🤝 The Cancer Dream Team
- Multidisciplinary Team (MDT) / Tumor Board: A collaborative group of specialists who jointly manage cancer patients, representing the modern standard of care.
- Primary Goal: To develop a comprehensive, individualized treatment plan by reaching a consensus on diagnosis, staging, and the optimal sequence of therapies.
- Core Members (📌 SMRRP):
- Surgical Oncologist: Manages surgical resection.
- Medical Oncologist: Administers systemic therapy (chemo, immunotherapy).
- Radiation Oncologist: Delivers local radiation therapy.
- Radiologist: Interprets imaging for staging.
- Pathologist: Provides tissue diagnosis & molecular profiling.
- Key Ancillary Support: Palliative care, genetics, social work, nutrition, oncology nursing.
⭐ High-Yield: The MDT approach is strongly associated with improved survival, better adherence to evidence-based guidelines, and increased patient enrollment in clinical trials.
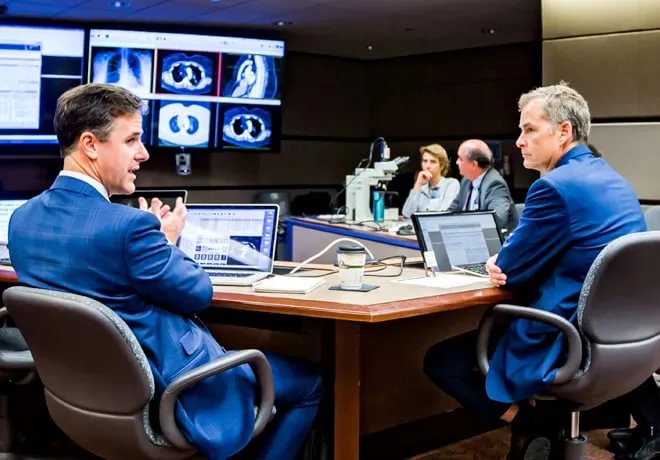
🤝 Management - The Tumor Board Huddle
A regularly scheduled meeting where a multidisciplinary team (MDT) discusses individual cancer cases to formulate a consensus treatment plan. It is the cornerstone of modern, patient-centered oncologic care.
-
Key Objectives:
- Establish accurate diagnosis & staging.
- Develop evidence-based, personalized treatment plans.
- Improve inter-specialty communication & coordination.
- Increase enrollment in clinical trials.
- Ensure adherence to NCCN/ASCO guidelines.
-
Core Participants:
- Surgical Oncologist
- Medical Oncologist
- Radiation Oncologist
- Radiologist
- Pathologist
- Nurse Navigator / Coordinator
- Palliative Care, Genetics, Social Work (as needed)
⭐ Multidisciplinary tumor board review can alter the diagnostic, staging, or treatment plan in 10-40% of cancer cases, significantly improving adherence to clinical guidelines and patient outcomes.
Tumor Board Workflow:
💡 The surgeon's input is crucial for determining resectability and the optimal sequence of surgery with neoadjuvant or adjuvant therapies.
🚧 Complications - Communication Breakdowns
- Root Causes of Failure:
- Lack of standardized handoffs (e.g., SBAR, I-PASS).
- Information silos from non-integrated Electronic Health Records (EHRs).
- Hierarchical culture discouraging junior members from speaking up.
- Time constraints leading to rushed or incomplete exchanges.
- Diffusion of responsibility ("bystander effect" in a clinical team).
- Clinical & System Consequences:
- ⚠️ Medical Errors: Medication mistakes, treatment delays, diagnostic inaccuracies.
- Conflicting information given to patients, causing confusion and anxiety.
- Fragmented care plans with poor execution and follow-up.
- ↓ Patient satisfaction and ↑ provider burnout.
⭐ The Joint Commission estimates that communication failures are a root cause in over 70% of sentinel events (e.g., wrong-site surgery, unexpected death).
⚡ Biggest Takeaways
- Multidisciplinary Teams (MDTs) or Tumor Boards are the standard of care for most cancers.
- Core members: surgeons, medical/radiation oncologists, pathologists, radiologists.
- Goal: Create a comprehensive, individualized treatment plan.
- Improves patient outcomes, adherence to guidelines, and clinical trial enrollment.
- Key decisions: accurate staging, assessing resectability, and sequencing therapies (neoadjuvant vs. adjuvant).
- Promotes shared decision-making with the patient, improving care coordination.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

