💥 Pathophysiology - Anatomic Catastrophes
-
Obstruction: Tumor mass physically blocks a lumen.
- GI Tract: Malignant Bowel Obstruction (MBO) from colorectal, ovarian CA.
- Biliary Tree: Obstructive jaundice from pancreatic head CA, cholangiocarcinoma.
- Urinary Tract: Hydronephrosis from cervical, prostate, bladder CA.
- Airway: Stridor, dyspnea from lung, laryngeal, thyroid CA.
-
Perforation: Tumor necrosis or invasion through a hollow viscus wall.
- Leads to peritonitis, sepsis.
- Common in GI lymphomas, GISTs, advanced colorectal CA.
-
Hemorrhage: Tumor erosion into blood vessels or bleeding from friable tumor surface.
- Presents as acute bleed (e.g., hemoptysis) or chronic anemia.
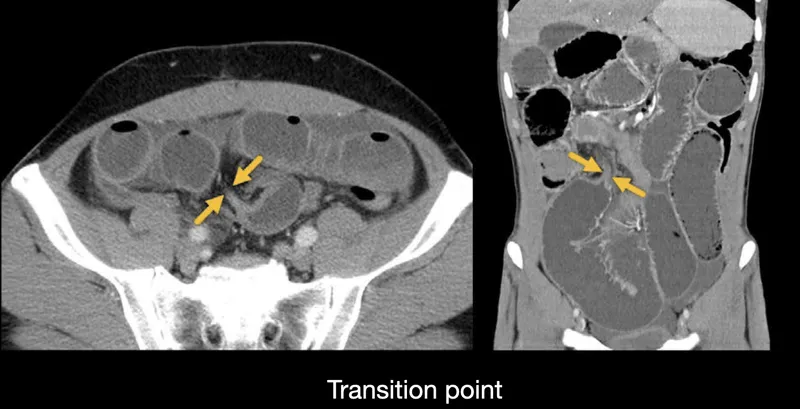
⭐ Ovarian cancer is a leading cause of malignant bowel obstruction from an extra-intestinal primary tumor, often causing diffuse peritoneal studding and multiple points of obstruction.
🚩 Clinical Manifestations - Red Flag Rundown
| Emergency | Key Signs & Symptoms | Diagnostic Clues |
|---|---|---|
| SVC Syndrome | Facial/arm edema, plethora, JVD, dyspnea, cough, headache. 💡 Pemberton's sign (facial flushing on arm elevation). | Chest X-ray: widened mediastinum. CT chest with contrast is definitive. |
| MSCC | ⚠️ New/worsening back pain (esp. nocturnal/supine), radicular pain, motor weakness, sensory loss, saddle anesthesia, bowel/bladder dysfunction. | MRI of the entire spine is the gold standard. |
| MBO | Nausea, vomiting (bilious/feculent), abdominal distention, obstipation, colicky pain. Bowel sounds: high-pitched → absent. | Abdominal X-ray: dilated loops, air-fluid levels. CT abdomen confirms level/cause. |
⏱️ Diagnosis - Race Against Time
- Initial Steps: Rapid ABCs assessment, focused history (cancer type, prior treatments), and targeted physical exam (neurologic, vascular).
- Core Labs: CBC, CMP, coagulation panel, lactate. Consider tumor markers if relevant.
- Malignant Spinal Cord Compression (MSCC):
- MRI of the entire spine is the gold standard.
- Superior Vena Cava (SVC) Syndrome:
- CT chest with IV contrast to visualize obstruction.
- Malignant Bowel Obstruction (MBO):
- Initial: Abdominal X-ray (air-fluid levels).
- Definitive: CT abdomen/pelvis with contrast.
- Tumor Hemorrhage:
- Endoscopy, bronchoscopy, or angiography for localization.
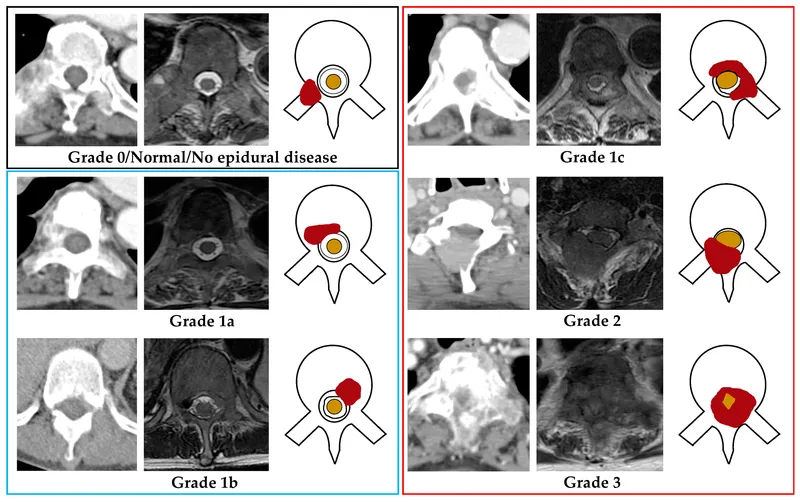
⭐ New-onset back pain in a known cancer patient, especially with neurologic symptoms (weakness, sensory loss, incontinence), is Malignant Spinal Cord Compression until proven otherwise.
⚔️ Management - Damage Control
A staged surgical strategy for exsanguinating patients (e.g., ruptured tumor), prioritizing physiology over immediate definitive repair. The goal is to interrupt the "Lethal Triad."
- Phase 1 Techniques:
- Hemorrhage: Perihepatic packing, vessel ligation/shunting.
- Contamination: Resection without anastomosis (staple off bowel).
- Phase 2 Goal: Restore physiologic reserve.
- Phase 3 Goal: Definitive anatomical repair and formal closure.
⭐ The "Lethal Triad" - Hypothermia (<35°C), Acidosis (pH <7.2), and Coagulopathy - is the primary indication. Each component potentiates the others, creating a vicious cycle that must be broken in the ICU.
⚡ Biggest Takeaways
- Spinal cord compression: Suspect in cancer patients with new back pain/neuro deficits. Get emergent MRI and give high-dose corticosteroids.
- SVC syndrome: Most often from lung cancer/lymphoma. Presents with facial/arm swelling. Treat with radiation and/or stenting.
- Malignant pericardial effusion/tamponade: Diagnose with echocardiogram; treat emergently with pericardiocentesis.
- Malignant bowel obstruction: Manage with NG tube decompression and consider surgical bypass or stenting.
- Acute airway obstruction: Requires emergent tracheostomy or endobronchial stenting/debulking.
- Massive tumor bleeding (e.g., hemoptysis): Control with angiographic embolization or surgery.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

