🦴 Backbone Bonding Basics
- Goal: Achieve arthrodesis (bony fusion) between vertebrae to eliminate motion, providing stability and pain relief for conditions like spondylolisthesis or severe degenerative disc disease.
- Key Components:
- Bone Graft: The biological "glue" for fusion.
- Autograft: Iliac crest (gold standard); osteoinductive & osteoconductive.
- Allograft: Cadaveric bone; osteoconductive only.
- Instrumentation: Pedicle screws, rods, and cages provide immediate mechanical stability while fusion occurs.
- Bone Graft: The biological "glue" for fusion.
⭐ Pseudoarthrosis (failed fusion) is a major complication, presenting as persistent or recurrent pain post-operatively.
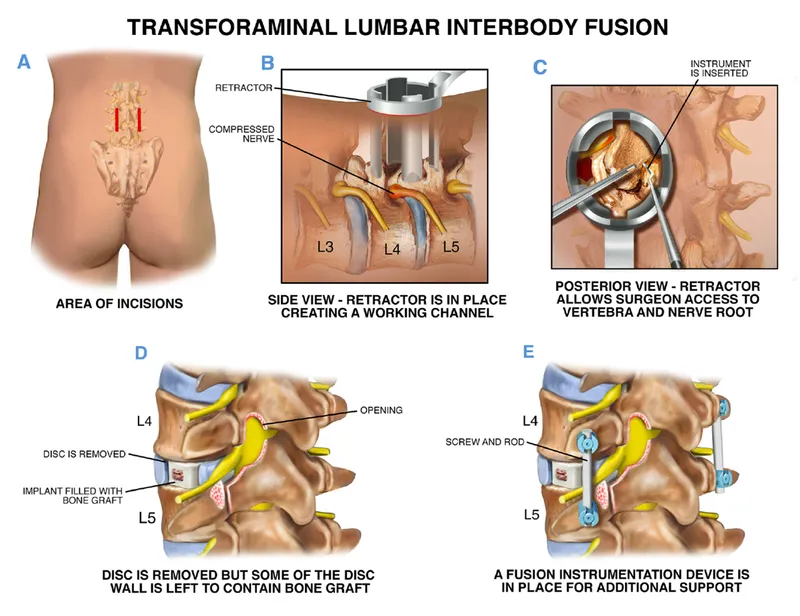
🔩 Clinical Manifestations - When Spines Need Support
- Spinal Instability: Pathologic motion causing pain or neurologic deficit.
- Traumatic: Unstable fractures (e.g., Chance, burst fractures).
- Neoplastic: Vertebral body tumors causing structural compromise.
- Infectious: Spondylodiscitis (e.g., Pott's disease) leading to collapse.
- Iatrogenic: Post-extensive laminectomy.
- Deformity:
- Progressive or painful scoliosis/kyphosis.
- Spondylolisthesis (vertebral slip), especially high-grade (>50%).
- Degenerative Disease (Refractory):
- Degenerative Disc Disease with severe, disabling axial back pain.
- Spinal stenosis with associated instability.
⭐ Fusion is indicated for progressive neurologic deficits (myelopathy, radiculopathy) or intractable pain from mechanical instability, not just for pain alone.
🔩 Management - The Fusion Fix-Up
The primary goal is arthrodesis (bony fusion) to stabilize painful or unstable spinal segments, eliminating motion.
Procedural Flow:
Approaches & Materials:
- Surgical Paths: Anterior (ALIF), Posterior (PLIF/TLIF), Lateral (XLIF).
- Bone Graft:
- Autograft (Iliac Crest): Gold standard; osteogenic, -inductive, & -conductive.
- Allograft: Cadaveric; mainly osteoconductive.
- Synthetics: e.g., BMPs; avoid donor site morbidity.
- Hardware: Pedicle screws & rods provide immediate rigid fixation.
⭐ Pseudoarthrosis (failed fusion) is a key long-term complication, presenting as persistent axial pain. Smoking is a major modifiable risk factor.
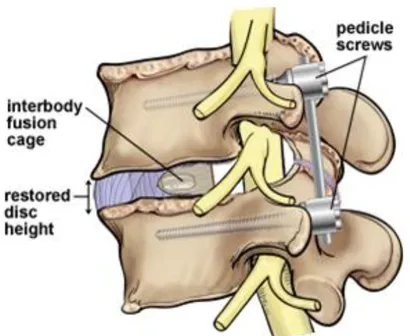
⚠️ Complications - When Fusion Goes Foul
- Intraoperative:
- Nerve root injury → new/worsened radiculopathy.
- Dural tear → CSF leak (postural headaches).
- Vascular injury (e.g., great vessels in anterior approaches).
- Postoperative (Early):
- Surgical Site Infection (SSI): Superficial or deep (discitis/osteomyelitis).
