🎯 Core Principles - The Sentinel Hunt
The Sentinel Lymph Node (SLN) is the first lymph node to receive lymphatic drainage from a primary tumor. Its histological status predicts the status of the entire regional nodal basin, guiding decisions on further axillary lymph node dissection (ALND).
- Lymphatic Mapping Techniques:
- Blue Dye: Isosulfan blue (or methylene blue) is injected peritumorally. It stains lymphatic channels and the SLN blue for direct visual identification. ⚠️ Risk of anaphylaxis with isosulfan.
- Radiotracer: Technetium-99m ($^{99m}$Tc) sulfur colloid is injected, localizing in the SLN. Detected intraoperatively with a handheld gamma probe.
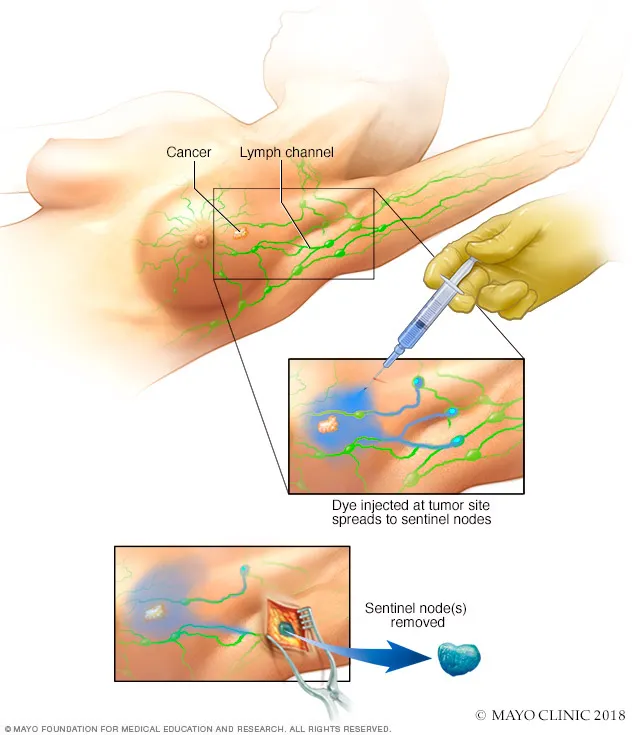
⭐ The dual-tracer technique (blue dye + radiocolloid) is the gold standard, maximizing the SLN identification rate to >95% in melanoma and breast cancer.
🔪 Management: Biopsy vs. Dissection
Decision-making for regional lymph nodes hinges on clinical status. The goal is accurate staging with minimal morbidity.
| Feature | Sentinel Lymph Node Biopsy (SLNB) | Axillary/Regional Lymph Node Dissection (ALND/RLND) |
|---|---|---|
| Indication | Clinically node-negative (cN0) disease | Clinically node-positive (cN+) or SLNB-positive disease |
| Goal | Staging (diagnostic) | Therapeutic & Staging (locoregional control) |
| Extent | Removal of 1-3 "sentinel" nodes | Removal of a larger group of nodes (e.g., Level I/II axillary) |
| Morbidity | Low | High |
| Complications | ↓ Lymphedema, ↓ nerve injury | ↑ Lymphedema (~20-30%), ↑ nerve injury, shoulder dysfunction |
⭐ ACOSOG Z0011 Trial: In early-stage breast cancer (T1/T2, cN0) with 1-2 positive sentinel nodes undergoing lumpectomy and whole-breast radiation, ALND shows no survival benefit over SLNB alone.
⚠️ Complications - Post-Op Perils
- Lymphedema: Chronic, non-pitting edema in the ipsilateral arm from impaired lymphatic drainage.
