💃 The Debulking Dance
- Goal: Surgical removal of maximal visible tumor mass (cytoreduction). Aims to enhance efficacy of subsequent chemotherapy or radiation.
- Mechanism: ↓ tumor burden, removes chemo-resistant cores, and ↑ drug penetration into smaller residual nodules.
- Key Metric: Residual Disease (RD)
- Optimal: RD < 1 cm. Correlates with improved survival.
- Suboptimal: RD > 1 cm.
- Classic Indication: Advanced epithelial ovarian cancer. Also used for peritoneal mesothelioma and pseudomyxoma peritonei.
⭐ The volume of residual disease post-surgery is the most critical prognostic factor in advanced ovarian cancer. The goal is "optimal" debulking (< 1 cm).
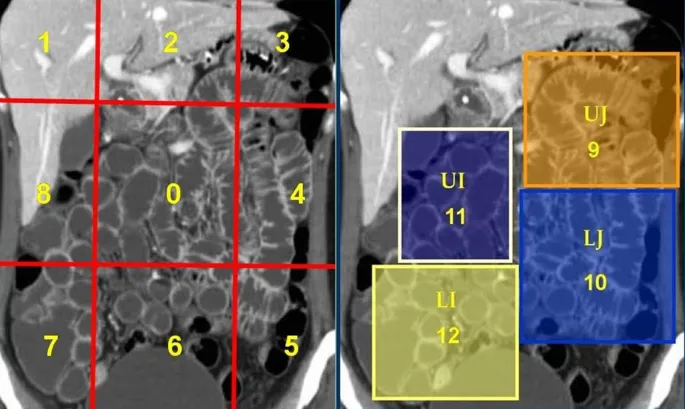
🔬 Pathophysiology - Rationale & Indications
- Core Rationale: To surgically reduce the macroscopic tumor burden ("debulking"). This enhances the efficacy of subsequent systemic or regional chemotherapy (e.g., HIPEC).
- Mechanism: Smaller residual tumor volume allows for better drug penetration, targets rapidly dividing cells, and decreases the likelihood of developing resistant clones.
- Primary Indications: Peritoneal surface malignancies where disease is confined.
- Ovarian Cancer
- Pseudomyxoma Peritonei
- Peritoneal Mesothelioma
- Select Colorectal & Appendiceal Cancer with peritoneal mets
⭐ The goal is complete cytoreduction (CC-0), leaving no visible residual disease. This is the single most important prognostic factor for survival.
🎯 Patient Selection Criteria
- Physiologic Fitness:
- Good performance status (ECOG 0-1).
- No severe comorbidities; able to tolerate major surgery.
- Tumor Biology:
- Favorable histology (e.g., low-grade appendiceal, mesothelioma).
- Chemo-sensitive disease.
- Disease Extent & Resectability:
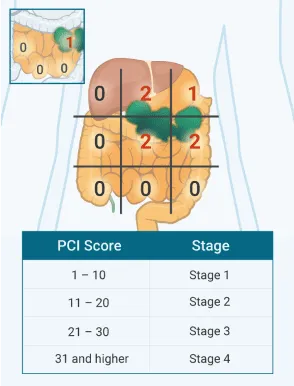
- Low volume of disease (low Peritoneal Cancer Index - PCI).
- No extensive/unresectable extra-abdominal metastases.
- No deep parenchymal liver/lung metastases.
⭐ The goal of CRS is complete cytoreduction (CC-0/CC-1), leaving no or minimal (<2.5 mm) residual disease. The Peritoneal Cancer Index (PCI) score is critical for predicting resectability.
🔪 CRS + HIPEC Technique
-
Goal: A two-pronged attack to eradicate macroscopic (CRS) and microscopic (HIPEC) peritoneal disease.
-
Procedure Steps:
- Cytoreductive Surgery (CRS): Meticulous surgical removal of all visible tumor implants (peritonectomy, organ resections).
- HIPEC: Intraoperative "chemo bath" with agents like Mitomycin C or Cisplatin, heated to 41-43°C and circulated for 60-90 minutes.
- Heat enhances drug penetration and provides direct cytotoxic effects.
⭐ The single most important prognostic factor for long-term survival is the Completeness of Cytoreduction (CC score). A CC-0 score (no visible residual disease) is the goal.

⚠️ Complications - The Price of Progress
- High morbidity (30-50%) & mortality (2-5%) risk; correlates with procedural extent (PCI) and patient comorbidities.
- GI: Prolonged ileus, anastomotic leak, enterocutaneous fistula, pancreatitis, chyle leak.
- Systemic: High risk of VTE (DVT/PE), ARDS, AKI, sepsis/SIRS.
- HIPEC-Specific: Profound myelosuppression (neutropenia), electrolyte abnormalities (↓Mg, ↓K), renal toxicity.
⭐ Anastomotic leak is a major driver of mortality. Suspect with fever, tachycardia, and leukocytosis around post-op day 5-7.

⚡ Biggest Takeaways
- Cytoreductive surgery (CRS), or debulking, aims to remove all gross visible tumor, not for cure but to improve efficacy of subsequent therapy.
- The primary goal is "no gross residual disease" (R0/R1 resection); R2 resection (visible tumor left) has poor outcomes.
- Completeness of cytoreduction is the single most important prognostic factor for survival.
- Commonly used for peritoneal surface malignancies like ovarian cancer and pseudomyxoma peritonei.
- Often combined with Hyperthermic Intraperitoneal Chemotherapy (HIPEC).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

