🕊️ Core Concept - Beyond the Cure
Palliative surgery aims to alleviate symptoms and improve Quality of Life (QoL) in patients with incurable, advanced cancer. It is not intended to be curative.
- Key Prerequisite: Patient's expected survival should significantly exceed the surgical recovery period (e.g., > 2-3 months).
- Decision Framework:
- Common Indications & Procedures:
- Obstruction: GI/biliary stenting, bypass (e.g., gastrojejunostomy), diverting colostomy.
- Bleeding: Resection, ligation, embolization.
- Pain: Debulking of a painful mass, neurolysis.
- Pathologic Fracture: Prophylactic fixation.
⭐ The primary endpoint for success in palliative surgery is symptom control and improved QoL, not overall survival.
📖 Management - The Palliative Playbook
Palliative surgery aims to relieve symptoms and improve Quality of Life (QoL) in incurable disease, not to cure. The core principle is balancing surgical morbidity against expected survival and potential benefit.
Common Indications & Procedures:
- Obstruction:
- GI: Bypass (gastrojejunostomy), diverting stoma (colostomy), or endoscopic stenting.
- Biliary: Stenting via ERCP/PTC or surgical bypass (choledochojejunostomy).
- Urinary: Percutaneous nephrostomy tubes or ureteral stents.
- Bleeding: Resection, angiographic embolization, or direct ligation of a bleeding tumor.
- Pain: Debulking of a painful mass, stabilization of pathologic fractures (internal fixation).
- Fistula/Perforation: Surgical diversion or repair.
⭐ High-Yield: Patient selection is paramount. A good candidate typically has an expected survival > 2-3 months and a reasonable performance status (e.g., ECOG ≤ 2).
Decision-Making Flow:
🎯 Clinical Manifestations - Symptom Relief Targets
-
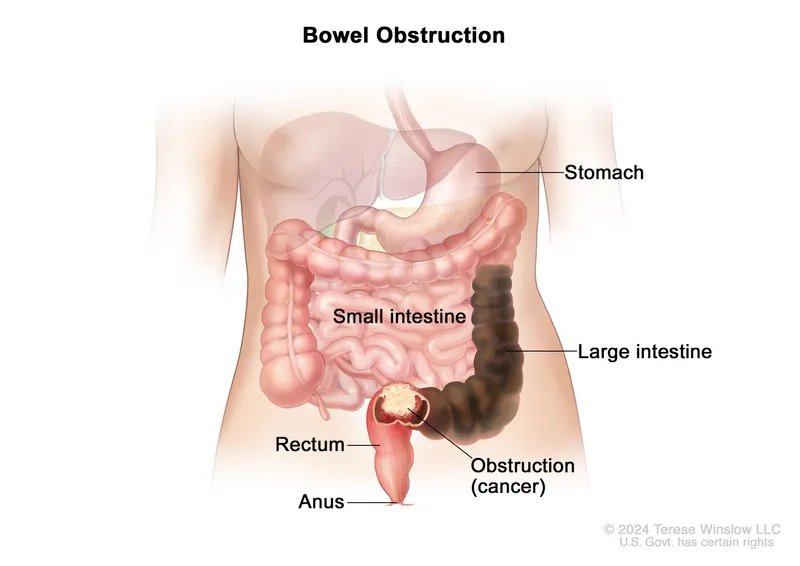
Obstruction: Most common indication for palliative surgery.
- GI Tract: Malignant bowel obstruction (MBO), gastric outlet obstruction (GOO), esophageal dysphagia.
- Procedures: Endoscopic stenting, surgical bypass (e.g., gastrojejunostomy), diverting stoma (colostomy/ileostomy), palliative resection/debulking.
- Biliary Tree: Obstructive jaundice, pruritus, cholangitis.
- Procedures: ERCP with stenting, percutaneous transhepatic cholangiography (PTC) with drainage.
- Urinary Tract: Ureteral obstruction causing hydronephrosis, renal failure.
- Procedures: Ureteral stenting, percutaneous nephrostomy tube.
- GI Tract: Malignant bowel obstruction (MBO), gastric outlet obstruction (GOO), esophageal dysphagia.
-
Bleeding: From ulcerated tumors (e.g., GI, lung).
- Procedures: Palliative resection, vessel ligation, angiographic embolization.
-
Pain:
- From nerve invasion, spinal cord compression, or pathological fractures.
- Procedures: Debulking, neurolysis (celiac plexus block), orthopedic stabilization (e.g., vertebroplasty).
-
Fistula / Perforation / Infection:
- Procedures: Abscess drainage, resection, diversion (stoma).
⭐ In malignant gastric outlet/duodenal obstruction, endoscopic stenting is preferred for patients with life expectancy < 2-3 months due to faster recovery, while surgical bypass (gastrojejunostomy) is considered for those expected to live longer (> 3-6 months) due to better long-term patency.
⚖️ Complications - Balancing Risks & Rewards
- Core Principle: Benefit (↑ Quality of Life) must significantly outweigh surgical risk and recovery burden.
- Key Risks: Standard surgical risks (bleeding, infection, VTE) are amplified by malignancy, malnutrition, and chemotherapy effects.
- Specific Concerns: Poor wound healing, anastomotic leaks, prolonged ileus.
⭐ A patient's pre-operative performance status (e.g., ECOG, Karnofsky) is a primary predictor of post-operative morbidity and mortality in palliative surgery.
⚡ Biggest Takeaways
- Palliative surgery's goal is symptom relief and improved quality of life (QoL), not cure.
- Common indications: malignant bowel/biliary obstruction, hemorrhage, or intractable pain.
- Crucial patient selection: must have adequate performance status and life expectancy (typically > 3 months) for benefits to outweigh surgical risks.
- Procedures aim for minimal morbidity: examples include stenting, bypass, diversion (colostomy), and debulking.
- Shared decision-making regarding goals of care is essential.
- Prophylactic fixation of impending pathologic fractures preserves function.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