- Epidural hematoma → progressive neuro deficit (⚠️ surgical emergency).
- Postoperative (Late):
- Hardware Failure: Screw malposition, breakage, cage migration.
- Pseudoarthrosis: Non-union/failed fusion; persistent pain.
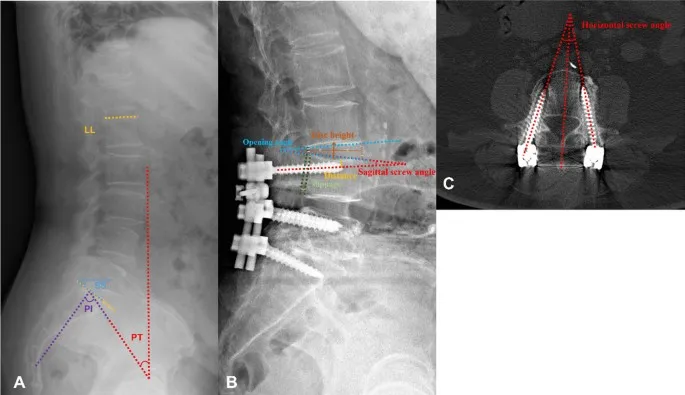
⭐ Adjacent Segment Disease (ASD): A key long-term risk. Fusing a segment increases biomechanical stress on the mobile levels above and below, leading to accelerated degeneration, new stenosis, or instability requiring further surgery.
☢️ Radiology - Peeking at the Plates
- X-ray (AP/Lateral/Flexion-Extension): Initial check for alignment, hardware integrity, and instability.
- CT Scan: 🥇 Gold standard for evaluating bony fusion (arthrodesis). Best modality to visualize pseudarthrosis (failed fusion).
- MRI: Assesses soft tissues. Indicated for new/worsening neurologic deficits to rule out hematoma, abscess, or persistent nerve compression.
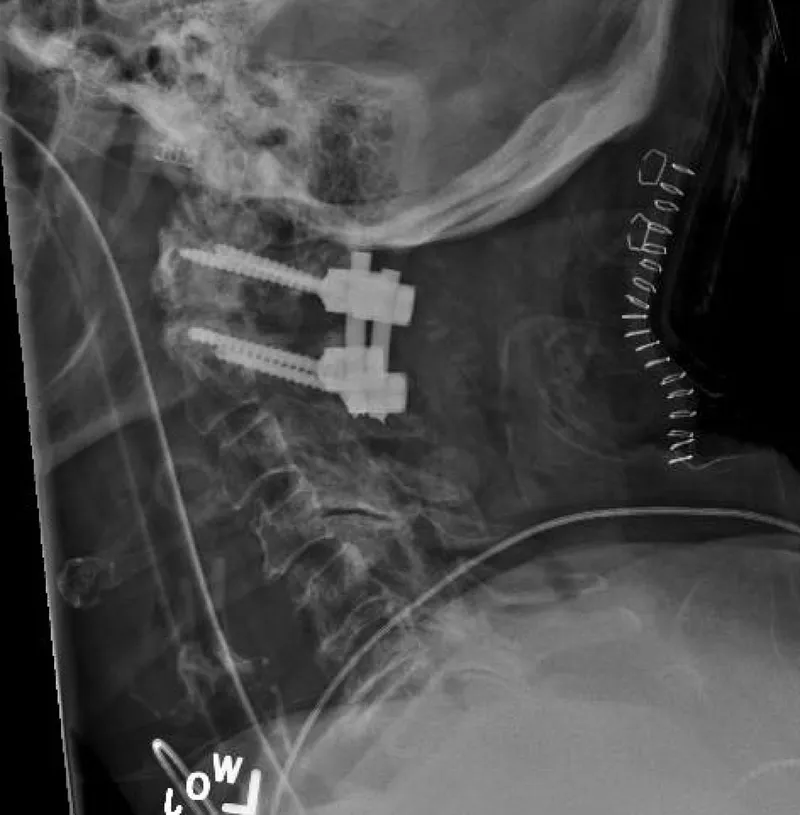
⭐ Pseudarthrosis: A key complication seen as a radiolucent gap at the fusion site on CT, often with motion on dynamic X-rays. It's a major cause of "failed back surgery syndrome."
⚡ Biggest Takeaways
- Goal: Stabilize the spine via arthrodesis (bony fusion) for instability, spondylolisthesis, or severe degenerative disease.
- Technique: Combines bone graft to stimulate fusion with instrumentation (screws, rods) for immediate immobilization.
- Key failure: Pseudarthrosis (failed fusion) is a primary cause of persistent pain, often requiring revision surgery.
- Long-term risk: Adjacent Segment Disease (ASD)-accelerated degeneration of levels next to the fusion due to altered biomechanics.
- Post-op warning: Avoid NSAIDs as they inhibit bone healing, increasing non-union risk.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

