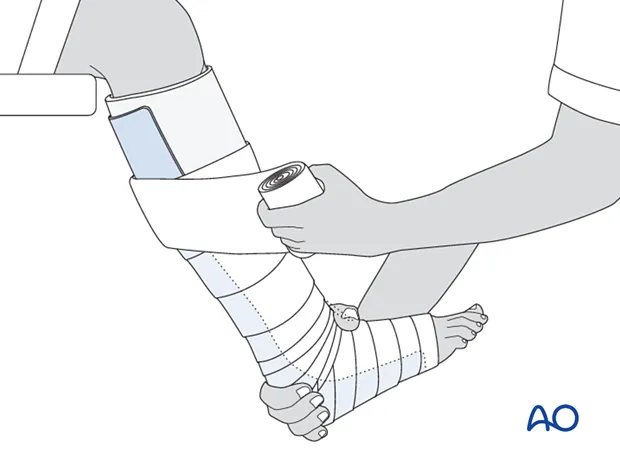
- Immobilization:
- Temporary (Acute): Splint - Accommodates swelling; non-circumferential.
- Definitive: Cast - Circumferential; applied after acute swelling subsides.
- Indications for ORIF (Open Reduction Internal Fixation):
- Open fractures
- Intra-articular displacement (>2 mm)
- Failed closed reduction / Unstable fractures
- Pathologic fractures
- Nonunion / Malunion
- Associated neurovascular injury
⭐ Compartment Syndrome: A surgical emergency! Suspect with pain out of proportion to injury, pain on passive stretch, and paresthesias. Pulselessness is a late sign.
🤕 Complications - When Healing Goes Wrong
| Early (Hours to Days) | Late (Weeks to Years) |
|---|---|
| * Neurovascular Injury: Direct damage | * Malunion: Heals in wrong position |
| * Compartment Syndrome: ↑ Pressure | * Nonunion: Fails to heal (>6-9 mo) |
| - 📌 6 P's: Pain, Pallor, Paresthesia, Pulselessness, Paralysis, Poikilothermia | * Delayed Union: Heals too slowly |
| - ⚠️ Dx: $\Delta P$ < 20-30 mmHg | * Avascular Necrosis (AVN) |
| * Fat Embolism: Triad (neuro, resp, petechiae) | * Post-traumatic Arthritis: Joint damage |
| * DVT/PE: Immobility risk | |
| * Infection: Open fx, surgery |
⚡ Biggest Takeaways
- Open fractures are surgical emergencies requiring immediate irrigation, debridement (I&D), and IV antibiotics.
- Always assess distal neurovascular status before and after reduction; any compromise is an emergency.
- Suspect compartment syndrome with pain out of proportion to injury; treat emergently with fasciotomy.
- Salter-Harris fractures involve the pediatric physis (growth plate); Type II is the most common.
- Management principles are Reduction (alignment), Immobilization (stabilization), and Rehabilitation.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