⭐ Lymphedema risk is significantly lower with Sentinel Lymph Node Biopsy (SLNB) (
5%) compared to Axillary Lymph Node Dissection (ALND) (20-30%). - Nerve Injury:
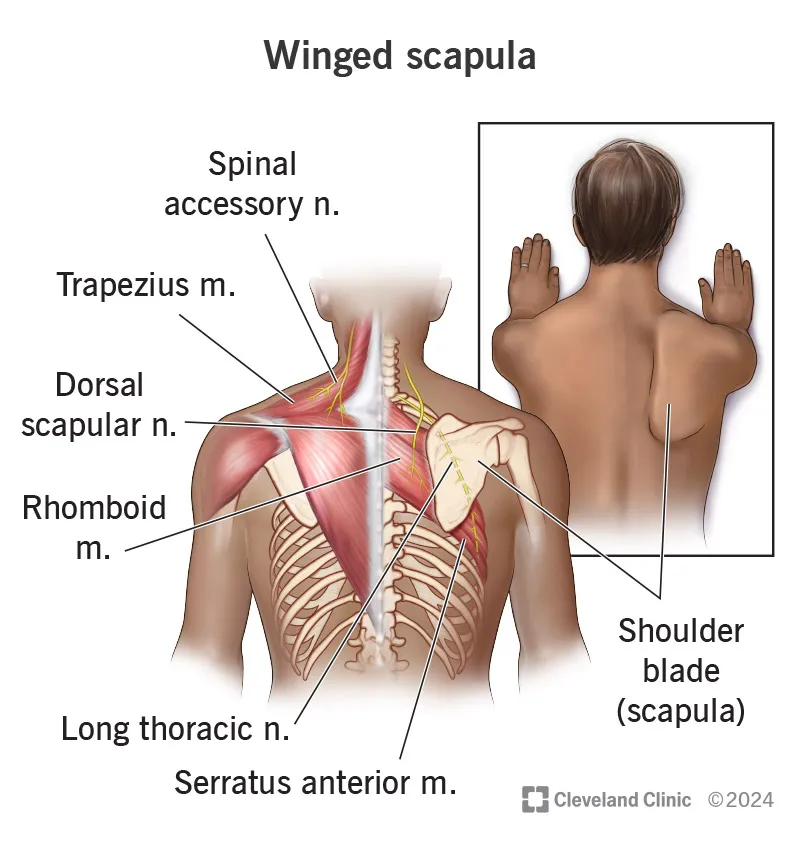
- Long Thoracic n.: Innervates serratus anterior → Injury causes "Winged Scapula".
- Thoracodorsal n.: Innervates latissimus dorsi → Injury causes weak arm adduction & internal rotation.
- Intercostobrachial n.: Sensory nerve → Injury causes numbness of medial arm/axilla.
- Seroma: Fluid collection in surgical dead space; may require aspiration.
- Shoulder Dysfunction: Pain, stiffness, ↓ range of motion.
📊 Clinical Correlations - Staging Significance
- TNM Staging: Lymph node status is the 'N' in TNM staging ($N_x, N_0, N_1-N_3$), a powerful independent prognostic factor for most solid tumors.
- Prognosis: Node positivity (N+) significantly worsens prognosis and increases the risk of distant recurrence.
- Adjuvant Therapy: A positive node finding is a primary driver for recommending adjuvant systemic chemotherapy and/or regional radiation therapy (XRT).
- Decision Impact: The number and anatomic level of positive nodes determine the specific N-stage, guiding treatment intensity.
⭐ For many cancers (e.g., breast, colon), the absolute number of positive lymph nodes is a more powerful predictor of survival than the size of the primary tumor (T-stage).
⚡ Biggest Takeaways
- Sentinel Lymph Node Biopsy (SLNB) is the standard for staging clinically node-negative breast cancer and melanoma.
- It identifies the first draining lymph node(s) using a radiotracer (technetium-99m) and/or blue dye.
- A negative SLNB avoids a more morbid Axillary Lymph Node Dissection (ALND).
- ALND is indicated for positive SLNB or clinically palpable, biopsy-proven nodes.
- Major ALND risk is chronic lymphedema; also nerve injury (long thoracic, thoracodorsal).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

